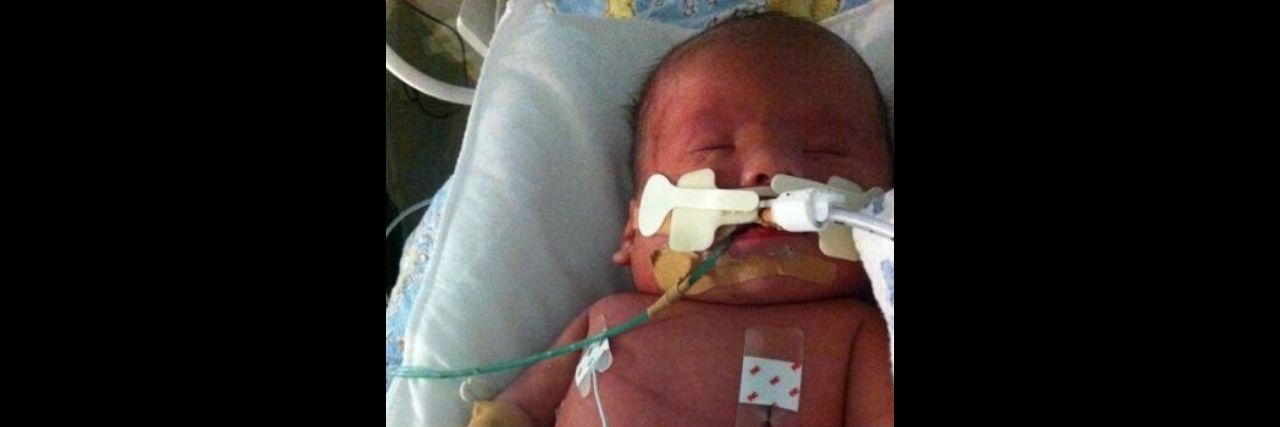
I’ve heard stories from those who were pressured to abort their babies with disabilities, and from those whose children with disabilities were denied adequate care in the hospital. In this blog I’m adding my experience of both, from the perspective of a single mother and an immigrant.
I’m going to be very matter-of-fact in relaying my experience, but please don’t take it to mean that I was not under severe emotional distress during that entire period. I will talk a lot more about that after I get the chronological facts out of the way.
In 2012, I found out I was pregnant one week after I kicked my husband (Noah’s father) out of the house, so I had to carry the pregnancy alone (while also running my restaurant and attending counseling for my marriage breakdown). I showed up at my 20 week ultrasound at the Royal Prince Alfred Hospital (RPAH) expecting to find out the gender of the baby, but instead I was pulled aside by the doctors. They wanted to deliver the “bad news” based on what they saw in the scan (i.e. that the baby had a heart defect as well as a blocked bowel), it was very likely that he had Down syndrome. I was advised to get an amniocentesis test done before it was “too late” to terminate. I knew that the test would be invasive and risky, so I told the doctors that I was satisfied to work with the assumption that my baby did have Down syndrome. I told them that termination was out of the question.
At my next RPAH checkup, the subject of the amniocentesis test was brought up again by a different consultant (a midwife) again, I said I would not go ahead with the test because I planned to keep the baby. She urged me to do it on the basis that it would help me to better prepare for the baby’s arrival if I knew the level of disability he had. Based on what she said, I told her I would think about it.
Over the following days I weighed up the benefit of being able to plan for my baby’s needs ahead of time; I decided it made sense, so I relented. When I attended the next antenatal appointment, I advised the doctor (again, a different person to the previous ones I had seen), that I would like to get the test done. She was excited (as though relieved that I had come to my senses) and said we’d better get this done quickly because we were running out of time.
I corrected her and said I wasn’t doing it with the intention to abort, but rather to find out the level of disability I would need to prepare for, per advised by the last prenatal consultant. She stopped in her tracks and said that an amniocentesis test does not tell you that; it only gives a positive or negative for T21. To this day, I have no idea if it was pure ignorance by the previous person that led me to be misinformed, or if it’s just a symptom of the systemically coercive environment to terminate, that was the experience of my pregnancy. My antenatal consultations were transferred to Westmead Hospital as the doctors felt Westmead Children’s would be better equipped to handle my child’s complex medical issues.
At that point, they detected fluid in his lungs. A subsequent visit showed that the fluids had not resolved and in fact, had increased. I was told my baby was dying and would not survive to term. I was given three options: to let him die in the womb and deliver him stillborn, to have him delivered immediately with no likelihood of survival, or to prolong the pregnancy as much as possible by presenting at the hospital three times a week (from memory) for a few hours each visit, for steroid injections and monitoring of the baby’s heartbeat. I chose the third option.
At one of these visits, the nurse detected that the baby was in distress. I was kept overnight for observation, and the next day, my baby was delivered via emergency cesarean.
Noah was born on May 14, 2012, at 34 weeks gestation with an initial Apgar score of 1 out of 10. He required resuscitation, after which he was warded at The Grace Centre, i.e. the NICU at Westmead Children’s Hospital.
I knew Noah would need lifesaving bowel surgery for his duodenal atresia and lifesaving heart surgery for his AVSD, but it wasn’t until he was born that the term “Hydrops fetalis” was introduced, which is the accumulation of fluids in his organs that caused him to swell up. I would find out through my own research that the mortality rate for Hydrops fetalis was 90%, much higher than that for the other two pre-diagnosed conditions.
There were four head neonatologists on weekly rotation at Grace Ward at the time. As I check the Westmead Children’s Hospital website today, only one name remains (Robert Halliday) that I recognize from our time there. My only interaction with him during Noah’s stay was a positive one, but the same can’t be said of some of the others; I will refer to them as Doctor 1,2 and 3.
Doctor 1 was the rostered head of NICU in the week that Noah was admitted. He sat down with me on the first day with a fairly innocuous assessment of Noah’s condition. He confirmed that Noah had Down syndrome based on his physical characteristics (low set ears, etc.), and that he would need bowel surgery within a couple of weeks and one or more heart surgeries down the track. He said that Noah had fluids in his organs and they would have to wait for that to clear up before they could undertake the bowel surgery. At that point, I knew nothing about the severity of Hydrops fetalis and I thought it was something that would clear up by itself.
The one thing that was somewhat jarring from that meeting was when Doctor 1 told me (I’m paraphrasing), “His bowel, we can fix, his heart, we can fix, but there’s no cure for Down syndrome. Do you understand that?” I get the need to explain medical prognoses in layman’s terms, but I would see with the passage of time, this kind of condescension to be a symptom of something more malicious — which is, basically that the doctors think I’m “stupid.”
That night I received a call while in my room at Westmead Hospital (I was there for three nights post-cesarean) and was told that Noah had taken a turn for the worse. The attending neonatologist advised he would need to insert a shunt into Noah’s lungs to drain the fluids that had built up. The next morning, Doctor 1 asked for another meeting; this time, the prognosis was much more grim. He explained that there’s no fixed cure for Hydrops fetalis, the fluids could be caused by any number of issues and the treatment varied depending on the cause. He said in Noah’s case, the cause was Down syndrome, which made no sense to me and sounded like an excuse to not explore and treat the underlying reason for his fluid buildup. He said it was entirely up to Noah to decide if he wanted to live, and if he did, he would overcome this hydrops by himself.
So I did my own research and found that there had been instances where hydrops was cured through the administration of steroids. I can’t recall if I first brought this up or if Doctor 2 independently told me before I found out this information, but she said there were three different steroids they could try, and they would do so in stages to see if any of them worked.
I was now discharged from the hospital, but driving myself to Westmead to spend on average five hours at the NICU daily. I knew I wasn’t supposed to drive for six weeks after a cesarean but as a single parent with no social supports, I had no other option. I turned over the running of my restaurant to my staff.
I didn’t realize this would be my life for the next seven months.
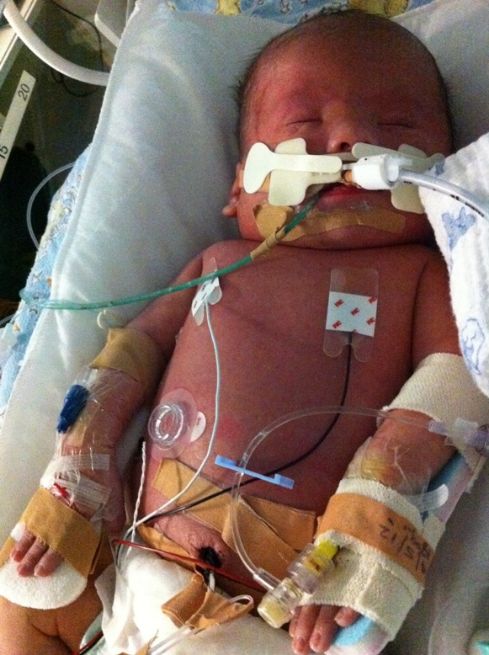
In the meantime, they were shunting fluids from Noah’s organs daily. I asked why they couldn’t do so indefinitely until they found a cure, and they said it wasn’t realistic; at some point the shunt had to be closed off and he would be left to swell up and die unless the fluids cleared up.
The first two steroids did not work. They were down to their final option, Octreotide, when the fluid levels started dropping. I held on to this last glimmer of hope as we monitored the fluid levels every day until it seemed like his Hydrops fetalis was resolved. At two and a half weeks, they were now ready to operate to repair his duodenal atresia. This was major surgery but I was told Westmead Children’s had the best bowel surgeon in the world, and Noah was in good hands despite his very fragile state. He was down to 2.2 kg, or 4.8 pounds, after all the fluids had drained from him. Noah seemed to be doing as well as you would expect when he came out of surgery, so I went home. At about 3 a.m. I received a call from Doctor 2 to advise that Noah’s condition had deteriorated. I drove to the hospital immediately. I found out his lactic acid levels post surgery had been climbing hourly and it was now at pre-death levels.
Nothing they tried was working; Doctor 2 argued with the surgeon to cut Noah open again because they were wondering if there had been a mistake and someone had left some surgical material inside his body. He refused because Noah would not survive another surgery. When I arrived at the ward, they took another reading and for the first time, the lactic acid level did not go up. At the next reading, it went down and it kept going down until he was out of danger. Over the next two weeks, Noah’s body started to look puffy. I thought he was just gaining weight. I received another call in the middle of the night, it turned out that the hydrops had returned and this time the fluids in his body had become infected.
The night shift neonatologist told me to expect the worst. Hydrops past the 30-day mark is not survivable, he said. Noah’s was past the 30-day mark. Doctor 3 asked for a meeting, from her tone she sounded like she thought I was suffering from delusion. She said, “I don’t know if you don’t understand this but hydrops plus Down’s is just not survivable. You need to make arrangements for his death.” As I was always visiting Noah alone, she asked if I had a friend who would be able to stay with me and perhaps film me holding Noah in my arms as he died. For the memories, you know. I had just finally, after a month of trepidation, sent off Noah’s birth registration form, and I realized that his birth certificate would arrive in the mail after he was dead. I talked to Doctor 2. They were treating Noah with antibiotics to clear the infection but they were out of options regarding the fluids otherwise. I reminded her that they had taken him off all medications including Octreotide in the lead-up to the bowel surgery, and asked if they could put him back on it.
She agreed. And Noah’s hydrops started clearing up again.
Then his heart started failing sooner than they had hoped. Dr. Halliday had told me early on that the plan was for him to go home after recovering from bowel surgery, and come back in a few months or even a couple of years for his heart surgery. Now it looked like that wasn’t going to be the case.
Doctor 2 called for a meeting. She said that they were running out of places from which to draw blood from Noah (which they had to do more than once a day for testing) and she asked how I felt to hear him scream as they pinned him down to do so (sometimes with my help) when he only had about two cups of blood in him (a fact that a different doctor in NICU later disputed). Could I bear to see him suffering?
She said she wanted to check in because most NICU parents start to question the wisdom of continuing treatment when they’re at the 6-8 week mark, and they start to feel that they need to get their life back on track. She wanted to give me the option to withhold treatment and let him die. I said that wasn’t me, and I didn’t care about the screaming, I wanted them to throw the book at Noah when it came to saving his life.
Nonetheless, I left the hospital questioning my judgement, until that Saturday, a lovely teenage boy came up while I was busy at work (I had gone back to working on Saturdays) and just loitered around, so I struck up a conversation with him. I knew through his mom that he had been sick as a baby and spent a year in hospital so I asked him if he remembered or was traumatized by the painful treatments they administered and he laughed and said “no,” and that reassured me that I had made the right call with Noah.
Noah was too small and fragile for AVSD repair. At two months they performed his first heart surgery for pulmonary arterial banding to help see him through until he was strong enough for the full procedure. They waited a few more weeks but he was never completely stable.
At three months, Doctor 1 asked for a meeting with me. This would prove to be the defining moment of Noah’s time at Grace Ward. The situation was that Noah’s heart had started failing again as it looked like the banding did not achieve the purpose of buying him more time. He wasn’t getting any stronger and Doctor 1 didn’t believe he ever would. It was now or never with the full AVSD repair. And if they were to do it now, because of his frail state, they would need to hook him up to an ECMO machine. This, in turn, would cause irreparable brain damage. Noah would be a vegetable the rest of his life.
He also said:
- He had seen children with Down syndrome grow up to be productive members of society. It was his opinion that Noah was never going to be one of them.
- If I decided to go ahead with treatment, my life as I knew it would never be the same. I would have to give up everything to take care of Noah.
- I wasn’t getting any younger. Who was going to look after Noah when I was gone?
- The government would be burdened with the cost of taking care of Noah for life.
Doctor 1 said that he had been observing me and he recognized I’m the sort of person who never gives up. He said this wasn’t about giving up but “giving in.” I said no, if the only options were to let him die or to operate now, I wanted them to go ahead with the operation.
Doctor 1 called the heart surgeon into the room. She looked horrified and said no, she and her team refused to operate on Noah because in his current state it would kill him. She said she wasn’t going to play the role of executioner.
Doctor 1 was visibly enraged. He told me that in that case, he was going to get things moving to eject Noah from NICU.
He said:
- They had run out of ideas on how to treat him.
- At three months he was technically no longer a neonate anyway.
- And “to be blunt about it,” (his words) they needed the bed back (despite the fact that the NICU ward wasn’t full).
He said, if it was any consolation, perhaps a different medical team in the next ward could come up with a breakthrough.
A nurse had to quietly reassure me that it wasn’t a simple matter of kicking Noah out of NICU; they had procedures to follow to make sure there was a bed for him at PICU, so it wasn’t like we would be left out on the street. I relayed the conversation to Doctor 3 and she agreed Doctor 1 had stepped out of line and not only that, but that he had been known to impose his own beliefs on patients in the past and she was going to have a word with him. I never crossed paths with either doctor after that, because Noah was transferred out of NICU within a day or so.
I didn’t fight to keep him there because I didn’t want to compromise my son’s care by leaving it in the hands of professionals who didn’t think he was worth saving. Miraculously, the PICU team did come up with a breakthrough and at five months, Noah was finally strong enough for his open heart surgery for AVSD repair. He came home one week before Christmas 2012 after spending the first 217 days of his life in hospital.
Contrary to the doctors’ doom and gloom even as Noah left the hospital, i.e. that the rest of our lives would be spent in and out of the emergency ward because of his fragile health, Noah has thrived. All of the residual holes in his heart have healed without need for further surgery, and he’s the happiest little kid I know.
From the moment I found out my child had Down syndrome, I spent some 300 days fighting medical odds for my son’s survival. This was exacerbated by simultaneously having to fight a hospital system that seemed hellbent on pressuring me to give up at each turn, and the truth is, I don’t think the fight will ever end.
Soon after his discharge, during a visit to a medical center, the attending GP took one look at Noah and said , “What’s wrong with him?” When I replied that he has Down syndrome, she asked incredulously, “Didn’t you get the test done?” I said, “yes” (though what I meant was that I knew prenatally that he did have DS) and her response, “Oh, so the test failed?”
I made a choice to “hold it together” during this period, because I had a business to run and staff to lead; some of the medical staff interpreted my stoicism as stupidity.
“There’s no cure for Down syndrome, you know.”
“He has pulmonary hypertension. That’s not a good thing. That’s a baaaad thing.”
“I don’t know if you don’t understand this, but your baby isn’t going to survive. You need to make arrangements for his death.”
When Noah first came home from the hospital, I struggled to talk about our experience without falling apart. I figured it was just a matter of time before I could do so comfortably and casually. That has not been the case.
It’s been seven years and I’m still struggling; it still keeps me up some nights. It affects my relationship with medical professionals and with society at large (e.g. when anyone insinuates that I’m a bad or inadequate parent).
This blog is too long as it is, but it’s only a part of a larger picture of what I went through with Noah.
I’m hoping that by sharing my experience, future parents can be better prepared for the insidious eugenics practiced by some in the medical profession here in Australia, accept that doctors often get things wrong, and claim their right to stand up to them when they do.
Photo submitted by contributor.