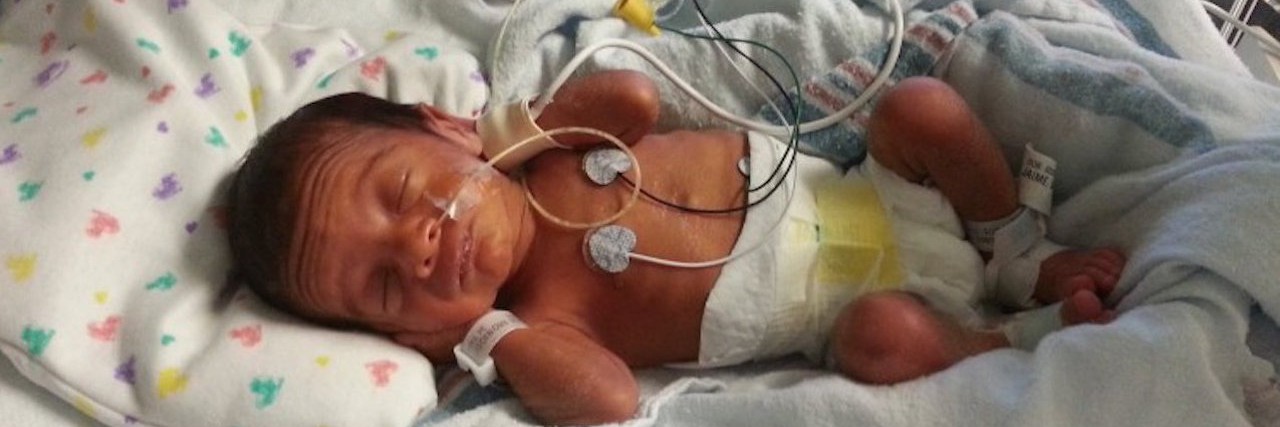
The NICU is an overwhelming place. The crash course happens so fast, especially when you go into premature labor.
You will immediately realize the NICU is home to many babies, each battling their own uphill battles. But from the onset, you’ll also realize NICU babies are the strongest, most resilient tiny creatures you ever laid your eyes upon, and they will forever change your perspective about the miracle of life. Preemies go through more pokes, surgeries and procedures than most adults will ever endure in their lifetime.
It’s both overwhelming and inspiring at once as you watch it all transpire. Here are eight things I learned during my babies’ time in the NICU:
1. Emotion will likely take over.
I was overcome with emotion every single time I walked into the NICU to visit my twin boys, Noah and Nikoh, who were born premature at 29 weeks. It was heartbreaking to see so many babies. Many were alone in their incubators, some babies had visitors, others were sound asleep and some were crying but waiting their “turn” to be tended to by the busy nurses. If you’re anything like me, the epitome of a first-time mom, you’ll likely shed lots of tears during your NICU journey.
2. Twin parents will master the “switch-off.”
Each time my husband and I would visit the NICU, we would walk over to our twins’ separate incubators. He’d go to one baby, and I’d go to the other. Their incubators were always positioned side-by-side so we could visit them both at the exact same time. We would stick our arms in their incubators, softly caress their little faces, touch their tiny hands and feet and whisper to them how proud we were of their progress and perseverance. A minute or two later, my husband and I would “switch,” so each of us could say hello and bond with our other baby. So was the case for all other parents of multiples in the NICU.
3. Sometimes you can only sit and stare.
For the first couple of days, our twins were too “unstable” for us to take them out of the incubators, so the majority of those first visits really consisted of us gazing into their incubators and imagining the moment we would get to hold them in our arms. It was heart-wrenching to be told we couldn’t hold our babies. Sitting and staring at them was torture during those first few days, but as a NICU parent, you have no problem sacrificing your emotions for what’s best for your baby’s development.
4. Nurse updates help.
At the start of each visit, we would get an update from the nurse who was taking care of our twins, including if they had gained weight, how they were tolerating their gavage feedings, had they been crying or uncomfortable, did their bilirubin levels rise or fall, were any episodes of apnea detected (which is common in premature babies and happens when the babies stop breathing) and had they experienced any bradycardia or “bradys,” which is a drop in a baby’s blood oxygen level as a result of apnea.
We were also updated on how well the babies were breathing. Both Noah and Nikoh were placed on a CPAP at birth, a respiratory support machine which gave them constant air flow to help them breathe and keep their tiny lungs from collapsing. The CPAP is a clear, thick tube, which was positioned tightly over each babies’ nose. It covered just about their entire faces and were very uncomfortable for them. It broke my heart to constantly see them try and tug on the CPAP mask. And although it was very faint, I often would hear them cry while they struggled to get comfortable with the CPAP covering their faces.
5. You’ll hear alarm bells in your sleep.
Alarms are a common sound in the NICU. Every time I would hear a monitor beep, which happened at least a dozen times an hour, my heart would sink and I’d quickly look at my twins’ monitors to check their blood pressure, heart rate, breathing, etc. The nurses explained what all the colors and numbers and sounds of the machines meant. That way when we heard the dreaded “ding, ding, ding,” we knew what was happening.
It was terrifying when the alarm was coming from one of our babies’ monitors, and it was a relief when it wasn’t. Emotional roller coaster, I tell ya! I would hear those alarm bells in our sleep, and I can still hear them in my head as I write this blog.
6. Expect to be intimidated.
It was a lot to learn, a lot to process and a lot to accept as a new NICU mom. I often felt intimidated talking to the nurses and doctors because they would talk in medical terms, and it was up to us as the parents to ask countless questions in order for us to really understand what was happening with our babies and their development. I felt intimidated when I didn’t fully understand something, but I quickly realized I was the biggest advocate for my twins and their development, so I got very comfortable asking as many questions as I needed in order to fully understand what was going on.
7. There will be triumphs and pitfalls.
Each day brought different triumphs and pitfalls for my twins, and it often seemed like when one of our babies had a really great day, the other baby was struggling in one area or another. My emotions were often divided down the middle — happiness and sadness — because my twins were always on “different pages,” medically speaking. It was rare that they ever had good days at the same time. The experience of having your heart divided for two children who were experiencing different things at the same time was incredible now that I look back on it. Parenthood gives you superhuman strength!
8. Trust is hard, but it gets easier.
Trusting the NICU nurses, who at first were strangers to me, with my underdeveloped, precious babies was the hardest thing I ever had to do. Looking back, I consider those NICU nurses our angels. They took care of our twins extremely well, and often spent time talking to us, parent to parent, to reassure us that one day we would be able to take our babies home.
Every NICU baby and parent will have different experiences and methods of coping. Lots of parents say after navigating early parenthood in the NICU they consider changing careers and becoming a NICU nurse. I know I contemplated it, mostly because my crash course in the NICU gave me new insight into how amazing premature babies are, and I have a newfound respect for the jobs NICU nurses do everyday.
I hope sharing a bit of what I experienced could serve as a general roadmap on what to expect if you find yourself and your baby in the NICU.
Follow this journey at reportertotwinmom.com.
The Mighty is asking the following: What’s one thing people might not know about your experience with disability, disease or mental illness, and what would you say to teach them? Check out our Submit a Story page for more about our submission guidelines.