What Is EDS and How Can You Manage Its Symptoms
Editor's Note
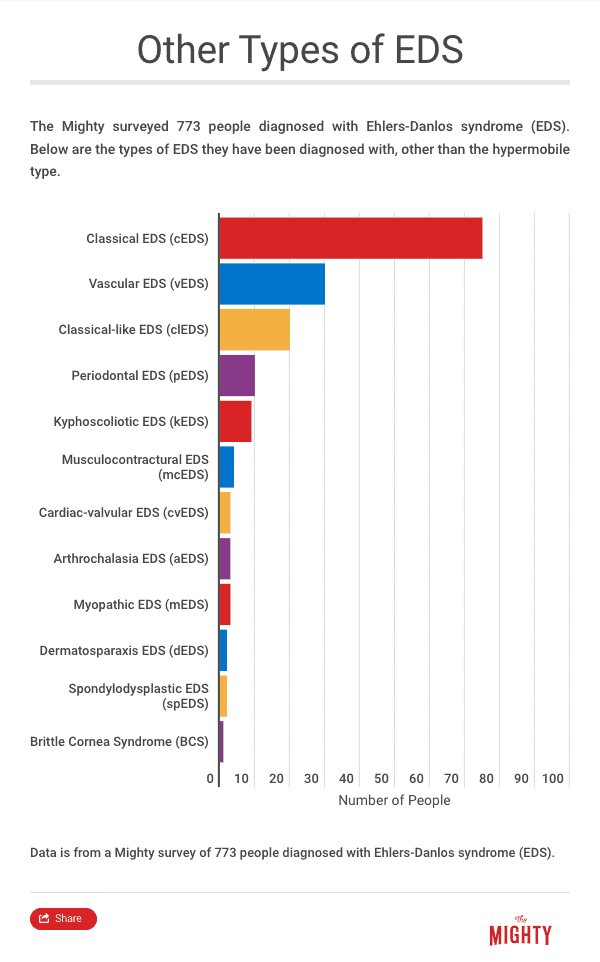
The Mighty’s Condition Guides combine the expertise of both the medical and patient community to help you and your loved ones on your health journeys. For the Ehlers-Danlos syndrome (EDS) guide, we interviewed three medical experts, read numerous studies and surveyed more than 750 people living with EDS. The guides are living documents and will be updated with new information as it becomes available.
What Is Ehlers-Danlos Syndrome?
Ehlers-Danlos syndrome (EDS) is a genetic condition that affects collagen, a connective tissue everywhere in your body, including your joints, ligaments, tendons, skin and organ tissues. The most common EDS symptoms include overly flexible joints, stretchy or loose skin and easy bruising. There are currently 13 subtypes of EDS. The most common is hypermobile Ehlers-Danlos syndrome (hEDS).
• What is Ehlers-Danlos Syndrome?
• What Are Common Ehlers-Danlos Syndrome Symptoms?
Learn More About Ehlers-Danlos Syndrome: Symptoms | Diagnosis | Treatment | Resources

Medically reviewed by David S. Saperstein, M.D.
What Are the Types of Ehlers-Danlos Syndrome? | Who Gets Ehlers-Danlos Syndrome? | What Causes Ehlers-Danlos Syndrome?
Your friends may think your overly flexible joints make a great party trick, but for you, they can be quite painful. This is especially true when your joints dislocate, which happens often, even when you try to pick up something “normal” like a shopping basket full of groceries. Sometimes joint dislocations happen so often that you need braces or splints to get through everyday activities.
Your skin may also be stretchy — you can easily pull it away from your body — and it’s fragile. You’re prone to bruising, and a lot of times, you don’t even know what caused the bruise. When you get a cut, it doesn’t heal very fast. You may also struggle with digestive system issues, chronic pain, fatigue and feeling dizzy or fainting.
These symptoms may indicate you have Ehlers-Danlos syndrome, which in addition to your joints and skin, can affect everything from your eyes to your internal organs like the heart, how much you grow and your teeth and gum health.
Ehlers-Danlos syndrome (EDS) is a genetic connective tissue disorder that affects the protein collagen in your body. Collagen is a key component of your connective tissue — the “glue” that holds everything from your joints to your organs in place. As you grapple with the abnormal experiences of dislocated joints, it’s expected that you search for any lead on what is EDS and how it will affect you personally.
There are 13 types of EDS, each with a specific set of symptoms that’s tied to a specific gene or group of genes causing problems with your connective tissue. EDS is most often passed through families, and you will have the same subtype of EDS as other members of your family, though your symptoms could be milder or more severe than your parents’, siblings’ or children’s.
To determine whether or not you have EDS and what subtype you have, your doctor will look at your symptoms, and then perform Ehlers-Danlos syndrome test on you. All of the subtypes of EDS except for hypermobile Ehlers-Danlos syndrome are tied to specific gene changes that doctors can identify. You may be referred to a geneticist or other EDS specialist to test your genes to confirm your EDS diagnosis.
Given the wide range of symptoms associated with Ehlers-Danlos Syndrome, it’s important to recognize that there isn’t a one-size-fits-all solution when it comes to managing this condition. Rather, the focus of Ehlers-Danlos syndrome treatment is typically on mitigating symptoms and taking care to complications. By understanding what is EDS and its specific effect on a person, it’s possible to create a tailored treatment to significantly improve the quality of life for those living with EDS.
There is no cure for any of the types of EDS, but treatments like joint exercises and pain management can provide symptom relief and prevent the condition from getting worse.

What Are the Types of Ehlers-Danlos Syndrome?
There are currently 13 types of Ehlers-Danlos syndrome (EDS) that experts recognize. All types of EDS are considered rare, though hypermobile EDS (hEDS) is the most common — it’s estimated 1 out of 5,000 people have hEDS. Doctors will determine your EDS subtype based on your symptoms and the genes affected if you’re sent for Ehlers-Danlos syndrome testing.
Hypermobile EDS (hEDS)
If you have EDS, there’s a good chance you have hypermobile Ehlers-Danlos syndrome (hEDS). Doctors estimate that 80 to 90 percent of people with EDS have hEDS. This equals approximately 1 out of every 3,000 people or 2.25 million people worldwide. It’s the most common inherited tissue disorder known.4 As its name suggests, the primary symptom of hEDS is joint hypermobility, or very flexible joints, which is measured using the Beighton scoring system. Even though it’s the most common type of EDS, scientists still aren’t sure which gene causes it. Doctors believe it may actually be caused by more than one gene, but additional research is needed.

Classical EDS (cEDS)
The first subtype of EDS to be identified in the 1960s, classical Ehlers-Danlos syndrome (cEDS) causes stretchy skin, overly flexible joints (hypermobility) and scars that look “dented.” When you have cEDS, a geneticist can tell by looking for a mutation or unexpected change in your type V collagen genes, COL5A1 and COL5A2. In rare cases, your collagen 1 gene COL1A1 can also cause EDS, which leads to more serious vascular or blood vessel complications. Though genetic testing can identify mutations in most people with cEDS, there are still a number of times when you may have all the symptoms, but no gene changes will be detected. The classical type of EDS is estimated to be the second-most common type, behind hEDS, with 1 in every 20-40,000 people having the condition.3
Vascular EDS (vEDS)
Vascular Ehlers-Danlos syndrome (vEDS) is one of the most serious types of EDS because it affects your blood vessels, which are vital for the health of your organs. Those with vEDS may rupture an artery at a young age, with colon rupturing a major symptom. When not treated right away, these ruptures can be fatal. The average life span with vEDS is about 51 years. This type is relatively rare. It’s thought to occur in about 1 out of every 200,000 people. A mutation in your COL3A1 gene, which is responsible for type III collagen, has been linked to vEDS. In rare cases, your COL1A1 collagen 1 gene can also be affected.
Classical-like EDS (clEDS)
Classical-like Ehlers-Danlos syndrome (clEDS) has many features in common with the classical type of EDS. If you have clEDS, your skin may be both stretchy and feel velvety, and you may have joints that are more flexible than most of your friends. You might also bruise more easily than others. To find out if you have clEDS, a geneticist will test your TNXB gene to look for differences that cause the condition.
Cardiac-valvular EDS (cvEDS)
The main symptoms of Cardiac-valvular Ehlers-Danlos syndrome (cvEDS) include flexible joints, stretchy skin that bruises easily, and progressive heart problems caused by connective tissue issues in your heart valves. This type happens when you don’t have proα2‐chain of type I collagen because of mutations in your COL1A2 genes. It’s estimated that less than one out of every 1 million people have cvEDS.6
Arthrochalasia EDS (aEDS)
If you’re experiencing frequent hip dislocations in addition to joint hypermobility and stretchy skin, your doctor may consider the subtype arthrochalasia Ehlers-Danlos syndrome (aEDS). A geneticist will confirm your aEDS diagnosis by looking for mutations in your COL1A1 and COL1A2 genes.
Dermatosparaxis EDS (dEDS)
Dermatosparaxis Ehlers-Danlos syndrome (dEDS) shares a prefix with dermatology for good reason as dEDS mostly affects your skin. Your skin may be fragile, you might get extra wrinkles on the palms of your hands and you can get bruises so severe they hemorrhage. In addition, you might not grow as tall as you would expect. This is all caused by a mutation in your ADAMTS2 gene, the gene behind the procollagen I N‐proteinase.
Kyphoscoliotic EDS (kEDS)
Depending on which of your genes are affected, Kyphoscoliotic Ehlers-Danlos syndrome (kEDS) might present a little differently. Almost everyone with kEDS experiences low muscle tone; joint dislocations, especially in your shoulders, hips and knees; and kyphoscoliosis, which causes your spine to curve in ways it’s not supposed to. If the gene PLOD1 causes your kEDS, you will also have fragile skin and a smaller-than-usual cornea in your eye. When a FKBP14 gene mutation is the cause of your kEDS, you may experience hearing and bladder issues as well as thick skin.
Brittle Cornea Syndrome (BCS)
Brittle cornea syndrome (BCS) is a subtype of EDS that mostly affects your cornea, the clear outer layer of your eyes. You may have a bluish hue in the white area around your eyes, and the shape of your cornea may change because it’s thinner than it should be. BCS has been linked to several different genes, including ZNF469, PRDM5 or a zinc finger protein that scientists don’t know much about.
Spondylodysplastic EDS (spEDS)
There are three genes linked to spondylodysplastic Ehlers-Danlos syndrome (spEDS): B4GALT7, B3GALT6 or SLC39A13. Each of these genes changes cause you to have slightly different symptoms. The main markers of spEDS are low muscle tone, bowed limbs and not growing as tall as expected.
Musculocontractural EDS (mcEDS)
Because connective tissue determines the structure of almost all parts of your body, depending on the collagen genes that your EDS impacts, you might not have joint flexibility but rigid or overly inflexible joints, muscles or tendons. This is the case with musculocontractural Ehlers-Danlos syndrome (mcEDS), even though it’s opposite of the hyperflexibility in most other EDS subtypes. If you do have mcEDS, also look for stretchy skin, extra wrinkles and easy bruising and scarring. To confirm a diagnosis, your geneticist will look for mutations in several of your genes, including CHST14, D4ST1 and DSE.
Myopathic EDS (mEDS)
Myopathic Ehlers-Danlos syndrome (mEDS) causes you to have a mix of rigid and overly flexible joints. Typically your knees, hips and elbows will be rigid and stiff, while joints in your hands and feet are more flexible than usual. A geneticist will confirm if you have mEDS by searching for a mutation in your COL12A1 gene that determines your type XII collagen.
Periodontal EDS (pEDS)
Periodontal Ehlers-Danlos syndrome (pEDS) primarily causes dental and gum problems in addition to joint flexibility and fragile skin. If you have pEDS, your C1R or C1S genes may be mutated, which can be confirmed by genetic testing.

Who Gets Ehlers-Danlos Syndrome?
Across the 13 subtypes of EDS, it’s hard to estimate exactly how many people have the condition. EDS types like hEDS are common, while other forms, like cvEDS are very rare. On average, most experts estimate 1 of every 5,000 people has one type of EDS or another.3 Scientists and doctors also believe the rates of recorded EDS cases might be low because you may have such a mild case of EDS that you never need to go to the doctor for it. EDS has been recorded in all genders of all ethnic backgrounds.1 There are more recorded cases of female-born EDS patients than male-born EDS patients.
Because EDS is a genetic disorder, children are born with the gene mutations that cause the syndrome. Early in life, kids may show off their double-jointed limbs to friends or get a slow-healing fracture at a sports game that causes suspicion. However, many children naturally outgrow hypermobile joints by the time they turn 5 years old. For this reason, some doctors recommend waiting to evaluate young people for EDS until they are at least 5 or 6 years old, though many patients are much older by the time they get the correct diagnosis.5
Given the varying prevalence and manifestations that define what is EDS, it can often be challenging to pinpoint a diagnosis. If there’s a signs that child or adult exhibits some of the following traits on this EDS symptoms checklist, then you may want to ask for genetic screening:
- Hypermobile joints: Joints that move beyond the normal range expected for a particular joint, including joints that dislocate easily.
- Skin involvement: This could include unusually stretchy skin, thin or translucent skin, easy bruising, slow wound healing, or atrophic scarring (thin or depressed scars).
- Chronic pain: This could be joint pain, muscle pain, or even nerve pain.
- Cardiovascular issues: Some types of EDS can involve the heart and blood vessels, so symptoms like palpitations, chest pain, or fainting could be relevant.
- Digestive problems: This could include symptoms like abdominal pain, nausea, bloating, constipation, or diarrhea.
- Dental issues: These can include fragile teeth, gum disease, and a high palate.
Remember, this checklist serves as a guide to answering the question, “What is EDS?” based on common symptoms. However, having these symptoms doesn’t definitively mean you have EDS. It’s always essential to discuss these symptoms with healthcare professionals who can help you manage the process of diagnosis and treatment.


What Causes Ehlers-Danlos Syndrome?
EDS is a genetic condition, not an autoimmune disease, as some people think. EDS, in particular, affects your collagen genes. Collagen is a protein that gives your body structure, forming connective tissue and keeping everything in your body in place. When you look at the collagen of an EDS patient under a microscope, you might see fewer cells than you would for a patient without EDS. These collagen levels are controlled by your genes and whether or not they have mutated or changed.
There are two ways you might get EDS and the collagen-related symptoms that come with it. The first is inheriting the condition from your family. If one of your parents has the changed gene for EDS, they passed it to you. The other way you can get EDS, even if nobody in your family has it, is when your genes are copied wrong when you are conceived. This is called a de novo or “new” case of EDS.
Genetics 101
Your DNA is basically your biological blueprint. In your DNA, you have a collection of genes that each determine who you will be. What eye and hair color will you have? How tall will you be? What illnesses or syndromes will you be at risk for? You have two copies of the same gene, one inherited from your biological mother and another inherited from your biological father. Depending on the data contained in those genetic “files,” your genes will “express” themselves per the rules or patterns of genetics.
There are two types of genes — dominant and recessive — that, when combined, determine what characteristics you will inherit. You could have two dominant or two recessive genes or a combination of one dominant and one recessive gene. Each combination encodes a different trait into your DNA. When you get a dominant and recessive gene, think of the dominant gene as the “louder” one. It’s the gene you can’t ignore, and the information in the dominant gene is the one that “wins” and gets expressed. Only when you get two recessive genes together do those recessive characteristics have a chance of making it out into the world.
Inheriting EDS
Whether or not you have EDS and what subtype you have is similarly determined by your dominant and recessive genes, specifically the genes that regulate your body’s collagen or connective tissue. Some subtypes of EDS are transferred by a dominant gene, which means if your parents, siblings or children have the condition, you have a 50 percent chance of inheriting the same gene variant.1
Other types of EDS are considered recessive, which means you only have a 25 percent chance of inheriting EDS. But for you to have EDS, you would need two copies of the changed collagen gene instead of just one copy, as is the case in a dominant inheritance pattern. You also have a 50-percent chance of inheriting one recessive EDS-causing gene from one parent but not the other. This means you may never have EDS, but you are a carrier of the recessive gene that causes it, which can be passed on to your children later.
Subtypes also usually run in families. So if your mother has the hypermobile form of EDS, that’s the same subtype you would get as well. However, you may have severe EDS symptoms and another family member may have such mild symptoms they never have to go to the doctor.

De Novo EDS
Even if no one in your family has ever had EDS, you can still get the condition. When you get a “new” case of EDS, meaning it wasn’t inherited from your family, it’s called “de novo” or “new.” This happens when your genes aren’t copied correctly during conception. As your genetic material is copied from your parents’ genes, a mistake could be made that happens to be the exact same mutation that causes a type of EDS. Some experts believe as many as 50 percent of EDS cases could be new and not inherited from a family member.2
Learn More About Ehlers-Danlos Syndrome: Symptoms | Diagnosis | Treatment | Resources


Sources
- Atwal, P. (2018). Ehlers-Danlos Syndrome [Telephone interview].
- Bowen, J. M., Sobey, G. J., Burrows, N. P., Colombi, M., Lavallee, M. E., Malfait, F., & Francomano, C. A. (2017). Ehlers–Danlos Syndrome, Classical Type. American Journal of Medical Genetics Part C (Seminars in Medical Genetics), 175C, 27-39. Retrieved from https://www.ehlers-danlos.com/pdf/2017-FINAL-AJMG-PDFs/Bowen_et_al-2017-American_Journal_of_Medical_Genetics_Part_C-_Seminars_in_Medical_Genetics.pdf
- Genetics Home Reference. (2017). Ehlers-Danlos syndrome. Retrieved from https://ghr.nlm.nih.gov/condition/ehlers-danlos-syndrome#statistics
- Levy, H. P. (2018, June 21). Hypermobile Ehlers-Danlos Syndrome. Retrieved from https://www.ncbi.nlm.nih.gov/books/NBK1279/
- Neilson, D. (2013, August 19). Ehlers-Danlos Syndrome: The lengthy road to diagnosis. Retrieved from https://blog.cincinnatichildrens.org/rare-and-complex-conditions/ehlers-danlos-syndrome-the-lengthy-road-to-diagnosis/
- Orphanet. (n.d.). Cardiac valvular Ehlers Danlos syndrome. Retrieved from https://www.orpha.net/consor/cgi-bin/OC_Exp.php?lng=en&Expert=230851

