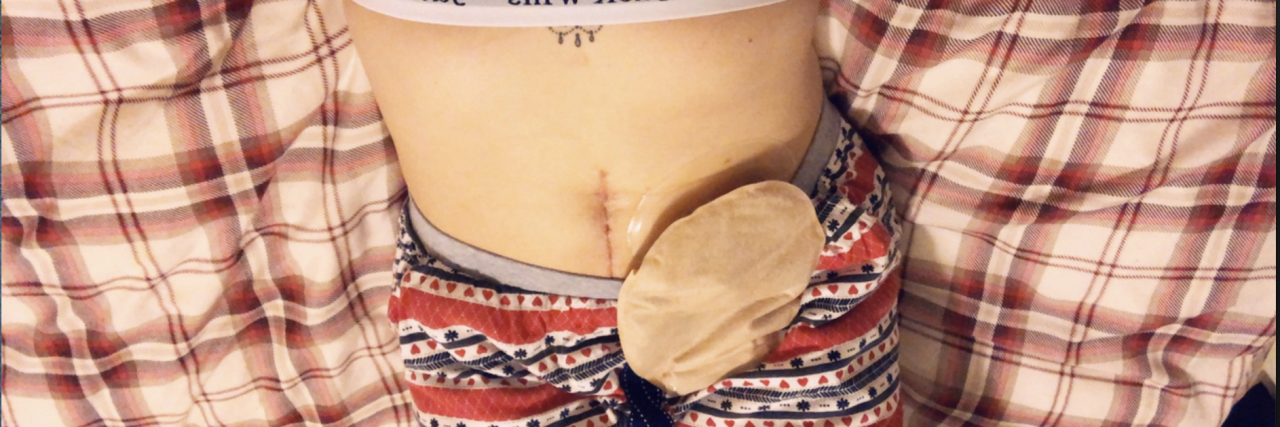
Having an ileostomy (where they bring your small bowel out onto the skin surface to form a stoma) was something I was always acutely aware might be in my future once I found out I had Crohn’s disease, but I was vehemently against having one at all costs. I wish I’d realized then that although there are some issues that can be associated with having a stoma, for me, just being free of pain was reason enough to have one years ago!
If stoma surgery is in the cards for you, there’s a lot of stuff that you might not be told beforehand, and stuff you might not even think to ask about! As a list type girl, here are 15 things I wish I knew before having my surgery:
1) It’s likely you’ll have an initial meeting with a stoma nurse / healthcare professional who’ll mark you up for the stoma — this is more important than you realize. Really think about what you wear and where you like your clothes to sit while they’re doing this – you’ll thank me for that later! Make a list of all of the questions you can think of beforehand (e.g. what to expect within the first few days and further down the line, what the stoma will look like, what changing the bag involves, how your life might change etc.) and check that list before you leave. You probably won’t see them again until after your operation, when things can be a little overwhelming.
2) When you wake up from surgery, you’ll more than likely have been fitted with a clear stoma bag – do not freak out if you take a look and see blood in the bag. It is perfectly normal! Your stoma is likely to just bleed a bit for the first 24 hours and not produce much of anything else.
3) It’s different for everyone, but I personally recommend trying to look at your stoma and be involved in changing the bag as early as you feel you can. Seeing it makes it more real and once you begin to look after it yourself, you will start to feel differently about it. I looked at lots of photos of other people’s stomas online before my surgery; preparing yourself for what it’s going to look like can really help.
4) Having a piece of chewing gum can help to get your stoma started. Be prepared for the little air bubbles you’ll initially feel when it starts to wake up. When mine became active it was mostly air and liquid coming out — I felt a slight pressure and then a bit of bubbling. It wasn’t painful at all though, which is one of the things I was worried about.
5) Your output (the term used for what comes out of your stoma) is likely to be very watery to begin with. You’ll quickly learn that what you eat will make a huge difference to the amount of output you have and the consistency. I can’t recommend enough packing some marshmallows or jelly babies for while you’re in hospital – as an ostomate, they will soon become your best friend. Once you begin to introduce solid food back in, your output will calm down and thicken, so don’t panic. The nurses are also there to help you so don’t worry about it bursting overnight. I had a little meltdown once my stoma became active, afraid I wouldn’t be able to keep getting up during the night to empty it. The nurses just told me they would come and empty it for me – I wasn’t even aware they were doing it most of the night!
6) The smell. I’m not going to lie — it can smell really bad to begin with. Having had Crohn’s for over nine years, I thought I could handle bad smells, but wow! The first three days were just awful and I gagged every single time I had to empty the bag. Believe me, that won’t last! Just as what you eat affects the consistency of the output, you’ll find it will affect the smell too, but it won’t be as bad as it is those first few days, I promise!
7) You can’t feel the stoma. For the first few days I could feel a pressure before my stoma was active, but this subsided once the surgery swelling started to go down.
8) There are many different types of bags. Your stoma nurse / healthcare professional should provide you with two or three types to try at the beginning, but if you’re not absolutely happy with the options given, just keep asking for others to try! There are lots of brands, but also lots of sizes, material types etc. I think I might be on my 10th type now as my skin reacts to quite a lot of the material. Don’t feel you have to rush to settle on one type. This bag is about to become your closest accessory, so take your time to pick one you’re happy with. The same goes for the other stoma supplies (powder, remover sprays, barrier wipes etc.) – ask for samples and try lots!
9) This next one is a tough one to deal with – it is highly likely that at some point you will experience a bag leak. These can happen for lots of different reasons – poorly-fitting bag, adhesive becoming unstuck, pancaking (where the output gathers all at the top, pulling the bag away from the skin), ballooning (where the bag fills with too much air), movement affecting the adhesiveness of the bag etc. Sometimes it can seem to happen for no reason at all. The most important thing is to not panic! At the time, and especially the first time it happens, it can feel like the worst thing in the world, but you will deal with it and you will be OK!
There are ways you can go about trying to help stop leaks from happening. For example, I’d recommend setting at least one alarm during the night to wake you up so you can empty your bag – even if it’s just releasing the air. I usually set an alarm for around 3 a.m. Make sure your bag is stuck on properly when changing it – heat can help with sealing it down and I usually give it a blast from the hairdryer for a few seconds as I’m pushing it down. If you’re experiencing pancaking, try putting some oil at the top of the bag to help encourage the output to move down. Make sure you only have a very tiny gap between the edge of the hole you’ve cut in your bag and your stoma – if output starts to seep under the bag this can not only cause leaks, but also damage the surrounding skin. I found this one out the hard way!
Try to be prepared. If you can, always carry around a spare set of supplies with you. I have a small bag in my handbag that contains a pre-cut stoma bag, some dry wipes, a small bag for rubbish, some flange extenders, powder and adhesive remover spray. I also take a spare pair of clothes to work with me. This is mainly because I’ve had a large amount of leaks from using bags that wouldn’t stick well to my skin, so I feel more comfortable if I’m prepared, but do whatever works for you.
10) Your stoma nurse / healthcare professional will become your best friend to begin with, and should be your first port of call for any of your queries or concerns. Honestly, no question will be a silly one and no worry is too small not to flag up. They are there to help you, and I wholeheartedly recommend making the most of them! I’ve had quite a lot of skin problems with my stoma and have at times lost my confidence with it all. This can happen. You’ve just had a major life change and it can affect you mentally as well as physically. But speaking to your stoma nurse / healthcare professional about all of it – the physical and the mental issues you might be having — is the best thing you can do!
If you don’t feel you can talk to your stoma nurse, then definitely find someone you feel comfortable with to talk to about it. I’ve had some pretty embarrassing moments with mine and sometimes I choose to cry about it over a cup of tea with my mum and sometimes I just want to laugh it off with close friends. There are also lots of support groups you can join where fellow ostomates are always on hand with positivity and kindness!
11) Support wear can really help, not only in the first few days but also further down the line. There are lots of different types to choose from and doing a bit of research before picking what you’d like can be invaluable and save you a bit of money! There are types of support underwear with extra pouches to hold your bag, mild support bands for daily use, support bands for sport, support wraps, hernia protection bands, support vests… the list seems endless. Think about what activities you do, what you do for work, what clothes you wear and use all of that to help you decide what will work best for you. In the U.K., some of the support wear is available on prescription, and it is worthwhile having a good relationship with both your GP and stoma nurse as this can make the process of getting your stoma supplies much easier!
12) Naming your stoma can really help! I laughed at this idea initially, but have found that giving my stoma an affectionate name made me feel a bit better about it. Mine is called Paloma. You can even accessorize it with stoma bag covers; I’m particularly fond of my alpaca brush cotton cover.
13) You will need to rest! It’s hard when you’re starting to feel better to make yourself rest, but it is so important. Especially in the first few months. You’ve just had major surgery, which is bad enough in itself, but if you overdo it too quickly you do run the risk of getting a hernia. Give yourself time to heal properly. Try not to compare your recovery to other people’s either — some people may feel that they can go back to their normal lives after four to six weeks and some will need months. Both recovery periods are OK!
14) Stay hydrated! It can be quite easy to become dehydrated with a stoma. Lots of sports drinks, rehydration drinks and regular water can really help. I also found upping my protein and salt intake made the healing process speed up and made me feel much better.
15) Finally, I want to tell you it will be OK. It is scary, it takes some adjusting, your routine might change and at times you’ll wonder why you ever thought this would be a good idea. But it will get better, you’ll get quicker at bag changes, learn when your stoma is more active and when you can leave emptying the bag a bit longer. Eventually, in my experience you will start to feel in control again. Just give yourself time and don’t be too hard on yourself. Remember what you’ve already overcome and what now lies ahead. We are all stronger than we realize and braver than we think.