Some types of rare disease impact only one part of your body. Charcot-Marie-Tooth disease, for example, specifically impacts nerves that send messages and cells to certain muscles in your body. Other illnesses, however, can impact systems throughout your entire body. For people with systemic illnesses, it is common to feel sick or in pain most of the time. Vasculitis is one of these health conditions.
Vasculitis is a family of rare diseases that are characterized by the inflammation of blood vessels that can damage the vessels. There are around 20 different forms of vasculitis and they are autoimmune diseases. Symptoms can range from acute rashes in some people to organ failure in others.
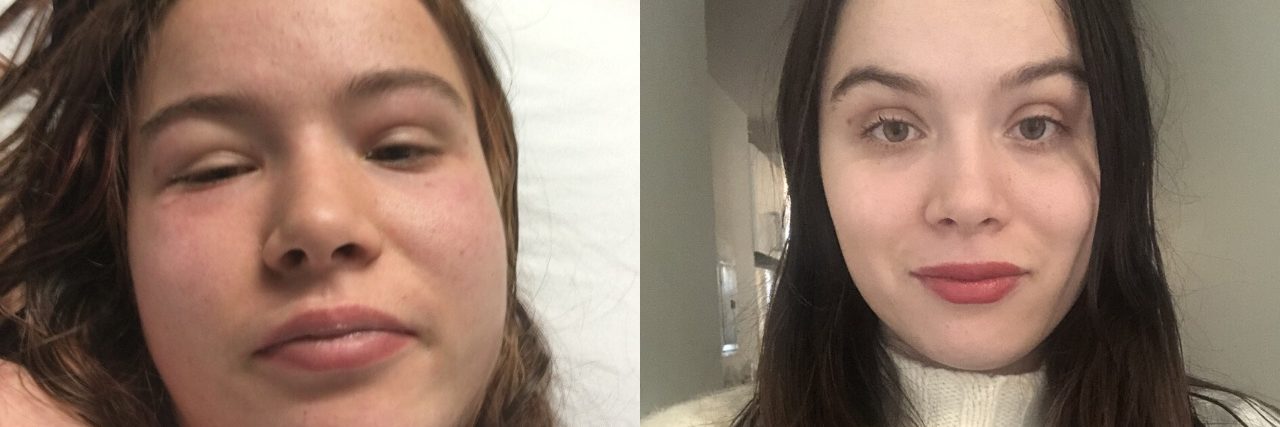
Trauma and infections are some of the many triggers that may cause vasculitis to become active or worsen in people who have a form of this rare disease. My systemic urticarial vasculitis became active after I was in a car accident when I was 18. I had a range of symptoms, from severe facial inflammation to stomach pains, until I was diagnosed with a blood test and a biopsy.
Most forms of vasculitis are rare, with the cause of the disease being unknown. However, there are some types of vasculitis, like Kawasaki disease, that may run in families. The prognosis of people with vasculitis often depends on the type you have and if it is caught early.
Here are five things you should know about vasculitis.
1. Some forms of vasculitis are more prevalent in certain age or ethnic groups.
Vasculitis affects male and female patients equally, although there are exceptions depending on the type of vasculitis. Different age groups, ethnicities, sex, medical and family histories can increase people’s chances of getting this condition, according to the National Heart, Lung, and Blood Institute. For example:
- Buerger’s disease usually affects men younger than 45
- Giant cell arteritis affects adults 50 years and older, women two to four times more often than men and is most common in Scandinavia and people living in Minnesota
- Kawasaki disease affects only children and is more common among children of Japanese descent
- Behçet’s disease is most common in people of Turkish descent and affects more men than women
Vasculitis can also be drug-induced. Some of the medications that may increase someone’s chance of having vasculitis include:
- Hydralazine
- Levamisole
- Propylthiouracil
- Tumor necrosis factor inhibitors
The prevalence of vasculitis varies immensely depending on the form of the disease and a person’s location. For example, the Vasculitis Foundation reports that an estimated 3 to 5 per 100,000 people have Behçet’s disease in the United States, but 400 per 100,000 people have Behçet’s disease in Turkey. There are no estimates on how many people the disease affects for some types of vasculitis, such as the type I have, systemic urticarial vasculitis.
2. Symptoms of vasculitis vary depending on which organs are affected.
Vasculitis is a systemic illness, which means that you can experience symptoms anywhere in your body. Common symptoms of vasculitis include fever, headache, fatigue, general pain, rashes, and nerve problems that may present themselves as numbness or weakness, according to the Mayo Clinic.
The symptoms that people with vasculitis may experience depends on which type they have and which organs vasculitis impacts. There are around 20 types of vasculitis, and they are often separated into subgroups based on which size vessels the disease affects, including:
- Large vessel vasculitis includes giant cell arteritis and Takayasu’s arteritis.
- Medium vessel vasculitis includes Kawasaki disease and polyarteritis nodosa.
- Small and medium vessel vasculitis includes granulomatosis with polyangiitis, eosinophilic granulomatosis with polyangiitis and central nervous system angiitis.
- Small vessel vasculitis includes urticarial vasculitis, Henoch-Schönlein purpura and cutaneous small-vessel vasculitis.
- Vasculitis that affects a range of vessels includes Behcet’s syndrome and Cogan’s syndrome.
Vasculitis can also cause organ damage or failure when your symptoms are not managed. The National Heart, Lung, and Blood Institute also states that complications from this disease not being diagnosed and treated could include blindness, deafness, heart attacks and strokes.
3. Biopsies are often used to confirm a diagnosis when possible.
Many different diagnostic tests are often done to confirm a diagnosis of vasculitis based on a person’s symptoms and medical history, according to the National Organization for Rare Disorders. These tests could include bloodwork, an X-ray of your blood vessels or a biopsy of an organ when it is safe to do so.
I was diagnosed with urticarial vasculitis after a blood test showed that my erythrocyte sedimentation rate and my C-Reactive protein levels were out of the normal range, and a skin biopsy confirmed that I had inflammation in my skin. Doctors also did a urine analysis to check for signs of kidney failure, which was negative.
4. Vasculitis can either be a short-term or lifelong condition.
Vasculitis can be either an acute or chronic condition. If caught early on, vasculitis can be treatable and lead to remission from the disease. Johns Hopkins Vasculitis Center reported some types of vasculitis, like Henoch-Schönlein purpura or vasculitis caused by medication, can be cured.
The American College of Rheumatology noteed that glucocorticoids medications such as prednisone are an important part of treating most forms of vasculitis. Newer drugs like rituximab have also been shown to help treat severe forms of vasculitis. Patients may need organ transplants or dialysis if their vasculitis caused organ failure as well as other treatments to mitigate their symptoms.
As many people with vasculitis also experience chronic pain, they sometimes take over-the-counter pain relief medication or could be prescribed medication to help manage pain by their doctors.
5. Advocates fought to change the name of a type of vasculitis.
From the 1950s to 2011, granulomatosis with polyangiitis used to be known as Wegener’s granulomatosis. According to the Vasculitis Foundation, Wegener’s granulomatosis was named after Dr. Friedrich Wegener, an early describer of the disease. While others have advocated for a condition name change for a variety of reasons (such as changing stiff-man to stuff-person syndrome), it was Wegener’s harmful past that prompted advocates to change Wegener’s granulomatosis.
Now-retired Mayo Clinic doctor Dr. Eric Matteson was a prominent advocate in leading the name change after he discovered that Dr. Wegener was a Nazi Party member. The American College of Rheumatology, the American Society of Nephrology and the European League Against Rheumatism adopted the name change togranulomatosis with polyangiitis in 2011. Many descriptions of this form of vasculitis include that it was formerly known as Wegner’s.
References (click to expand)
- American College of Rheumatology (2017, March). Vasculitis. Retrieved https://www.rheumatology.org/I-Am-A/Patient-Caregiver/Diseases-Conditions/Vasculitis
- Johns Hopkins Vasculitis Center (n.d.). Vasculitis Frequently Asked Questions. Retrieved https://www.hopkinsvasculitis.org/resources/vasculitis-faq/
- Mayo Clinic (2017, Oct. 16). Vasculitis. Retrieved https://www.mayoclinic.org/diseases-conditions/vasculitis/symptoms-causes/syc-20363435
- MPR News (2011, May 18). Mayo doctor helped spearhead name change for disorder with Nazi namesake. Retrieved https://www.mprnews.org/story/2011/05/18/nazi-named-disorder-name-change
- National Heart, Lung, and Blood Institute (2019, Oct. 21). Vasculitis. Retrieved https://www.nhlbi.nih.gov/health-topics/vasculitis
- National Organization for Rare Disorders (2008). Vasculitis. Retrieved https://rarediseases.org/rare-diseases/vasculitis/
- Vasculitis Foundation (n.d.) Behcet’s Syndrome. Retrieved https://www.vasculitisfoundation.org/education/behcets-disease/#1545059297615-6dd5af3e-896d
- Vasculitis Foundation (n.d.) General Vasculitis. Retrieved https://www.vasculitisfoundation.org/vasculitis/#1545129976387-fd136823-13d7
- Vasculitis Foundation (2011, May 5). New Name for Wegener’s Granulomatosis Retrieved https://www.vasculitisfoundation.org/mcm_article/new-name-for-wegeners-granulomatosis/
Image via author/Canva