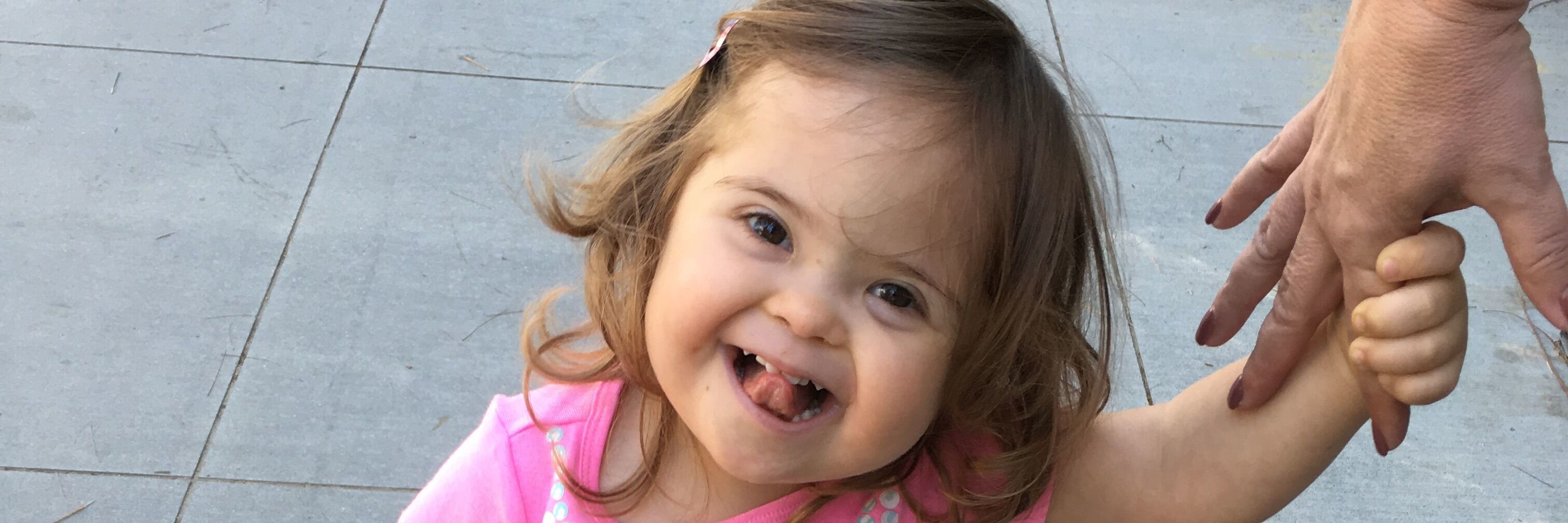
My daughter Leah was not quite 24 hours old when I overheard the pediatric surgical team discussing her case in the hallway of the neonatal intensive care unit. “Look at her — are we going to do a repair on this tiny baby? No — it will be at least five months before she’s ready.” Leah was born two months early, with Down syndrome, two holes in her heart, a congenital diaphragmatic hernia, and long-gap esophageal atresia, a rare condition in which a large portion of the esophagus is missing. She would not be able to leave the hospital until the esophagus was repaired. Her first surgery, to place a feeding tube directly into her stomach, took place when she was 2 days old and weighed just over three pounds.
Leah stayed in the ICU for seven months. We brought her home on oxygen, a feeding pump, steroid treatments via nebulizer, and methadone to wean her off of the extensive regimen of pain medications, sedatives and paralytics that had been required to immobilize her for nearly two weeks following her esophageal repair.
In the year after Leah came home, she averaged seven to 10 doctor and therapist visits per week and spent the equivalent of another month in short hospital stays. Today at almost 4 years old, Leah still relies heavily on her feeding tube, and requires hours of speech, occupational and physical therapy each week in addition to her preschool special day class. She has been in the operating room 21 times and has undergone 33 procedures during those OR trips.
Despite her complex and challenging medical history, Leah is a happy, beautiful and thriving little girl. She likes swing sets, Raffi, tea parties and “Frozen,” and she knows over 200 ASL signs and recognizes several letters of the alphabet. She is the queen of “Head, Shoulders, Knees and Toes,” and she can Hokey Pokey like that’s what it’s all about. We attribute much of her progress and good cheer to the fact that aside from hospitalizations for acute conditions, Leah has been able to live at home, with me as her primary caregiver.
Fifty years ago, a child like Leah would be condemned to lifelong institutionalization in a state-funded nursing home for the developmentally disabled — and that’s if the doctors made the effort to save her in the first place. As recently as the 1980’s, doctors famously convinced a couple to let their newborn with Down syndrome and esophageal atresia starve to death in the NICU because it was purportedly the “compassionate” choice. If a child with Leah’s conditions did survive infancy, she would be 100 percent reliant on care providers for the remainder of her life.
But it’s 2017, and Leah doesn’t live in a nursing home. Instead I take her to her countless weekly appointments; coordinate her medical care with multiple specialists; order and organize medical supplies and equipment; prepare and administer her g-tube feeds, medications, oxygen, and nebulizer treatments; follow home therapy regimens to reinforce her skills at home; monitor her caloric and fluid intake; assist her in oral feeds and watch closely for choking and “stuckies” (the EA parent’s nickname for food getting stuck in a child’s esophagus due to poor motility); advocate on her behalf with the regional center and the school district; and make sure she doesn’t pull out her g-tube or otherwise injure herself due to lack of safety awareness. I do the work of a nurse, a service coordinator, a social worker, a chauffeur, an executive assistant, and above all, a mom.
I am able to provide all of these services to keep Leah out of a nursing home because years ago, the government realized it could both save money and improve the lives of people with developmental disabilities by shifting resources away from institutionalization and toward providing home and community-based services, including in-home nursing and attendant care.
In California, these services are administered through In-Home Supportive Services (IHSS), a Medicaid program that provides home attendant care for the elderly and people with disabilities who are at risk of institutionalization, alongside state waivers that ensure that all people with developmental disabilities can access these programs.
When a parent is unable to work full time because of a child’s extraordinary needs, the parent can be paid (at minimum wage, mind you) as the child’s in-home attendant to provide services for needs that go above and beyond what is developmentally appropriate for a typical child of the same age. By allowing parents to be paid as care providers, the state saves money it would otherwise spend on institutionalization, parents keep a roof over their families’ heads, and children receive care in the environment that leads to the best long-term outcomes.
And it should go without saying that all else being equal, kids are better off living with their families than in nursing homes. Today, the average life expectancy has more than doubled for people with Down syndrome, a statistic partially attributable to improved outcomes for infants with heart defects, but surely also the result of not warehousing them out of sight in state homes. One only has to Google the term “Willowbrook State School” to see the conditions in which some children with disabilities lived only 50 years ago.
Today many adults with Down Syndrome are able to live independently or with the help of life-skills coaching and community supports, due in large part to publicly-funded early intervention services. This reduces the number of people who become dependent on the state for complete care as adults. Overall, home-care programs are a win for everyone involved — the government, the family, and the person with disabilities.
These vital programs are at risk in the face of current threats to Medicaid. The Senate’s proposed health care bill slashes funding to Medicaid across the board, and the proposed per-capita spending caps mean that the number of people who rely on Medicaid will grow faster than the amount of funding made available for it. This poses a huge threat for waiver programs that provide home-based care to the elderly and people with disabilities. If states lose huge portions of their federal Medicaid funding, they will be forced to come up with the difference themselves, and if the past is any indication, programs for people with disabilities will be first on the cutting block — particularly programs for children.
The last time California suffered a major budget crisis, state officials attempted to slash IHSS services by 20 percent. Supreme Court-mandated protections for people with disabilities kept California from successfully carrying out this cut, which would have led to institutionalization for thousands of Californians. This time around, the Supreme Court decision — which takes into account the State’s available resources – may not be enough to save Californians at risk of institutionalization.
Vice President Hubert Humphrey once said that “the moral test of government is how that government treats those who are in the dawn of life, the children; those who are in the twilight of life, the elderly; and those who are in shadows of life, the sick, the needy, and the handicapped.”
Right now, we are facing our nation’s greatest moral test in decades. For my daughter’s sake, I hope we pass the test.
Editor’s note: This story reflects an individual’s experience and is not an endorsement from The Mighty. We believe in sharing a variety of perspectives from our community.
We want to hear your story. Become a Mighty contributor here.