A Sleepover At The ER: Navigating a Rare Blood Condition
“Is it possible that it is just… nothing?”
Raising my voice over the beeps of the Alaris medical pump, clutching a folded medical gown with tigers on it, and staring at seven doctors with their traveling computers should have been my sign that this was not “nothing.”
“No. This is definitely something,” the doctor states. He turns to the panel of residents filling the hallway. “We have here a seven-year-old presenting with head hematomas that needs attention. How do you handle sending in a patient who needs surgical intervention when you aren’t sure if their blood can clot?” He pauses for their response. “It’s tricky, isn’t it?”
He turns his attention back towards us. “This is a teaching hospital. Yours is a good case to learn on.”
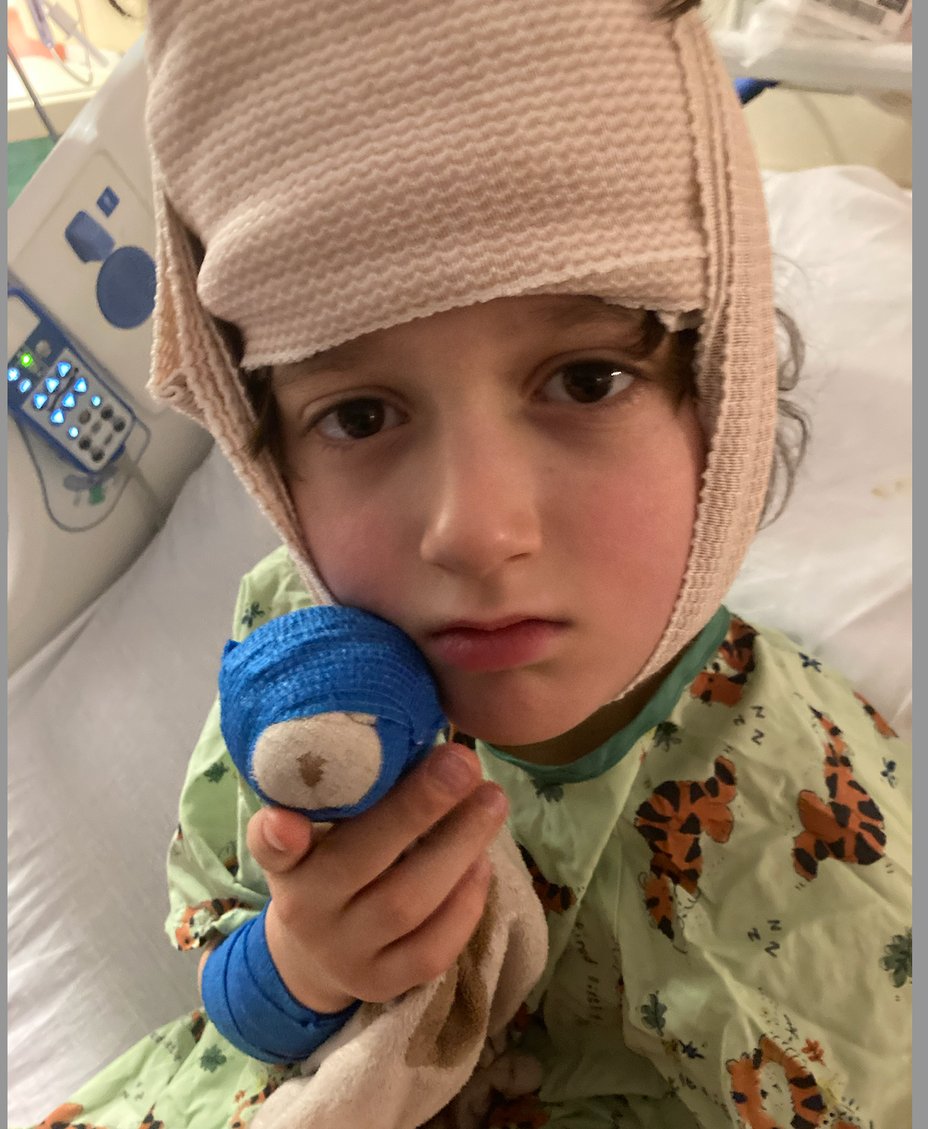
Twelve days ago, I tucked my son into bed surrounded by his five favorite stuffed animals, his Bobos. He casually mentioned, “Momma, I bunked my head on the monkey bars during recess but I’m okay.” It wasn’t significant enough of an event to warrant telling the recess monitors, visiting the nurse, or even using an ice pack. I kissed his forehead and snuggled him in tightly into bed, carefully laying each Bobo around his neck, as he likes. Just days later, it would become the same routine I would continue at the children’s hospital for the next ten days.
Quietly, this unremarkable bump began a stealthy descent into concerning bumps on both sides of our child’s forehead and the top of his skull.
These hematomas, or as Oliver called them, the mushy part of his head that felt now like Squishmellows, grew to an alarming size. So alarming that the pediatrician's office immediately sent us to the emergency room, which lead us to our new room on the Hematology/Oncology floor.
“It appears as if we are looking at something rare,” the doctor continues explaining to the team. He describes how Oliver’s initial diagnosis of ITP at age two appears inaccurate or perhaps incomplete. This diagnosis occurred after a terrifying investigation when he presented with a petechiae rash. It was determined that Oliver’s body produced fewer platelets and would require supervision as he grew older. It was no big deal. An occasional nosebleed here, a visit to get blood drawn there; the diagnosis while unsettling was in no way impeding the life of a healthy, active seven-year-old. However, this time, it seemed like the monkey bars unearthed something more nefarious hiding in his system. The doctor translated: It is like the platelets are the pieces that build up at the dam to prevent the water from flowing. We initially thought he just didn’t have enough pieces, but now it appears that the ones he has aren’t really working. Like they are on strike…
“So, what do we do?” my husband asks while I attempt to draw a picture of water flowing into a dam in my notebook.
“We give him what his body is missing with infusions, hope his procedure goes well, and then wait for these hematomas to go away. Something is happening with his blood to cause this reaction, but we do not know what it is yet. This is a highly unusual case, so we will take it day by day.”
The Moores know rare, but we are not comfortable with it. One might think that with each experience of navigating the unknown, we would form calluses to help us get through the next event. But the previous resistance we have built does not transfer into the new situations. We return to our contact list to update new doctors, we explain new medical terminology to our family, and we help our children (who have never been great at transitioning) begin to transition into the next unknown.
Although, this time it is different. This time we have learned how to ask for help and accept it. This time, we have opened our doors (and broken refrigerator) to our loving and supportive community who continually show up in ways that we didn't even know we needed. We receive daily jokes and riddles to keep humoring our little trooper.
And we don’t know what is coming ahead. We don’t know when he will spend a day without being hooked up to an IV or when he will return to school. We don’t know when he can take off his compression bandages or his Spiderman helmet designed to make those sneaky hematomas go away. We don’t know what is causing this or what it will look like in the months ahead. But we do know how lucky we are to be surrounded by an incredibly strong community.
Not for just this rare adventure, but for every single one we have been through as a family.
And at the end of every long day, after hours of infusions of donated platelets and plasma, we snuggle with our little boy in bed. We reposition his bandages, kiss him right on his squishy forehead, and make sure he peacefully sleeps (with his newly bandaged Bobo to watch over him)
- until we can figure out what this “nothing” really is.