When Dark Thoughts Flooded My Head After My Child's Diagnosis
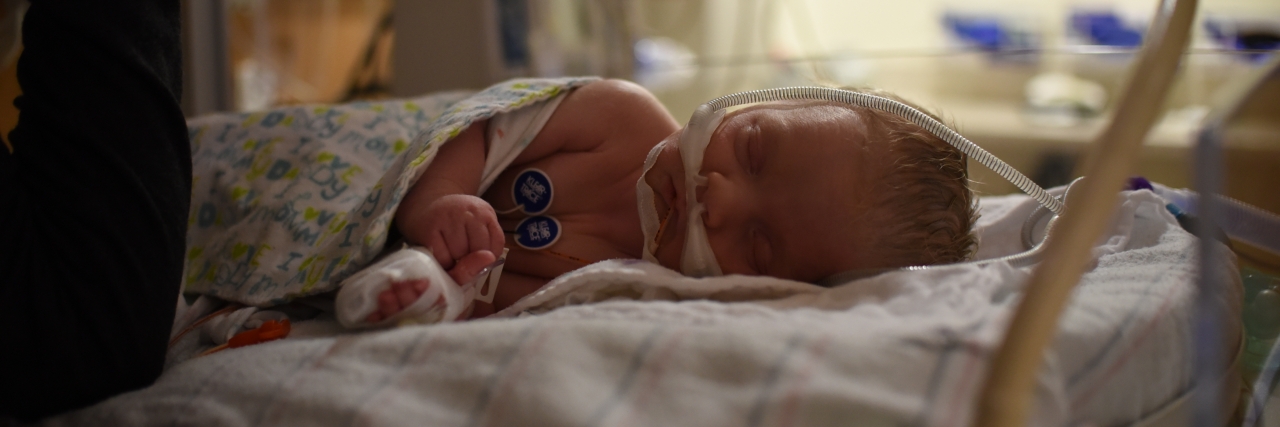
Evan was 4 days old when the NICU doctor finally gave in to our insistent questions. He was full term but couldn’t breathe or eat on his own. Something was wrong.
The doctor hesitated, reluctant. “Have you ever heard of Prader-Willi syndrome (PWS)? We can’t be certain without a blood test, but he seems to meet some of the criteria.”
She put pages she had printed from the Internet on the counter. My husband, Blake, went first. “Don’t read it,” he said through puffy eyes. I read the first bullet point, then waited an hour. A few more bullet points the next hour. I couldn’t handle it all in one sitting.
- Failure to thrive
- Physical, cognitive disabilities
- Anxiety, aggression, behavior issues
- Infertility
Just as I had begun grieving the healthy baby we thought we were having, I grieved the possibility of grandchildren.
- Insatiable appetite, unrelenting hunger
- Morbid obesity
The list seemed endless:
- Skin picking, apnea, speech delays, scoliosis, tooth decay, autism, weak muscles, vision impairments, lethargy, small hands and feet, short stature, seizures, psychosis, slow metabolism.
I moved past the bullet points and on to the pages of text, fumbling through unpronounceable medical terminology. I learned PWS wasn’t hereditary. A small piece of chromosome 15 had broken away — a fluke, a 0.005 percent chance. Why him? Why us?
Words like locked refrigerators and group homes leapt from the page and into the lump in my throat. Then, like a knife…
Life expectancy: 30 years.
No cure.
I looked at my sleeping baby, wondering about his quality of life, then mine and Blake’s lives, too.
That night we were transferred from IU West to Riley Hospital for Children. I looked back at our empty car seat, then ahead to the ambulance we were following, our fragile newborn inside. Exhausted from trying to keep up with the calls and messages from family and friends, Blake created a Facebook group, Team Evan, from the Riley NICU waiting room. Hours passed before we were allowed to see him. The visit was brief, as Evan was too weak to be handled or even open his eyes. We had nothing with us besides the clothes on our backs and a new breast pump, so we decided to go home and try to rest.
Dark thoughts flooded over me as I laid in bed. This cannot be my baby. We will never manage this. How can this be happening to us?
That morning, Blake peeled me off the stairs, where I sat, head in my hands, weeping. He helped me into the car. I can’t go back, I don’t want to go, I protested.
We received our visitor passes and scrubbed in. There was a nurse already working in Evan’s room.
“He had a good night, the night nurse only reported two destat episodes.” We were silent, but she smiled. I wondered what she meant by “destat,” but didn’t have the energy to ask.
“Would you like to hold him?”
Not really, but I didn’t want to seem like a bad mom, so I settled into the recliner while she and Blake untangled his wires and tubes. I studied Evan for a long time, running my fingers through his blonde hair, then along his nasal cannula, feeling the dutiful hum of oxygen pumping through. I looked up at Blake looking down at us. “He’s beautiful,” he whispered, tears in his eyes.
In that moment, a fire lit within me. My dark thoughts turned into I’ll do whatever it takes.
And ever since then, that’s been our mantra. Whatever it takes.
Christmas came and went. We spent three more weeks in the hospital, enduring a series of x-rays, ultrasounds, an MRI, MRV, EEG, exams we had never heard of, pokes and pricks before Evan was deemed strong enough to come home. A few days later, our pediatrician read us the test results over the phone, confirming our worst fears. Whatever it takes, whatever it takes, we reminded each other.
We started early interventions, sought out the best doctors and got plugged in to the PWS community. We read updated and promising research literature. Evan started growth hormone therapy, delivered via needle injection every night, to help him grow. Hope blossomed.

Evan is now 7 months old and aside from gross motor delays, he looks and behaves much like any baby his age. He’s inquisitive, social and starting to get into everything. He lights up our world. His weekly therapies and appointments are well worth the effort. Now that Evan has graduated from his feeding tube and is fairly stable medically, we’re in the “honeymoon phase” of PWS. The insatiable appetite has not yet set in, but that will likely change as he enters early childhood. Each day is a blessing and a challenge. Evan is growing stronger, but we are also one day closer to hyperphagia – when Evan’s brain will trick him into thinking he’s starving. All. The. Time.
Although we are encouraged by current medical advancements, PWS research efforts are grossly underfunded. We ache when we hear about another research study delayed because of lacking funds. We want to see our Evan live life full – not just in his belly, but in all facets of his life. His future depends on this research.
So, in the spirit of whatever it takes, we fundraise. We advocate. We raise awareness. We get loud. And we leave the darkness behind.
To donate and follow this journey, visit One Small Step – Team Evan
Learn more about the incredible research your donations are funding: Foundation for Prader-Willi Research