A Guide to Psoriasis: What You Should Know About This Skin Condition
Over 7 million people within the United States live with psoriasis. Yet, in many ways, psoriasis is still a largely misunderstood and overlooked health condition. In fact, most people don’t even realize that August is Psoriasis Awareness Month. So, in honor of Psoriasis Awareness Month, let’s take a closer look at this frustrating, yet underrepresented, chronic health condition.
What Is Psoriasis?
Psoriasis is a chronic autoimmune skin disease. Researchers believe that dysfunction within the immune system speeds up the growth cycle of a person’s skin cells. This rapid turnover of skin cells causes dry, scaly patches to appear all over the affected part(s) of the body.
Unfortunately, the cause of psoriasis is still unclear to doctors and other researchers. However, because it is an autoimmune-type disorder, it is not contagious. Furthermore, psoriasis is not typically considered life-threatening for most people.
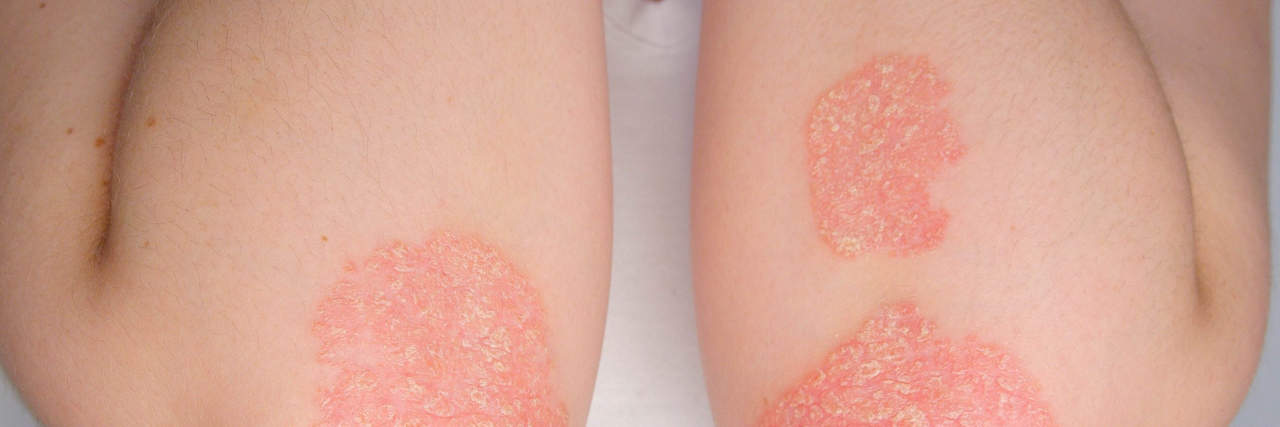
Typically, psoriasis forms scales that are a whitish-silver color. These scales develop in thick, red patches. However, people with darker skin tones may experience psoriasis that looks more like purple or dark brown scales. Regardless of the color or general appearance, psoriatic patches will crack and bleed.
Some people with psoriasis say that the psoriasis plaques on their skin burn, itch, and sting. The inflammation caused by psoriasis can also affect tissue and organs in other parts of the body, and people with psoriasis often experience other chronic health conditions alongside their psoriasis.
Types of Psoriasis
According to the Mayo Clinic, there are six main types of psoriasis. Each one affects a different part of the body and looks slightly different in terms of presentation. People can also experience more than one type of psoriasis.
Plaque Psoriasis
Plaque psoriasis is the most common type of psoriasis, with up to 80 percent of all psoriasis patients having plaque psoriasis. It causes raised skin patches of dry, itchy skin that is covered in scales. Plaque psoriasis usually appears on a person’s elbows, scalp, knees, and lower back. It can appear in different colors, depending on the person’s skin tone.
Inverse Psoriasis
Inverse psoriasis is also fairly common, with nearly one-quarter of all people with psoriasis living with this type. It causes patches of smooth, but inflamed skin that usually gets worse when the person sweats or the affected region experiences some type of friction, such as with clothing. Inverse psoriasis mainly affects areas of the body such as a person’s breasts, buttocks, and groin.
Nail Psoriasis
Nail psoriasis affects the fingernails and toenails. It causes abnormal nail growth, discoloration, and pitting of the nails. In some cases, psoriatic nails loosen and separate from the nail bed or even crumble.
Guttate Psoriasis
Guttate psoriasis is usually triggered by a bacterial infection such as strep throat. It causes small, drop-shaped scaling patches of skin on a person’s arms, legs, and trunk.
Pustular Psoriasis
Pustular psoriasis is a more rare type of psoriasis, but it can be one of the most difficult to deal with. Pustular psoriasis stands out due to the pus-filled blisters the condition causes, and these blisters can appear in isolated regions or all over the body.
Erythrodermic Psoriasis
Finally, the rarest type of psoriasis is called erythrodermic psoriasis. It usually covers the entire body, and causes a peeling rash that itches or burns intensely. This can occur as a short-term breakout (called an acute case) or as a long-term (chronic) condition. Erythrodermic psoriasis is also the one form of psoriasis that is considered life-threatening.
Symptoms of Psoriasis
Like many other autoimmune disorders, the symptoms of psoriasis can vary from person to person. In general, though, common symptoms of psoriasis include:
- Inflamed skin patches that can be red, purple, brown, or purple in color
- Scales or plaques on the colored patches of skin
- Dry, cracking, or bleeding skin
- Soreness, particularly around the patches
- An itching or burning sensation around the patches
- Thick nails that are also pitted
- Swollen, painful joints
Not everyone will experience all of the above-listed symptoms, and some people may even have additional symptoms due to secondary health conditions caused by psoriasis. Also, the areas (called patches) of psoriatic skin can appear as small areas or cover large regions of the body. Also, people can experience periods of “remission,” where they exhibit no symptoms at all.
Psoriasis Triggers
Most people with psoriasis experience “cycles” of symptoms. The symptoms can be severe, clear up, and become severe again within just a few weeks. This often happens because of the various triggers that can lead to a “breakout” in symptoms.
Common triggers for psoriasis include:
- Stress
- An infection or illness
- Alcohol consumption
- Injuries such as cuts or scrapes
- Certain medications
- Sunburns or prolonged exposure to the sun
- The weather
Although triggers can vary from person to person, identifying your personal triggers can help you better manage your symptoms.
Treatment Options
Unfortunately, there’s no cure for psoriasis. In fact, doctors are still learning a lot about the condition and how it affects the body. However, there are treatment options out there that can slow the growth of skin cells, remove plaques, and reduce inflammation and scales. These treatment options include topical treatments such as corticosteroids, moisturizers, or retinoids, medications such as methotrexate, and light therapy.
Luckily, psoriasis can be diagnosed fairly easily. You can start by seeing your primary care doctor, who will likely refer you to a dermatologist. The condition can mostly be managed with the treatment options listed above, but you should see a doctor if your symptoms suddenly worsen or you are experiencing pain.
Life with psoriasis can be frustrating and discouraging. However, bringing awareness to this condition can help people feel less alone.