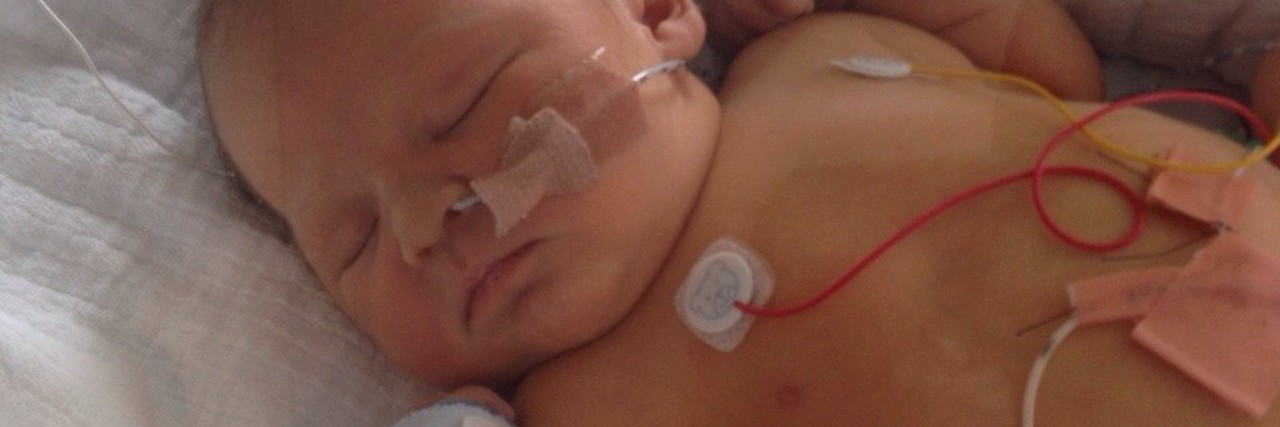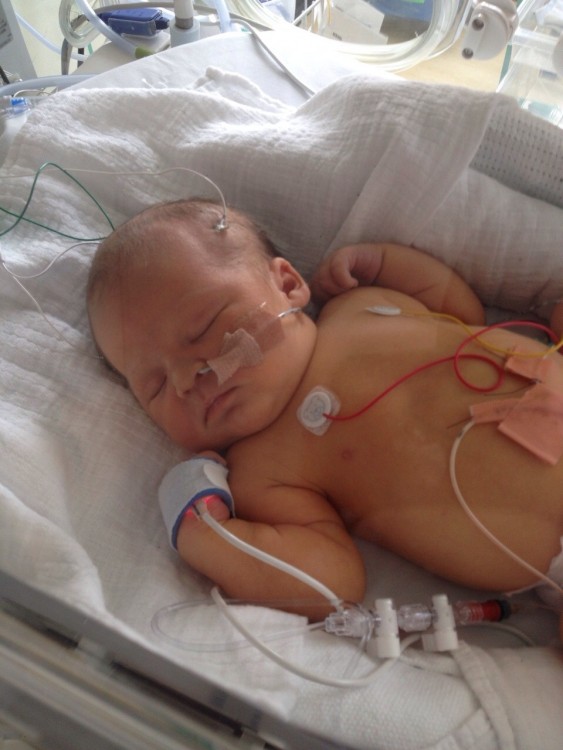
There are many articles and posts that others have written about “How to survive your time in NICU.” I am not sure “survive” is the correct term. Did my baby and me “survive” NICU? Yes, we did. But my time as a NICU mum didn’t end when we came home. Nor did it end when my son had follow up appointments or lifesaving surgery. Nor will it leave me when he will have to have yearly check-ups. It is still with me in the flashbacks, the nightmares, the memories and when I am talking about my son’s first few hours, weeks and months of life.
I want to help those who are finding themselves in the same position we did. I want to be honest, brutally honest about how we tried to cope. That is not to say you will be feeling the same, or you agree with what is being said. These are my personal opinions based upon the journey we took.
There are many reoccurring themes in the advice to those with babies in NICU and this is what I will try and give you my honest and realistic opinion on.
I have to say I was quite alarmed to find a “do’s and don’t’s” guide to surviving your time in NICU. Whatever you decide to do is right. If you do not really want to do something, that is OK. Everyone is different and some may not find the below useful; some may find it the best advice they have ever been given. The fact of the matter is, there is no right or wrong way to deal with this. It’s shit. It’s the worst time of your life. Do what you think is right and what you can to get through this. Nothing is wrong with that. This is not flat pack furniture we are talking about; this is your life.
The following were listed on many of the websites under the “Do” section:
Get to know the nurses. There will be a high staff turnover with day shifts and nights shifts, but if you are in there for a few days you will start to see familiar faces. The nurses from my experiences are normally happy to talk through everything they are doing and help out where they can. They will help explain what the doctors have said and advise on vouchers, accommodation issues, etc. They have seen this all before. They know how it works and they have some idea of how you feel. I found myself confiding in one nurse as it was easier than talking to my husband. Don’t feel like you have to though. They also respect the fact you may not want to talk. They will encourage you to look after yourself. At times I found this annoying but they were just looking out for me. Some of them you will not like or get on with, especially if you have a favorite (I did).
Ask if you can get involved in infant care. This includes nappy changes, bathing their eyes and mouth, etc. This will make you feel involved as a parent and will help. I treasure some of the moments where I was in charge of his feeds, his bum changes and taking his temperature. I felt like I was a normal mother.
I once went in when Elijah had been moved rooms, been fed, put back down and had been sick. No one had noticed and this annoyed me a lot. They were probably over stretched but I feel like you have to tell them if you’re not happy. Every step of the way with Elijah’s hospital appointments, op and various other bits I have always pushed for what I think is best. And you know what? I have always been correct in doing so to get the best for him. This is your baby — if you do not like something or how something is done, or if you want to take over something, tell them.
Take care of yourself and make time for yourself outside of hospital by taking breaks. This one is a hard one. Yes, you have to eat, shower (in Greg’s case smoke!) and it is good to get outside. I will warn you: even though you are away from them, you cannot stop thinking about them or how much time is left until you can go back next to them. My honest advice if you feel like you can’t leave them? Don’t. Eat something before you go in. Take a book for when they are asleep and sit, for as long as you want. If that’s what you feel you have to do, then do it.
Most hospitals have a “family room” attached where you can go sit, read a magazine or make a drink. We did not find these places very comfortable. They are filled with other, often anxious parents with emotions boiling over, and it was a time where we did not particularly want to be that social. Some of these articles tell you to befriend other NICU parents. I was still in complete denial that Elijah even had something wrong with him, so I found talking to other parents really difficult. I didn’t want to talk to my family or friends never mind anyone else. It’s all really hard to watch other parents be told about a setback, or when their baby is not getting better. I had a strange type of guilt I felt when my baby was doing so well and when we went home. It was even worse when one of the babies passed away. I felt why have I been able to take my baby home and they have cruelly lost theirs? It’s a hard situation to even get your head around.
We spent a lot of time walking around (well, I waddled) and sitting in the hospital restaurant people watching as a distraction. I did not particularly want to eat. I drank a lot of coffee, after nine months being caffeine free, I was pretty much hooked on filter coffee every day. As some sort of punishment, I used to not eat or eat as little as I could so I had some control over the situation were in. I felt so helpless. Eat as much or as little as you want. Sometimes you are so distraught the very thought of food makes you want to vomit. Try and eat small portions and often, even if it is a Crunchie from the hospital vending machine to keep your sugar up. I swore by Powerade — it helped keep my energy up without feeling like I was eating. Eventually, you get your appetite back. Just do what your body tells you. Although, when we were in there I think my mind had taken over and it was not my best ally.
Get involved in NICU activities and support groups. In the nine days we were in NICU, never once did I hear the word “activity.” If they had, I personally would not have partaken in them. I am not sure if they think having an arts and crafts table would help. It didn’t for me. There were chaplain and charity volunteers that come round to offer you support. Even now it is only after 18 months of leaving NICU can I even begin to process all this. I didn’t go to any support groups. Maybe I should have, but those sort of things are not for me. I was diagnosed with post-traumatic stress disorder (PTSD) and am on medication. It is only after time has now passed that I feel I can try and get some help and “move forward.” At the time, my focus was my baby.
Focus on the positives. Easier said than done, as I was in a very negative mind space. I was focused on something horrific happening after each bit of good news we had. I was overjoyed when each tube of Elijah’s came out and when he was allowed to start feeding. Small things make the world of difference and you will find yourself telling anyone that will listen that, “baby’s feed has been upped by 20 milliliters,” or “he is now allowed to wear a vest and is busy putting on weight.”

Bonding. Although Elijah was with me for 12 hours before he went to NICU, I was out of it for at least 10 of those, so I missed the first proper bonding moments. It is then quite hard to bond with a baby in an incubator covered in tubes and attached to every machine going. I always held his hand, something we still do even now if he has a rare nap on me. It’s a very intrusive time with medical staff, other babies, parents, equipment, noise, lights and cleaners being around. Therefore it may not seem like it, but every minute you spend with your baby is building a bond with them.
As soon as I could, I held him and we used to sit in a chair with him on my chest for what seemed like hours. I was not able to breastfeed, but if you do or if you’re pumping and expressing milk, this all builds to the bonding experience. The hospital actively encourages it. I still feel robbed of the precious bonding moments, and I often feel insanely jealous of those who get to go home on the same day, or even go onto the ward, but I tried. I had small knitted triangles the hospital gave me to keep in my bra so Elijah would be able to smell me. I used to leave a t-shirt of mine that smelled of my perfume in his incubator, and brought his teddies and dummies from home so it felt more like a proper crib. I felt like I was being a mother doing those things, as silly as that sounds.
Keep a written record. I did not keep a written record, as I didn’t particularly want to remember the horrendous time I was going through. Some may find it helpful to keep a journal or online blog as each day passes. Some of the days I just did not want to remember. We have lots of photos. Looking back now some of them are very hard for me to look at, but I want to show Elijah one day what he has overcome. Whatever helps you, do it. I once saw a woman knitting at her child’s bedside. If it keeps your mind distracted for just one moment, then in my opinion it is worth doing.
The following were listed on many of the websites under the “Don’t” section:
Note: I am still appalled there is a “don’t” guide for surviving your time in NICU. It is not like you’re going to not feel any of the below. It is natural and we should be accepting these feelings and not to be made to feel they are wrong.
Isolate yourself from your friends and family. I believe although people can try to understand and comfort you, unless they have been through it, they really do not understand what you are really feeling. You may not even want to admit what you are feeling: confusion, anger, resentment, loss of control, hurt, jealousy, worry — to name a few. That’s not to say they cannot provide comfort and support. Although I pushed them away, I had two amazing friends who did everything they possible could for my family when we were in hospital. From feeding my cats, to driving Greg to and from the hospital every day and even bringing me and my baby home for the first time. I can never thank them enough for what they did for us then and they are a huge part of my son’s life to this day. If you don’t want to talk to anyone, don’t. Let your partner update one or two friends and let them pass the message on to everyone. It can get quite overwhelming repeating the same update numerous times to everyone and then seeing the replies coming in can be quite emotional. If you want speak to everyone and have lots of visitors, have them. I couldn’t face anyone. I was ashamed and I felt like I did something wrong, like I couldn’t have a baby properly. Like I wasn’t a proper mother. I was clearly depressed, and dealing with a traumatic event. I dealt with it the only way I felt was right at the time, on my own.

Become discouraged with setbacks. This is actually what some lists tell you not to do. Of course you are going to be discouraged with setbacks. That’s your child. All you want for them is to be healthy and to be home. Anything stopping or delaying that is a setback. If you want to cry, then cry. If you want to scream, do it. You will be discouraged, of course you will. Accept it. That’s my advice and I believe it is far healthier than trying to pretend you are not anything but discouraged.
Feel guilty for not being at the hospital all of the time. Again, seriously? If you are not at the hospital, try and keep busy and remain focused on something. If you feel so guilty that you think it’s going to tear you up, then try to get back to the hospital if you are able. It’s not worth letting it eat away at you.
Most of the NICUs have a 24-hour policy anyway, so if you want to go back up at 3 a.m., do it. I spent as much time as I could, but I caught the flu and was unable to visit Elijah for two days. I was at home and my baby was 25 miles away. It was extremely challenging. There are so many other emotions going on, you need to make life as simple as you can and listen to how you feel. I wish I could go back and tell myself some of this, but hindsight remains a very beautiful thing.
I could go on and on about how you’re “supposed” to feel and what you’re “supposed” to do. At the end of the day this is your journey, and you must do what you think is right. If you feel something, even if it is negative, accept it. You’re obviously feeling it for a reason, and it’s a natural human reaction to the stressful situation you are in.
You’re doing great by the way, from a NICU mum who spent nine days in NICU with Elijah in September 2014.
Follow this journey on Confessions of a NICU Mum
The Mighty is asking the following: Create a list-style story of your choice in regards to disability, disease or mental illness. Check out our Submit a Story page for more about our submission guidelines.