Women Are Posting Pictures to Challenge a Stereotype About PTSD
The idea started with a disappointing online search. While researching for a piece about trigger warnings, Cissy White realized when she searched for images under “post-traumatic stress disorder” (PTSD), the top results showed exclusively men in uniform.

Given that women are more than twice as likely to develop PTSD than men, White, a writer and advocate, wasn’t only troubled — she was mad. According to the U.S. Department of Veteran Affairs, trauma that could lead to symptoms of PTSD also includes experiencing sexual assault, child sexual abuse, living through a natural disorder and witnessing death or injury. Already in contact with women who live with PTSD through the online community Trigger Point Anthology, based on a book by the same name, she realized if they wanted to be seen on the Internet, they’d have to do it themselves.
Using the hashtag #FacesofPTSD, White, along with Dawn Daum, Joyelle Brandt (co-editors of “Trigger Points”), Arwen Faulknera and Jodi Ortega, started a campaign to do just that.
Now, woman who have PTSD are filling social media with their pictures, hoping next time a woman searches “PTSD,” she’ll land upon a familiar face.
Daum said when she first started doing research about parenting as a survivor of trauma, she found nothing — no advice, no pictures, nothing to let her know there were others like her out there. “I can’t even tell you what that did to my spirit,” she told The Mighty. “I think we associate feeling with what we see, more than we what we feel or hear. We want to look at someone who looks like us to validate how we’re feeling.
In a blog post explaining the campaign, Daum noted that even when you Google “women and PTSD,” you’re left with stereotypes — a woman falling apart, barely holding herself together:
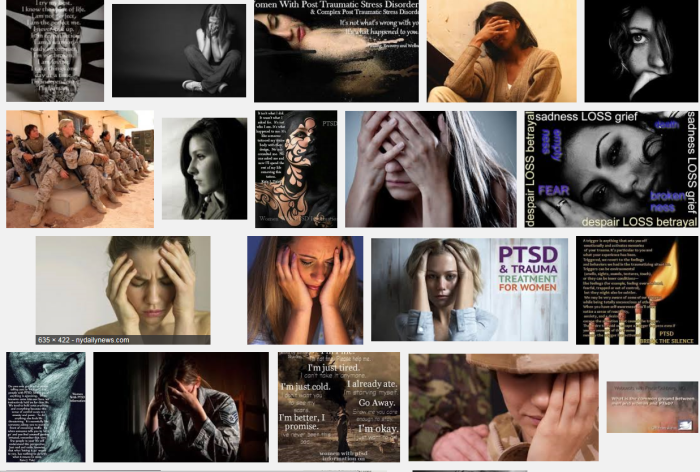
“Those who suffer with PTSD usually do so while raising children, working nine to five and/or taking care of necessary day-to-day tasks,” she wrote. “Survivors are professionals at looking ‘normal’ on the outside… They need to see the real #FacesOfPTSD. Faces that look like mine.”
Check out some of the faces of PTSD below:
#FacesofPTSD Not all wars are fought on the battlefield pic.twitter.com/8TNZ8pEWD5
— Sheila Cross (@Shrye) May 7, 2016
I’ve had #PTSD 30+ yrs.
Finally diagnosed in 2012 (yr this pic taken)
Trauma & Abuse take on many forms#FacesofPTSD pic.twitter.com/OSdGCazvmv— Donia ???? ???????? ♿ (@DoniaLilly) May 6, 2016
This Is Me. #FacesOfPTSD https://t.co/CrJIFo9EEa pic.twitter.com/uCiKB3bXrp
— The Counter Stool (@TheCounterStool) May 6, 2016
#FacesofPTSD Event https://t.co/14eoA01IZW pic.twitter.com/NNwdwOgQKw
— Kelley White (@KelleyLWhite) May 6, 2016
#FacesofPTSD pic.twitter.com/ESYZ3pqHBK
— Xsightable (@xsightable) May 5, 2016
“Not all wars are fought on the battlefield.” Arwen Faulkner #FacesOfPTSD pic.twitter.com/KvqvorsvAe
— Christine (Cissy) White (@healWRITEnow) April 29, 2016
#FacesofPTSD #PTSDAWARENESS #EndTheStigma #semicolonproject pic.twitter.com/SDA7ltz6TO
— Riggs (@KannabisNerd) November 13, 2015
#PTSD is caused by severe trauma – my battlefield, my war was waged at home. #FacesOfPTSD #DomesticViolenceSurvivor pic.twitter.com/WFB3liklvw
— Amy Thomson (@AMarie9619) May 6, 2016
Write to heal PTSD from sex abuse #facesofPTSD #mondayblogs https://t.co/ZkJrX3UfnA @healWRITEnow pic.twitter.com/SGglHxkAzV
— S Burpee Dluginski (@GenfitSheryl) May 9, 2016
What I have accomplished will never define who I am. #StopTheStigma #FacesOfPTSD #SmallButPowerful pic.twitter.com/iAyS3Ha0l8
— Riggs (@KannabisNerd) May 8, 2016
#FacesOfPTSD #EndTheStigma #MentalHealthAwarenessMonth
Not all wars are fought on the battlefield. pic.twitter.com/HNMsA8zXLV— IDropKickedThatChildInSellfDefense (@allie4140) May 7, 2016
“@craftyqueen101: Not all wars take place on the battlefield #FacesofPTSD pic.twitter.com/ghZyvVSxya” #PTSDchat #PTSD Survivor solidarity! ????
— Faces of PTSD (@facesofptsd) May 6, 2016
I am one. #CSA #CSE #DV #Stalking #Gunviolence #Abuse pic.twitter.com/P3Q4ipcU4v
— Dear #Police ???? Please see link in bio. Thank you! (@redtaperesidue) May 6, 2016
Not all wars take place on the battlefield. #FacesOfPTSD pic.twitter.com/hrEqlxCOX2
— Donna Kester (@KesterDV) May 6, 2016
This little girl survived a clandestine war at home. Not all wars take place on the battlefield. #FacesofPTSD pic.twitter.com/eTfESH9h4l
— Laura Parrott Perry (@lparrottperry) May 6, 2016
“Not all wars take place on a battlefield.” – Arwen Faulkenerhttps://t.co/mzjTO2YwPT#FacesOfPTSD pic.twitter.com/tBDavWtTAL
— Megan Lucas (@mjlucintyre) May 6, 2016
#FacesofPTSD pic.twitter.com/Jz8XZCfUTU
— Dawn Daum (@TDawn81) May 6, 2016
To join the campaign, use the hashtag #FacesofPTSD.
What’s one misconception about your mental illness you want to see busted? Tell us in the comments below.
