Dear Doctor, Here's What I Wish You Would Ask Us at Appointments
Dear Doctor,
I’m so thankful for the educated care you have provided us in caring for our daughter with food protein-induced
What I really wish you would ask us amongst the functional aspects of her physical care, is what the toll has been on our family unit. This letter is to tell you all the things that you never ask us, but my heart wishes you would. I know you are somewhat aware, but the reality of caring for a chronically ill child is not always easy.
Through your question-asking, you would discover that our marriage has struggled. It’s not just because of the stresses of work, money, and ordinary, everyday life that everyone faces. We have to juggle evenings of holding our daughter as she heaves because of FPIES — all the while doing the mountain of laundry, mopping and sponging that needs to be done when she has a flare. One of us has to pause the cleaning to order food for dinner so that we could hold her and still serve some food to our other tired and fragile children. It costs money, and takes a toll on our health. We also need have the added complexity of looking for signs that she’s going into shock. As her eyes roll back into her head, it’s a precarious balance. I don’t want unnecessary intervention and hospital trips, but I know that if I don’t get it right, she will be so very ill.
Despite all our careful communication, it’s not uncommon that an allergen might be fed at daycare. This is not only frustrating, it comes with lost work time and money, since one of us has to take off work while she recovers. Our personal and annual leave really doesn’t stretch far enough. Financially, our margins have diminished. There’s no real measure of the costs of the speech therapists, dieticians, psychologists, special foods, medicines, and linens. We can’t call on the help of a charitable body that supports people with her disease, because there isn’t one.
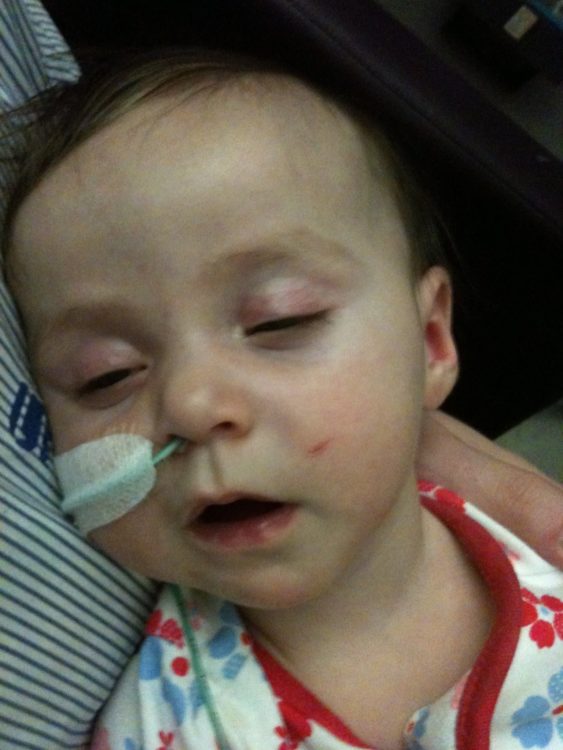
As you progress further with your question asking, you would discover that we have to support our eldest child as well. She now has panic attacks and visibly starts shaking when she hears the word “vomit.” She is exceptionally perceptive and has watched her youngest sister turn grey, floppy and wretch bile. The first time her sister had an acute reaction, I chose not to call an ambulance because not only did I not really understand what was happening, I also didn’t know what to do with my other little ones. As I drove to the hospital, I played happy music to mask my fear, occasionally asking my eldest to see if her sister was “sleeping” and wouldn’t open her eyes, or whether she was just resting and liked having her head patted. The bigger girls have come to the hospital with me because our youngest falls limp in my arms and requires urgent attention. I don’t want them to have to come with us, but they do when it’s urgent and there’s no rapid care solution available.
I’d love you to know that time together as a family has remained our greatest priority. We believe that laughter brings healing and “stickability.” Our own needs for social interactions have been forced to become a lesser priority. The most faithful of friends have stuck by us as our communication has waxed and waned. The faithful have ceaselessly asked about our daughter’s well-being and the condition of our hearts and souls. The comforting words sent in a message when I’ve cried out for help have carried me on many occasions. They hear what I can’t articulate.
Time seems to move remarkably slowly during the nights. Sitting upright in a chair in the middle of the night while you hold your child who’s screaming out of discomfort gives you too much time to think and feel. You wade through the feelings of isolation. Your mind wanders. No parent of a sick child wants to publicly confess this, but during those middle-of-the-night moments, your mind asks horrifying questions. Thankfully, these thoughts are fleeting and disappear as I gaze upon her beautiful face, despite her contortions from pain. If I could take on her disease for her, I would — without a second thought.
If you wanted to know what is most exhausting, it would be the preparation of her food. It takes me an inordinate amount of time in planning and cooking foods that are as similar to foods her sisters or other children will be eating. If we go out, I have to cook ahead of time and ensure we have enough food with us. It’s more than likely that she will reject the food that has been prepared, but it needs to be done anyway. You know well that her growth is rather stunted. To keep any vague level of growth, I have to calorie load her food. I add butter and sugar to pretty much everything.
I believe it’s important for you to think about the structure of your consultations. When we meet, our daughter is incredibly aware of what we discuss. Before we go to the appointment, I ask her if there is anything she wants to ask you or tell you about her body. She usually has something. I would find it helpful if you addressed her at times throughout the appointment. She is her own person with thoughts and feelings. You can ask her questions. I believe that this is vitally important as she needs to have some ownership of her body, since she has very little control over what has happened to it.
I know that what I’m asking of you is unrealistic. You carry a rather insurmountable patient load. Deep down, I think your time is best spent on research and consultation rather than asking families questions about their psychosocial support needs. I would, however, ask that you lobby your hospitals for holistic care for families with rare disease. I’d ask you to fight for our government to provide better funding for our pediatric hospitals, especially for funding to provide multidisciplinary care for children who have diseases that fall outside the better supported pediatric illnesses.
My voice matters. Your voice matters. Maybe we can raise them together to declare, “This may be rare, but this is real.”
From a Rare Mama Who Cares