The Science of Why Strong Emotions Are Harder to Tolerate After Trauma
Editor's Note
The following example is a case study representing multiple individuals. Any likeness to a single person is purely coincidental.
If you’ve experienced domestic violence or emotional abuse, sexual abuse or assault, the following post could be potentially triggering.
You can contact The National Sexual Assault Telephone Hotline at 1-800-656-4673.
You can contact The National Domestic Violence Hotline online by selecting “chat now” or calling 1-800-799-7233.
You can also contact the Crisis Text Line by texting “START” to 741741.
Peter had a rough childhood, dealing with an aggressive father and a submissive victimized mother. He internalized the father’s aggressive ways and mother’s low self-value; he performed to the best of his abilities the role of the mother’s protector, the father’s controller, and the responsible only child. Those circumstances dysregulated his nervous system in an unceasing way, a characteristic that led him to develop complex post-traumatic stress disorder (C-PTSD).
As an adult, he became an aggressive man with low self-esteem, who had no idea how to control his emotions, which shifted from anger to desolation, from despising to neediness, from strong ambition to complete defeat. While having dinner with a colleague he mentioned the frustration of feeling out of control and the colleague told him, “You have to learn how to stay within your window of tolerance.”
“What do you mean ‘window of tolerance?’” asked Peter.
“It’s something I learned in therapy that has helped me a lot but I’m not sure how to explain it. I’ll ask my therapist if she can write something about it and I’ll give it to you.”
So, here I am, writing a comprehensive explanation on what the window of tolerance is for Peter and any individuals who have problems regulating their emotions. In addition to introducing the concept, I’m also including some recommendations on how to use it.
First, it may be useful for people like Peter to know that trauma — complex trauma, in his case — is a disorder that develops from the dysregulation of the autonomic nervous system after experiencing constant stress, fear, confusion and strong emotions that feel overwhelming and impossible to escape or avoid. As a consequence, people like Peter feel out of control because they lack “affect regulation.”
Affect Dysregulation
We use terms all the time even when we are not clear on their meaning. Both terms “affect” and “dysregulation” are an example of this; it may be useful to define them:
Affect is the part of a person’s emotional experience that is “felt;” it’s the physiological manifestation in the body of having an emotion. If the emotion is anger, for example, the affect could be becoming hot and red, shaking, sweating, etc., and the sensations that those changes in physiology feel like. The affect reflects what’s happening internally, in the changes that our nervous system is going through to put us in action or at rest.
Dysregulation is the person’s inability to manage the intensity and duration of negative emotions like fear, sadness, or anger, and the subsequent manifestation of this poorly modulated response that does not fall within the conventionally-accepted range of emotive response. (Beauchaine, et.al, 2007). A person is dysregulated when they can’t find the way to manage behavior and mood, is unable to feel emotions, when the emotions overwhelm the person, and when they remain unresolved and unmanageable for a prolonged period of time.
Affect dysregulation — which is, by the way, one of the most important characteristics of borderline personality disorder (BPD) and post-traumatic stress disorder (PTSD) — is then defined as problems in managing or recovering from extreme states of affect. Affect dysregulation includes underregulation of heightened affect states as well as maladaptive overregulation of affect.
Underregulation involves limited access to strategies that could reduce intense affect states, and associated difficulties with impulse control and goal-directed behavior (e.g., anger that escalates into rage, or anxiety that becomes an unmanageable state of terror).
Overregulation involves limited awareness or clarity of the experience of emotions (e.g. states of profound emotional emptiness or detachment).
Autonomic Nervous System and Levels of Arousal
When we talk about affect or regulation, we are talking about some of the functions of our nervous system — the autonomic nervous system (ANS) in particular. The ANS is in charge of all the automatic functions of the body and of supplying energy to the internal organs including the blood vessels, stomach, intestine, liver, kidneys, bladder, genitals, lungs, pupils, heart, and salivary and digestive glands. It has two branches.
The sympathetic nervous system (SNS) branch is constantly active at a basic level to maintain equilibrium (homeostasis) by accelerating heart rate, widening bronchial passages, decreasing movements of the large intestine, constricting blood vessels, causing pupillary dilation, piloerection (goosebumps) and perspiration (sweating), and raising blood pressure, to name a few of its tasks. It is also responsible for the fight-flight response to prepare the system for protection and to keep you out of danger which is directly connected to the way one could become dysregulated.
The other branch — the parasympathetic nervous system (PNS) and sometimes called the “rest and digest system” — does its part in keeping equilibrium by conserving energy as it slows the heart rate, increases intestinal and gland activity and relaxes sphincter muscles in the gastrointestinal tract. It’s also responsible for defensive actions sometimes called faint, immobilization, collapse, submit (and some other names), and when overactivated, it’s responsible for dissociation of the experience or of the memory. Some people think that it is responsible for “freeze” but that is a misunderstanding. Freeze is actually a defense that uses both branches at the same time — the SNS and the PSN — and it’s normally activated before the FF reaction.
The two branches — sympathetic and parasympathetic — have complementary functions and they normally work by compensating each other’s activation. The sympathetic is in charge of setting you in action while the parasympathetic is the one that calms you down by keeping you — and your organs — at rest. Once you understand that those forces are at work, you can better understand their relationship to affect dysregulation: affect dysregulation means the two branches of the ANS lose their coordination, the whole system loses its equilibrium, and the emotions can easily get out of control.
Optimal Arousal
In regular circumstances, we need a certain level of arousal — a state of increased physiological activity — to function in the world. The activation of the ANS goes up and down in a similar way that our heart rate oscillates. The oscillation of our arousal looks like this:
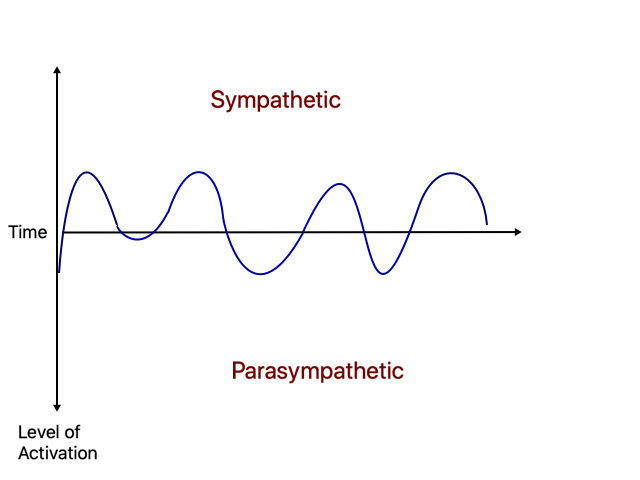
The oscillations in the drawing represent how the ANS goes above the timeline when the sympathetic get activated, and below the timeline when the parasympathetic does. It oscillates because we move between activity and inactivity to balance the use of energy of the brain and system.
Affect Tolerance
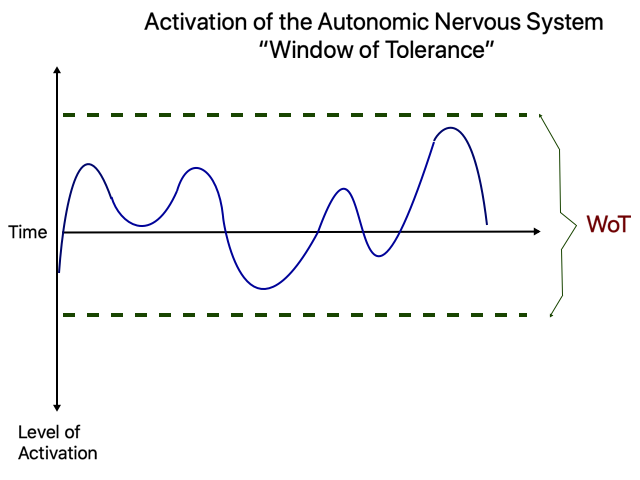
Here the area between the green lines represents what we call the “window of tolerance” (WoT). This “window” refers to the range of activation where the ups and downs are the “normal” or optimal way to function: while in some moments you may feel energized, stressed and even agitated, and in some moments you could feel rested, calm or tired, in either case, those emotional states don’t create distress because can be tolerated and managed. The width for both areas is often different; this means that some individuals can better manage to be “up” than being “down” or vice versa.
Our emotions come and go; they impact our thoughts and cause our mood to fluctuate throughout the day; on any normal day, we may feel stressed or “depressed” without experiencing any type of impairment in our productivity and can continue to do what we have to do in order to achieve our goals. The fact that we can tolerate changes in our mood and emotional states means we each have a certain level of resilience. That resilience is what regulates our tolerance to affect and its fluctuations.
I like using the WoT model to give my clients a graphic representation of the fluctuations of arousal and make it clear that sometimes the level of arousal can go beyond what is normally tolerable and that that’s when the emotional responses feel debilitating or impairing. By having that understanding, it’s easier to monitor our emotional states and identify if it’s getting beyond or below our tolerance in order to revert their path.
After experiencing traumatization, the ANS suffers a series of alterations to its normal functioning that cause states of either:
- heightened activity of the sympathetic (Hyperarousal), or
- a predominant activation of the parasympathetic (Hypoarousal), or
- a pervasive heightened activation of both (Rigid-Stuck or “Freeze”), or
- a constant parasympathetic activity with the withdrawal of sympathetic activation (Tonic immobility), or
- parasympathetic surge (Collapse immobility).
Those states become a person’s way to operate if they develop trauma as a disorder. Most people present one of these states as their most common way of reacting to stressful situations, as if they had gotten stuck in a recurrent way of responding to stress independently of the situation.
After traumatization, the WoT also gets altered. The window normally becomes narrower, and the levels of activation are higher (up or down), meaning that the peaks of the oscillations will be bigger, and the tolerance for affect will diminish.
Hyperarousal
Hyperarousal is a state or condition of physical and emotional tension produced by hormones released during the fight-or-flight reaction. When the stressors activate your sympathetic branch, you will experience emotions like anxiety, anger, fear, disorientation, etc., and your level of arousal could go up to levels that go beyond what you feel you can handle. Hyperarousal outside the WoT feels like overwhelm or helplessness and look like this:
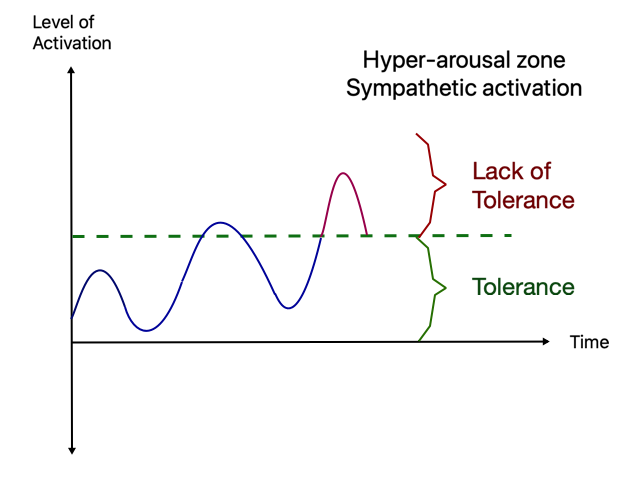
Hypoarousal
When the stressors can’t be handled by the sympathetic, the parasympathetic will get activated in an extreme way in order to solve for the sense of helplessness, leading to feelings of numbness, dissociation, confusion, low energy, disengagement and depression to the point of hopelessness. This is a very dangerous state. It doesn’t seem like it at first sight, but it has severe consequences to the rest of the body, like dissociation, shutting down emotionally, and shutting down physically. If it becomes permanent, it has serious medical and mental implications. This is how it looks using the WoT:
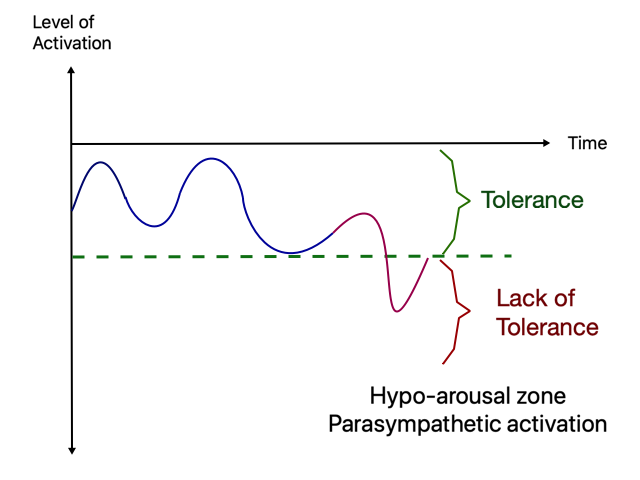
The traditional WoT graph to describe how a person has become less tolerant to experience affect after trauma looks like this:
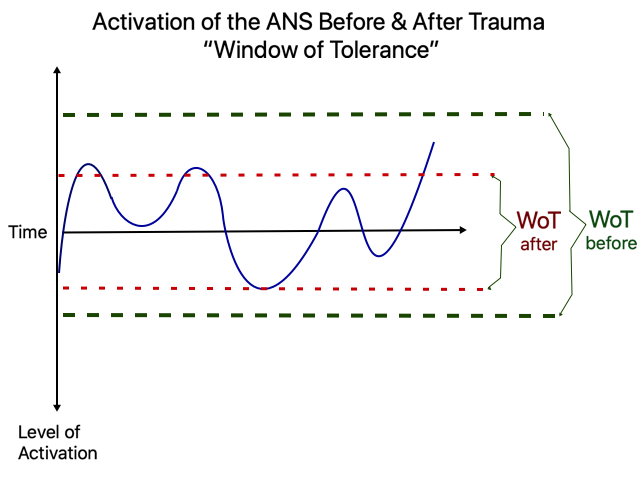
How to Use It
In order to use the window of tolerance model, you need to consider two variables:
● the width of the tolerance band: this includes how much you can tolerate your affect, both in terms of low mood and high mood. What this means practically is that if you get too low if you feel sad or depressed, you will need to widen the tolerance of your low moods; if you get too hyper when angry, you will need to widen your tolerance for hyperarousal.
● the intensity of your mood: besides widening your tolerance, you also need to reduce the intensity of your emotional responses. If you are overreactive, you will need to learn how to control your reactivity. If you feel suicidal when you go down, you need to learn how to not go so down so intensely and understand what emotions are overwhelming your system.
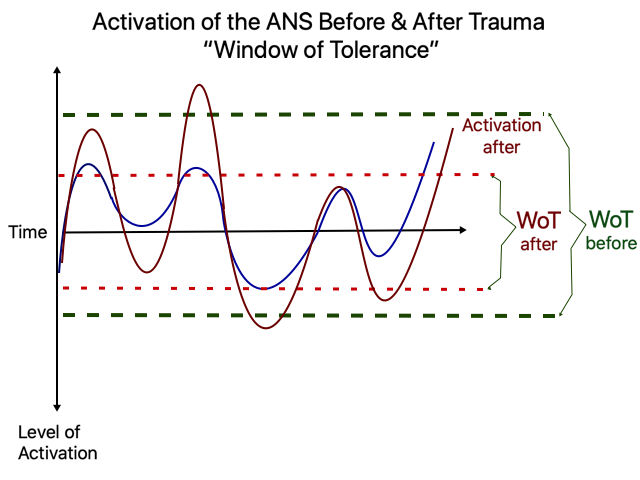
Increasing Affect Tolerance
An effective way to increase tolerance is to pause, breathe, assess and “host” the emotion without acting it out. Pausing is a signal that you need to develop the awareness that you are getting triggered and that it’s necessary to listen to the emotion before it becomes too loud. When we are attentive to what’s happening in our body, the brain understands that one is participating in the decision of how to manage that reaction. If you ignore your affect, then the brain goes automatic without your will. That’s when, as Peter mentioned, one feels out of control. By noticing the affect, the brain activates the part that it’s in charge of, regulating the emotional response. Just by noticing and becoming aware, you are creating more tolerance.
Lowering the Intensity:
When you feel hyperaroused, you can use two strategies to lower the intensity; the first one is:
● social engagement, which is reaching out to someone you trust or cares for you as a way to reduce the emotional reaction. Remember that all those hyperactivations mean that you feel like you’re in danger again, and looking for safety is the best solution. People we trust can provide that safety. It could be the barista at your favorite coffee shop or sending a text to a friend (or therapist). What’s important here is to remind yourself that you have people who can see you and whom you can count on, at least, for the time being.
● the second one is releasing some of the excess energy by moving your body in an intense way: dancing, running, hammering, boxing, kicking, etc. Whatever works for you that helps to put all that fight-flight activation to good use until it bounces back to normal. If you exhaust your energy in something physical, your brain will assume you were able to defend yourself, and it will go back into recovering equilibrium sooner.
When you are hypoaroused, you have to move. You need to tell your brain that you are not defeated and that you rather keep fighting than submitting. Move whatever way you can, slowly at the beginning and more energetically after. You want to have sympathetic activation to compensate for the excess of parasympathetic. You can start bouncing a ball, moving your arms up and down, clapping, and smiling.
Breathing always regulates, increases tolerance and lowers the intensity of the reaction. Never underestimate the power of using breathing as an important technique. There are many apps and devices that can help you learn how to breathe appropriately.
I know by now that Peter has been already applying some of these techniques and understood why he always felt like he was riding a roller coaster. He has developed awareness of the fact that the response he was using around everyone could seem like a threat (a familiar response in many men). He also recognized that the hypoactivation was not necessarily learned from his mother since he never felt like a victim; instead, he realized that the feeling of defeat came from not being able to protect his mother from the aggression. Those were the peaks of hypoactivation he felt every time he saw someone he was not able to help. Hopefully, this article has elements that give words to feelings you’ve had and didn’t understand, extreme reactions that might not be ideal but can morph back into fitting inside the window of tolerance if you develop the awareness of how to get there.
Lead photo by Beniamin Şinca on Unsplash. Graphs via contributor.