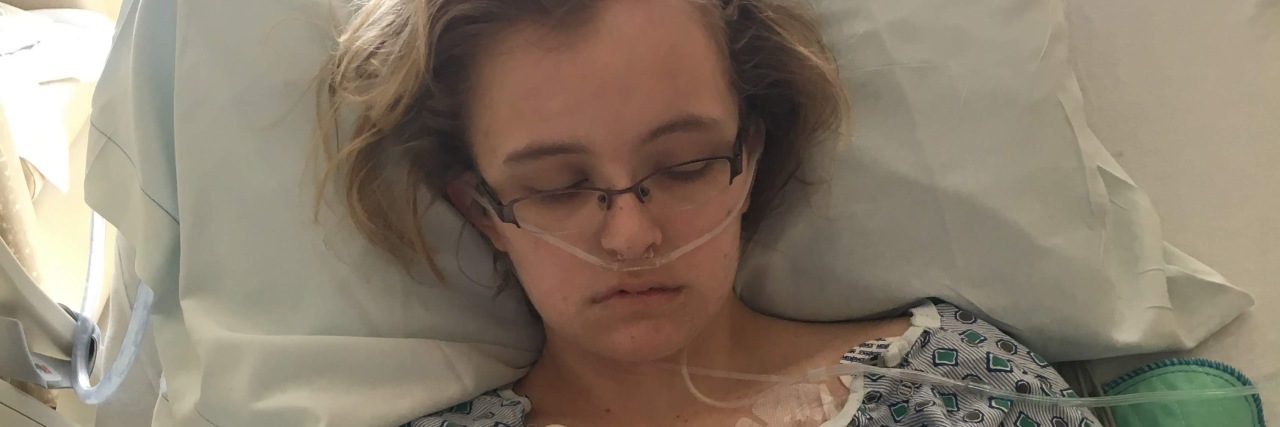
The Hardest Part of Coping With Pediatric-Onset Stiff Person Syndrome
There is nothing glamorous about a life with stiff person syndrome (SPS) in general, but I have noticed over the years that support is severely lacking for teens and young adults with the condition in support groups. Some have been so traumatized by the loss of quality of life, pain, and disease before diagnosis, they refuse to even talk to other young warriors. Others have resigned themselves to believing they are dying soon, and some are still in that seven-plus-year diagnostic limbo awaiting a diagnosis and/or effective treatment.
I can go on Facebook to a support group and find an adult with stiff person syndrome that started after they had a career, a family, their education, and so forth. It would be fair to say that life had “started” for them versus younger people like then-16 year old me. I know I am one of the fortunate ones. I finished high school and graduated college; even though it took five years of hospitalizations, plasma exchange therapy, IVIG/SCIG, a surgical GJ feeding tube, being connected to my backpack 22 hours a day, and taking classes three semesters a year. Kids and adults certainly face different challenges and I wouldn’t argue which is “easier,” but it is easier for me to relate to a younger population.
I think one of the hardest parts of raising awareness or talking about the younger version of SPS is that the pediatric-onset pictures and videos, in general, tend to be very “graphic” or “traumatizing” to others; especially those without the disease. I feel like some of the urgency to raise money for SPS research is because these videos are “graphic” and in my case, have made doctors in the corner of my ICU room cry because they didn’t have any power to stop one of my attacks. There was not an ounce of the medication I needed in that major city hospital’s ICU.
I want so badly to be able to have these conversations with other younger, 20-something warriors. I know a few, but not many, and most don’t care to discuss the subject. They seem to internalize it better than I do and I know that internalizing stressful situations often leads to PTSD over time. While there is no doubt I have mild situational PTSD from all of this, I’ve learned from a young age to talk about life: the good and the bad, challenges, and of course, the victories along the way.
Because I have medical personnel as parents, even now, almost a decade later, they will tell me to my face they don’t believe me or they don’t know what to believe. I meet every diagnostic criteria for the disease in terms of blood tests, cerebrospinal fluid (CSF) tests, electromyography (EMG), and more. All of this because I was tired of being the “sick girl” and just wanted my life to be “normal,” so I told them I was 100% fine and not sick at all. But that couldn’t be further from the truth. I was in a coma for 10 days due to a seizure that lasted over 24 hours. I’d had multiple seizures before then causing me to turn blue. My body still spasmed while unconscious on the ventilator. And my feet and knees are chronically stuck in contractures. So as much as I don’t want to be the “sick one,” especially after nearly a decade, I am. With no good treatment and no cure, living with this diagnosis and its comorbidities is extremely isolating as a young person.