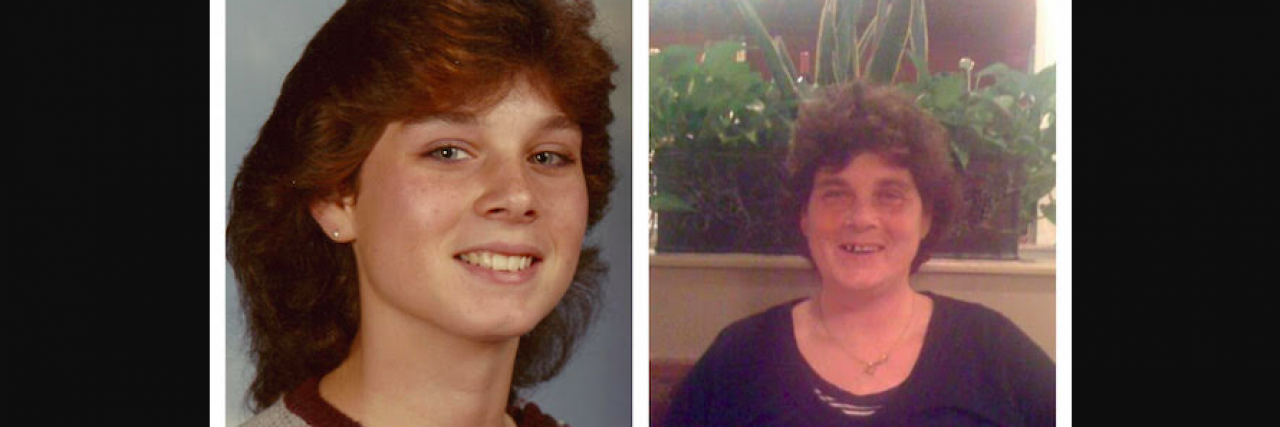My sister Regina was an outgoing, popular and beautiful spirit. In contrast, I was shy and awkward and — OK, I’ll say it — a bit nerdy. I always envied her social graces. But at the age of 16, she began to become “spacey.” We thought she might be experimenting with drugs, but the symptoms persisted and worsened over time. She began to neglect her appearance. She began to seem in a fog and disorganized. At this time I was away at college as a pre-med major. My father became increasingly alarmed and ultimately took her to see a doctor when she was wandering the halls of her high school in a complete daze, unsure of where she should be. She was hospitalized at a children’s psychiatric hospital, and when I returned home from college for a visit I could scarcely believe the transformation.
She barely recognized me. She was sedated on medication with horrible side effects. The light in her eyes had gone out. She stayed in the hospital for a year, and I changed my major from pre-med to psychology. The doctors were throwing out the label “schizophrenia” at the time, and I had only the most basic understanding of that illness. Helpless, I watched as Regina’s life became a series of hospitalizations. I was devastated.
After graduating from college I worked in an adolescent psychiatric ward, trying to desperately help others while working through the grief that I couldn’t help her. I ultimately did follow my dream to go to medical school. When I was in residency (working more than 80 hours a week), I received a phone call that Regina was in an emergency room in New York and might not survive. I called the ER and spoke with her nurse, who told me they were treating her for cardiac Lyme disease. I was dumbfounded. Regina wasn’t the type to tramp through the woods collecting ticks, how could she have contracted Lyme disease? It never even occurred to me that the ER staff were not appraised of her medications. The actual problem was that her lithium (one of the medication she was taking at the time) was at toxic levels. Without the insight to explain to them she was taking medication, my sister was being treated for the wrong thing.
I flew up to New York and burst out in tears when I saw her. I resolved I would bring her to North Carolina to come live with me so this could never happen again. A few months later she moved in with me. Of course, I bit off more than I could chew in my zealousness. She became floridly psychotic and paranoid, unsafe to leave alone (and I was working 80 hour work weeks doing a residency in internal medicine). With the help of the social workers, I found out about resources in the community, and was referred to the Sanctuary House, a nonprofit that offers services for adults living with mental illness.
The Sanctuary House was a lifesaver. She shined there, made friends and became socially engaged in events. She learned job skills and went to work, earning a small salary. The staff became her family and looked out for her best interest. They communicated with me and kept me abreast of Regina’s progress and issues. I will always be incredibly grateful for the excellent care they gave to her.
But the Sanctuary House had only day-programs, and Regina ultimately went to live in a group home. An unfortunate series of events followed. One group home closed without warning. At another, the staff took advantage of her. One took out a credit card in her name and ran it up into the thousands of dollars. The woman who ran this group home pulled Regina out of Sanctuary House and enrolled her in another program that provided very little. At the time, Regina told me she “liked” the new program — although in retrospect, she probably “liked” the fact that she wasn’t challenged. Regina’s condition steadily deteriorated after that. She was hospitalized a few weeks before she died, but even after she got out of the hospital, she didn’t seem quite right. She was edgy and irritable.
I woke up one morning in March 31, 2011 to multiple phone messages, including one from my father. As I listened to the panic in his voice — “Chris, call me back, it’s Regina…..I think she’s gone”— I hoped he meant she’d run away from the group home. But I could tell in his voice that “she’s gone” meant something much more dire. As I was about to call him back, a call came in from the group home. Regina was dead. She was found sprawled across her bed unresponsive. I raced to the group home. She was face down with her purse hooked on her arm. She had urinated on herself. I insisted on an autopsy and had to practically fight the coroner to agree. A 41-year-old dying suddenly and unexpectedly would warrant an inquiry as to why, especially when she had been the victim of fraud by a group home member who had been prosecuted for the crime. But this isn’t the case for the mentally ill. In the end, the coroner chalked it up to a seizure. Seizure as a consequence of medication to treat schizoaffective bipolar disorder.
She was my sister. I will be forever heartbroken by her story and how it ended.
But if telling her story can prevent one person from having to endure the pain my family went through, I’ll tell it. If telling makes the community aware of the woefully inadequate mental health services in our country, but also shines light on the selfless organizations like the Sanctuary House who fight for these who are neglected, then I will tell her story to anyone willing to listen.
Image via contributor