My entire world was turned upside down in 2012 after my daughter was born 17 weeks early. She weighed 1 pound and 4 ounces (just over 565 grams) and was not even as long as a ruler. I was thrust into the world of prematurity — a world most people barely know exists.

I was forced to learn acronyms I had never heard before and educate myself on the hundreds of side effects and disorders my daughter may or may not fall victim to, all because she was born far too early.
Because this was so confusing to me — at a time when I was both emotionally and physically vulnerable, in addition to being overwhelmed and sleep-deprived — I decided to put together a list of some common terms that parents of premature (and full-term but sick) babies will hear after being admitted to the NICU.
- Apnea — The temporary cessation (stopping) of breathing for a period of 15 to 20 seconds or more, especially during sleep.
- Bagging — Manually pushing oxygen from a resuscitation bag into a baby’s lungs through a special mask placed over the nose and mouth.
- Blood Gas — A blood test that assesses the acid/base balance and oxygenation level in the blood.
- BPD (Bronchopulmonary dysplasia) — A serious lung condition that is a result of tissue damage to the lungs from being on a mechanical ventilator or other oxygen support for an extended period of time.
- Bradycardia — A slower-than-normal heartbeat that can cause a drop in the baby’s blood oxygen level.
- Corrected Age — Your baby’s age based on his due date, not the actual date of birth (which can be important for developmental milestones).
- CPAP (Continuous positive airway pressure) — A plastic tube inserted through the nose that blows air, or an air–oxygen mix, in and out of the lungs under pressure.
- ET Tube (Endotracheal tube) — A tube that is inserted through the mouth down into the trachea to deliver oxygen or assist with breathing.
- Extubation — The removal of the ET tube; this sometimes happens by accident during medical interventions.
- Gavage Feedings — A way to provide breast milk or formula directly to your baby’s stomach through a feeding tube inserted through the mouth or nose.
- Isolette — A self-contained incubator unit that provides a controlled heat, humidity and oxygen microenvironment for the isolation and care of premature and sick babies.
- IVH (Intraventricular hemorrhage) — Bleeding into the normal fluid spaces (ventricles) within the brain; this can range from grade 1 to 4, with 4 being the most severe.
- Micro Preemie — A baby born before 26 weeks’ gestation or weighing under 1 pound and 12 ounces.
- Nasal Cannula — A device used to deliver supplemental oxygen (through a tube in the nose) to babies in respiratory distress.
- NEC (Necrotizing enterocolitis) — A serious intestinal infection in premature babies that requires invasive surgery and is considered a medical emergency.
- NICU (Neonatal Intensive Care Unit) — A section of the hospital where hospital staff care for babies who have been born prematurely or with medical complications.
- NPO — An abbreviation for a Latin phrase that means “nothing by mouth” (no food or water).
- PDA (Patent ductus arteriosus) — A condition leading to abnormal blood flow between two of the major arteries connected to the heart (the aorta and the pulmonary artery), which can be common in premature babies.
- PICC (Peripherally inserted central catheter) — A long plastic tube placed into a large vein in the upper arm that is guided up into a large vein near your child’s heart to deliver medications.
- PIP (Premature infant pain profile) — A pain management plan based on behavioral and physiological body reactions, like crying and facial expressions.
- Pneumothorax — A collapsed lung, which is caused by one or more alveoli (air sacs) rupturing and releasing air into the chest cavity.
- RDS (Respiratory distress syndrome) — A condition common in premature babies characterized by trouble breathing on their own due to underdevelopment of the lungs.
- ROP (Retinopathy of prematurity) — A condition that causes abnormal blood vessels and scar tissue to grow over the retina and make it difficult for the babies to see clearly or at all.
- Surfactant — A substance that babies over 32 weeks’ gestation naturally produce to allow their lungs to remain open. However, premature babies don’t have sufficient amounts of operational surfactant and must be given doses of it soon after breathing is stabilized to help their lungs function properly.
- TPN (Total parenteral nutrition) — An intravenous solution of protein, fat and carbohydrates designed to give babies the nutrients they were unable to get from their mothers.
My daughter’s NICU care included 23 of these 25 terms, and some were quite serious. She spent 121 days in the NICU, the first 40 of which were extremely rough. I was not able to hold her until she was over a month old because of the severity of her conditions. They left her very unstable and unable to be taken out of her isolette or “artificial womb.”
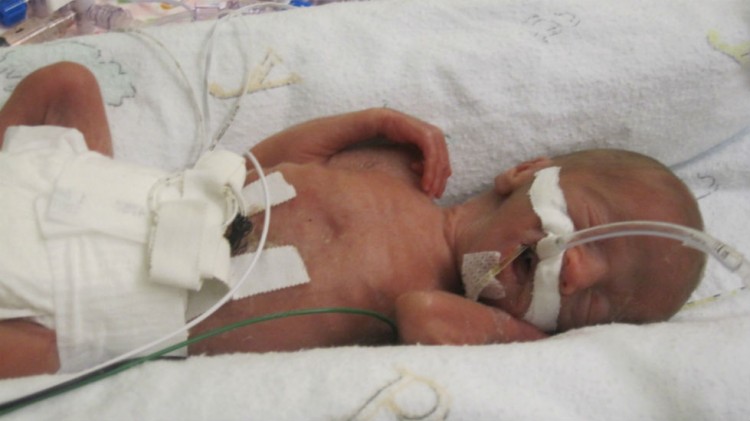
Every premature baby is different and will travel down a different road both during and after his or her NICU stay. One 23-weeker (like my daughter) will not necessarily have the same procedures and problems as another.
I could get into all of the medical interventions she endured during her first few months of life and the numerous times we thought we were going to lose her, but that’s not as important as the fact that she made it out of the NICU and came home to our family.
My daughter is now a healthy and happy 3-year-old who loves to watch “Dora the Explorer” and wear tiaras. She is the princess of the house and the boss of her three older brothers (plus me and my husband, too!).
While she is left with BPD (now you know what that is!) and a few other side effects of her extreme premature birth, she manages to enjoy her life to the fullest.
Just recently, she saw a picture of herself in her isolette in the NICU and asked me, “Why was I in the hospital?” I answered, “Because you were born too little and too early.” She then laughed and said, “That’s silly, I’m so big now!”
As parents of premature babies, we are comforted to know that our babies will never remember the hundreds of medical interventions they endured to be with us today.
However, as parents of premature babies, we will never forget!
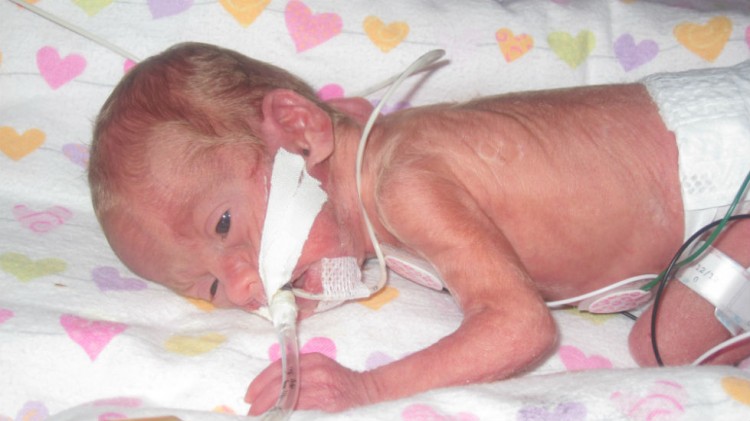
Please share this with anyone who may be experiencing a high-risk pregnancy or has experienced a premature birth, as it’s helpful to be prepared for the medical terms that may be thrown your way.
Did I miss any terms?
Follow this journey on Micropreemie.net.
The Mighty is asking the following: Tell us about a time someone in your community went above and beyond (or did the exact opposite) for you or your loved one with special needs. If you’d like to participate, please send a blog post to community@themighty.com. Please include a photo for the piece, a photo of yourself and 1-2 sentence bio. Check out our Submit a Story page for more about our submission guidelines.
