Symptoms of Parkinson's Disease
Editor's Note
The Mighty’s Condition Guides combine the expertise of both the medical and patient community to help you and your loved ones on your health journeys. For the Parkinson’s disease guide, we interviewed seven medical experts, three patients, read numerous studies and surveyed nearly 400 people diagnosed with the condition. The guides are living documents and will be updated with new information as it becomes available.
Other sections of this Condition Guide:
Overview | Diagnosis | Treatment | Resources

What you’ll find in this section:
Hallmark Motor Symptoms | Non-Motor Symptoms | Early Onset Parkinson’s Disease | Sex Differences: How Men and Women Experience Parkinson’s Disease | Factors That Can Affect Symptom Severity | Stages of Parkinson’s Disease | Causes of Parkinson’s-Related Death
This section was medically reviewed by Kristin Andruska, MD, PhD, Head of the California Movement Disorders Center

Understanding Parkinson’s Disease: What Does Parkinson’s Disease Feel Like?
Parkinson’s disease is a neurodegenerative disease caused by a lack of dopamine produced in the substantia nigra — the part of the brain that controls your voluntary movements like swinging your arms or walking. The lack of dopamine, combined with the effects of a protein found in the brain called a-synuclein forming toxic clumps, and the loss of neurons, communication cells in other parts of the brain and nervous system, causes a wide range of symptoms. It’s important to remember, though, that not everyone with Parkinson’s disease experiences all possible symptoms. Each case is unique.
What is Parkinson’s Disease?
Signs of Parkinson’s Disease
Parkinson’s symptoms can be divided into two categories: motor symptoms and non-motor symptoms. Motor symptoms involve changes in how you move your body, and non-motor symptoms are other symptoms not related to movement. Both types of symptoms can be equally difficult to deal with. Until recently, doctors primarily focused on treating motor symptoms. Symptoms can vary in how severe they are from day to day — you might feel better one day and worse the next, or even better in the morning and worse later in the day. Severity also depends on how effective your medications are.

Hallmark Motor Symptoms
The term “motor symptoms” describes symptoms related to movement and changes to how you’re able to move or control your body. There are three hallmark symptoms doctors look at to determine if you have Parkinson’s disease:
- Tremor
- Slowness of movement
- Rigidity in your muscles
If you have a certain combination of motor symptoms, plus a few additional findings (for example, how well you respond to medication) and you do not also meet criteria that suggest you may have a different diagnosis, then you will likely be diagnosed with Parkinson’s disease.
Tremor
A tremor is described as an uncontrolled shaking of a limb, typically your hand, foot, leg, jaw or head. This shaking occurs when you’re not using the limb, meaning the shaking stops when you purposefully move the tremoring part of your body. The tremor often starts on one side of your body, and almost always spreads to both sides.23 This is because the breakdown of dopamine-producing cells that cause your tremor tends to start on one side of the brain, and gradually progresses to both sides.
Bradykinesia
Another term for bradykinesia is “slowness of movement.” In other words, you can’t move your body as fast as you would like. This often becomes apparent through everyday tasks that require fine motor movement, like combing your hair or buttoning clothes.13 You may notice when you try to brush your teeth, for example, you can’t move your arm and hand very fast. Like tremor, you’ll typically notice the slowness of movement starts on only one side of your body in the beginning of your disease progression.
Rigidity
Rigidity is stiffness in your body. It feels like really tight muscles that you can’t extend or relax like you used to.19 For example, you might feel like you have a frozen shoulder or no longer naturally swing one of your arms when you walk. You might chalk up these stiffness symptoms as “arthritis” or “getting older” and may not think too much about it initially, but a neurologist will ask about it on an exam.23

Other Parkinson’s Motor Symptoms
There are several other common Parkinson’s motor symptoms. These are related to the three hallmark symptoms of Parkinson’s and are often included in a doctor’s evaluation of whether or not you have Parkinson’s. These include:
Problems With How You Walk
A few characteristic Parkinson’s gait or walking patterns are a slow, shuffling pace; not picking your feet up very high off the ground or dragging your feet; having difficulty turning; and “festination,” which is when you are walking, steps get progressively smaller and faster.
Freezing
You likely won’t experience freezing until later on in your Parkinson’s progression. You feel as though you are “stuck” or “frozen” in one place and can’t move one foot in front of the other or start the first step. It tends to happen in places where you have to go through a door or turn or you are in a crowded environment or narrow space. Freezing is more than just a motor phenomenon — it involves having less cognitive control over walking. Just because you want to move doesn’t mean your brain can make it happen, because changes in your neurons make it difficult for you to tell your body to move like you used to. Freezing also includes changes in how you normally walk — your gait might not be as smooth and even — as well as an emotional component, meaning freezing can be affected by stress or anxiety.10
Difficulty Balancing
When standing or walking, you might lose your balance or fall more easily than you used to. Like other movement or motor Parkinson’s symptoms, your balance will get worse as the disease progresses. Balance problems are caused by a variety of factors, including stiffness in your body, slowness of movement, freezing, and not having a grasp of your own body position and movement.
Micrographia: Having Small Handwriting
Having small handwriting may seem like an unexpected aspect of Parkinson’s, but it is quite common. Many people actually experience this symptom as one of their first signs of PD, years before other movement symptoms arrive. It is literally what the name describes: When you hold a pen or pencil and write on a sheet of paper, your numbers and letters are very small and “cramped”-looking. It is caused by a lack of dopamine in the part of your brain called the basal ganglia, which helps start and control your movements.25 Without dopamine, the neurons in the basal ganglia cannot communicate with each other to produce smooth, controlled movement.
Lack of Facial Expressions
A lack of facial expressions is called “masked face,” where you don’t make facial expressions like you used to and appear to have the same expression despite changes in your mood. You might look unemotional even if you are still having many emotions. Masking is caused when the muscles in your face become rigid and unmoving, similar to muscles throughout the rest of your body.
Stooped Posture
Some people with Parkinson’s develop a common stooped posture, which includes hunched shoulders, a rounded back, dropping your head, bended knees, and/or leaning forward. It’s not clear exactly what causes stooped posture, but it is likely a combination of factors like body stiffness, a side effect of medication, tightening muscles along your back and spine, muscle weakness and not being aware of your own body position.6

Non-Motor Symptoms
Parkinson’s can cause symptoms that don’t have to do with changes in your movements and can show up months or even years before motor symptoms. The “prodromal” phase of Parkinson’s occurs early on when you have non-motor symptoms without severe enough motor symptoms to make a diagnosis. This stage can last for decades.16 This phase is often characterized by symptoms unrelated to your ability to move your body. Even after motor symptoms appear, non-motor symptoms continue to be a part of the disease. Non-motor symptoms can be just as difficult to live with as motor symptoms (sometimes more so), and in the last 10 years or so, doctors have begun treating non-motor symptoms more regularly than they used to in decades past.23
Difficulty Sleeping
Sleep difficulties are common when you have Parkinson’s. You might not get good quality sleep or you may struggle to get enough sleep each night.4 This could be caused by a couple of different factors like medication side effects, related conditions like depression, needing to urinate during the night, not being able to move comfortably in bed, and the condition itself because neurons break down in the parts of your brain that control sleep patterns.21
One common sleep issue you might experience with Parkinson’s is REM sleep behavior disorder. REM sleep behavior disorder causes you to move in your sleep and act out dreams. For example, you might kick your legs or move your arms in a way that coordinates with what you are doing in your dream. Usually, during REM sleep, your body movements are automatically shut off to prevent you from getting hurt by acting out your dreams. REM sleep behavior disorder commonly occurs with Parkinson’s disease and other neurodegenerative disorders — one study found of over 1,200 people with REM sleep disorder, 73% developed Parkinson’s within 12 years.18
Cognitive Issues
Cognitive issues are when you have trouble processing information. This can manifest as problems with thinking and memory. You might feel like you have to wait for your mind to process auditory, written or verbal information — as if you were waiting on slow internet service.4 You also may experience difficulty with word-finding. Multitasking, like talking and walking at the same time, can be a challenge too.7 This is because it requires you to shift attention from one task to another.
Chronic Pain
Parkinson’s symptoms can cause chronic pain. You might experience joint pain, like your joint has limited motion or a pulling sensation; a tight or shooting pain sensation in your lower back and legs due to stiffness or rigidity; and central pain, which is pain caused by damage to your central nervous system (this encompasses your brain, brainstem and spinal cord). This causes a searing, burning sensation in the hands, feet, arms or legs that makes it painful to be touched.4
Apathy
Apathy is characterized by a loss of motivation to do things. You don’t feel like you have the energy to get up and participate in any of your usual activities, including social activities, leaving the house, and even basic things like showering or getting dressed. You may struggle with not feeling a “drive” to be active.4 You might also feel emotionally “flat.”
Seborrheic Dermatitis
If you have Parkinson’s you may experience non-motor symptoms on your skin. Seborrheic dermatitis is a skin condition that can happen when your immune system gets overactivated and causes swelling or irritation that some people with Parkinson’s experience. It causes scaly patches and red skin on the scalp, face, upper chest and back, which are areas of your skin that produce sebum, an oily substance that helps moisturize your skin and hair. When too much sebum is produced, that’s when the symptoms of seborrheic dermatitis occur. We don’t know for sure why Parkinson’s may lead to seborrheic dermatitis, but one theory is that it is caused by issues in your autonomic nervous system, which controls many of the body’s functions like sweat, saliva and tears. Issues with functions controlled by your autonomic nervous system are a common symptom of Parkinson’s disease.24
Parkinson’s Disease Dementia (PDD)
It can often be confused with other types of dementia, but Parkinson’s disease dementia (PDD) is a specific symptom of Parkinson’s itself. In PDD, the symptoms of dementia (a condition that causes you to lose mental functioning like your memory) are caused by Lewy bodies, or abnormal clumps of the protein a-synuclein, that form in the brain. These harmful Lewy bodies lead to symptoms like loss of memory, confusion, difficulty concentrating, irritability, and changes in sleeping patterns and appetite, along with motor symptoms similar to regular Parkinson’s movement symptoms.
Lewy bodies are a hallmark feature of Parkinson’s disease in general. Over a course of 20 years of living with Parkinson’s, most people (around 80% or more) will develop PDD. It’s unknown why some people with Parkinson’s go on to develop PDD and others don’t. Older age, a family history of dementia, experiencing hallucinations and delusions earlier in your Parkinson’s progression and having Parkinson’s for a long time appear to be risk factors.5 Parkinson’s dementia is sometimes confused for Lewy body dementia because the two conditions can look quite similar. However, Lewy body dementia is a separate condition.
Mental Health Symptoms
Mental health symptoms like depression and anxiety are common in Parkinson’s disease not just because of the stress of having a chronic illness — they can also be caused by the condition itself. This is due to the loss of neurons in systems of your brain associated with mood.14 You might feel emotional or hurt by situations that wouldn’t ordinarily be an issue.7 In addition, some medications for PD can have depression, anxiety and impulse control disorders as side effects, or as a symptom of medications wearing off.15 Feeling anxious or upset could also make your PD symptoms feel worse.
Other non-motor symptoms can include:
- Soft voice or slurred speech
- Constipation
- Loss of smell
- Orthostatic hypotension, or a drop in blood pressure after standing up
- Sexual dysfunction, including erectile dysfunction and hypersexuality in men and loss of lubrication and involuntary urination in women3
- Urinary incontinence
- Vision problems, including double vision, reduced blinking resulting in dry eye, trouble with spatial awareness and less ability to recognize faces.1 (Technically, this is considered a motor symptom because it is caused by a loss of eye and eyelid movement, but you’ll experience it more like you would a non-motor symptom.)
- Fatigue
- Drooling
- Excessive sweating
- Hallucinations and delusions
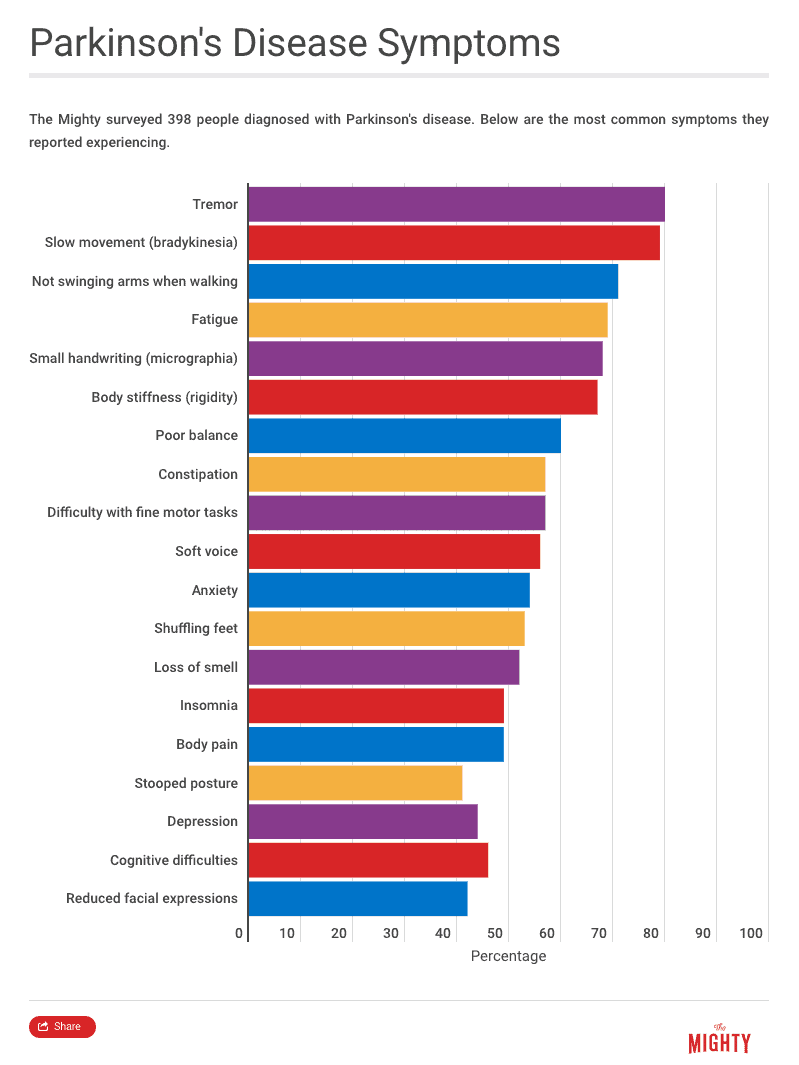
Related: Here are some ways people describe the symptoms of Parkinson’s
- 7 Early Symptoms People With Parkinson’s Disease Noticed First
- How I Fight the Apathy That Can Come With Parkinson’s Disease
- When I’ve Fallen and Can’t Get Up Because of Parkinson’s Disease

Early Onset Parkinson’s Disease
Early-onset PD is defined as anyone diagnosed under age 50, which represents 10-20 percent of cases. The symptoms of early-onset Parkinson’s are generally the same as when you get it later on but tend to be less severe if you are younger.17 However, you are more likely to have dystonia (involuntary muscle contractions) and dyskinesia (involuntary movement as a result of taking the medication levodopa, depending on your dosage) if you have early-onset PD.11
The disease also tends to progress slower if you’re diagnosed at a younger age. You are more likely to remain in the phases before you experience significant disability longer than people who are diagnosed at older ages.8
As a younger person with PD, you may feel the effects of symptoms differently since you are in a different place in your life than an older adult. For example, a tremor may impact your ability to perform certain jobs, or having very slow movements may make it difficult to play with your kids.10 It’s important to remember that there are several different types of medications that can dramatically improve your symptoms, as well as lifestyle changes and exercises that help keep you functioning and living a full life.
Related: These articles share what it’s like living with early-onset Parkinson’s.
- How My Childhood Parkinson’s Disease Diagnosis Transformed Me Into an Advocate
- Choosing Parenthood With Juvenile Parkinson’s Disease
Sex Differences: How Men and Women Experience Parkinson’s Disease
Parkinson’s has not typically been thought of as being different for men and women, but the medical community is starting to recognize some possible sex differences in terms of symptoms and your overall experience with the condition. Motor and movement symptoms are generally the same for all genders. However, women may experience more anxiety, depression and other non-motor symptoms and may experience changes in their menstrual cycle with PD symptoms.10 Women may also experience some different side effects to medications.4 There’s still a lot physicians don’t yet understand about sex differences, and more research is needed.

Factors That Can Affect Symptom Severity
One of the challenges of Parkinson’s is the severity of your symptoms can change from day to day due to a few different factors. One is sleep quality. If you get a good night’s sleep and prioritize sleep as part of your daily routine, you might find your walking, balance, stiffness, ability to think, process and remember information, and mood are better than if you had a bad night’s sleep.4
Another factor is your eating schedule. You might discover the timing of your meals affects how your medication is absorbed and thus how effective it is. For example, if you eat a high-protein meal around the same time you take your levodopa medication, you might feel less benefit from your medications.4 Stress can also cause symptoms to flare and medications to be less effective. As your stress levels decline, you may find your symptoms are more manageable.19 Traveling can increase the severity of your symptoms since it often throws off your sleep, eating, stress levels and medication timing.4 Finally, exercise can impact your symptoms in a beneficial way — it can help limit your symptoms in the short term, and has protective effect that can help slow down the progression of your disease over the long term.

Stages of Parkinson’s Disease
Parkinson’s disease is progressive, which means over time, symptoms get worse. However, its presentation and rate of progression differs from person to person. You may experience a very slow progression, with symptoms more like an “annoyance,” while others progress with worsening symptoms quicker.27 There is currently no proven way to predict how quickly you will progress. Experts think if your most significant symptom is a tremor, you may progress slower, whereas if you have more challenges related to rigidity, stiffness and balance, you may progress faster.11 Some genetic types of Parkinson’s may have different progressions, too. Scientists are continuing to research this area of Parkinson’s.
Parkinson’s disease can be organized into rough “stages,” which give you and your physician a common language to describe your functioning. There are two scales doctors use to determine which stage of Parkinson’s you are in. The first is called the Hoehn and Yahr scale. It was originally published in 1967 in the journal of Neurology by Margaret Hoehn and Melvin Yahr. It divides Parkinson’s into five stages, based only on motor symptoms:12 The five stages are:
- Stage 1: Motor symptoms on one side of your body that don’t affect your daily activities
- Stage 2: Motor symptoms on both sides of your body, but you’re still able to balance
- Stage 3: Balance difficulties and unsteadiness, some limits to what you can do in your everyday life but still physically capable of leading an independent life
- Stage 4: You are still able to walk and stand (often with a mobility aid), but your disability really impacts what you’re able to do
- Stage 5: You are unable to walk and must use a wheelchair or remain in bed
There isn’t a set time frame you stay in each stage, and there is no definitive linear progression for everyone, though the scale gives a general outline. In addition, if you have movement fluctuations where sometimes you are able to do more physically than other times, you can vary in your stage — for example, you might be in stage 4 when your medications are not working but in stage 2 or 3 when your medications are working.11
The other scale doctors use is the Movement Disorder Society-Unified Parkinson’s Disease Rating Scale (MDS-UPDRS), which factors in non-motor symptoms as well as motor symptoms.9 It is a four-part scale that includes patient-directed questionnaires about how you experience your symptoms, as well as a physician-directed movement disorders neurologic exam. The questions include five response options, from 0 to 4, with 0 being “normal” and 4 being “severe.” It consists of four parts.
Part 1 includes questions about non-motor aspects of daily living, like daytime sleepiness, pain, urinary problems and lightheadedness. Part 2 includes questions about motor aspects of daily living, like speech, swallowing, handwriting, walking and getting out of bed. Part 3 is a motor examination that checks symptoms like your rest tremor, walking patterns and rigidity. Part 4 looks at motor complications, like time spent in the “off” state (time when your medications are not working) and time spent with dyskinesia (uncontrolled movements you may develop from using the medication levodopa for a long time). Once completed, the MDS-UPDRS scale can make it easier to track your motor state, progression over time and response to medications.11
You may find it helpful to know which stage you are in or you may find it stressful. Since the progression of Parkinson’s can vary so much from person to person and is so hard to predict, it’s most productive to stay positive and focus on managing your symptoms as well as you can right now, rather than anticipating a certain future.23
Related: Read this story for more insight on the what it’s like having a progressive disease.

Causes of Parkinson’s-Related Death
Parkinson’s disease is not considered a terminal condition, and many people live well for years or decades after their diagnosis. When Parkinson’s-related death does occur, it is typically not due to Parkinson’s itself, but related to complications caused by a few specific symptoms. One is difficulty swallowing, which can lead to inhaling food into the lungs that can cause pneumonia. Another potentially life-threatening symptom is difficulties with balance and walking, leading to falls. Parkinson’s dementia also can shorten your lifespan.
Studies have found pneumonia, cerebrovascular disease (diseases that affect the blood vessels of the brain — a common form of this disease is a stroke) and heart disease are the most common causes of death in people with Parkinson’s disease, though it’s unclear if or how the latter two are caused by Parkinson’s.22
Other factors may also have an impact. One study found people with Parkinson’s disease with what’s considered “normal” thinking, processing and memory abilities had a normal life expectancy. On the other hand, people with mild difficulties in their ability to think and process information, a “freezing” walking pattern, loss of smell, and high white blood cell count in the fluid in their brain and spine had a shorter life expectancy.2
Overall, research on the effect of Parkinson’s on mortality is mixed. One study found death rates in people with Parkinson’s are about two times higher than the general population, although no significant difference is found for those under age 65.26 Another study found on average, people with Parkinson’s die just one year earlier than the general population.20 In general, it’s commonly said you die “with” Parkinson’s, not “because” of Parkinson’s.
Learn more about Parkinson’s: Overview | Diagnosis | Treatment | Resources


Sources
- Armstrong, R. A. (2011). Visual Symptoms in Parkinson’s Disease. Parkinson’s Disease. doi:10.4061/2011/908306
- Bäckström, D., Granåsen, G., Domellöf, M. E., Linder, J., Mo, S. J., Riklund, K., . . . Forsgren, L. (2018). Early predictors of mortality in parkinsonism and Parkinson disease. Neurology,91(22). doi:10.1212/wnl.0000000000006576
- Bronner, G., & Vodusek, D. B. (2011). Management of sexual dysfunction in Parkinson’s disease. Therapeutic Advances in Neurological Disorders,4(6), 375-383. doi:10.1177/1756285611411504
- De Leon, M. (2019). [E-mail interview].
- Dementia. (n.d.). Retrieved May 31, 2019, from https://www.parkinsons.org.uk/information-and-support/dementia
- Doherty, K. M., Can de Warrenburg, B. P., Peralta, M., Silveira-Moriyama, L., Azulay, J., Gershanik, O. S., & Bloem, B. R. (2011). Postural deformities in Parkinson’s disease. The Lancet Neurology. doi:10.1016/S1474-4422(11)70067-9
- Eagles, M. (2019, April 23). [E-mail interview].
- Ferguson, L. W., Rajput, A. H., & Rajput, A. (2015). Early-onset vs. Late-onset Parkinson’s disease: A Clinical-pathological Study. Canadian Journal of Neurological Sciences / Journal Canadien Des Sciences Neurologiques,43(1), 113-119. doi:10.1017/cjn.2015.244
- Goetz, C. G., Tilley, B. C., Shaftman, S. R., Stebbins, G. T., Fahn, S., Martinez-Martin, P., . . . LaPelle, N. for the Movement Disorder Society UPDRS Task Force (2008). Movement Disorder Society-Sponsored Revision of the Unified Parkinson’s Disease Rating Scale (MDS-UPDRS): Scale Presentation and Clinimetric Testing Results. Movement Disorders,23(15), 2129-2170. doi:10.1002/mds.22340
- Goldman, J. (2019, May 3). [Telephone interview].
- Goldman, J. (2019, June 12). [E-mail interview].
- Hoehn, M. M., & Yahr, M. D. (1967). Parkinsonism: Onset, progression, and mortality. Neurology,17(5), 427-427. doi:10.1212/wnl.17.5.427
- Malaty, I. (2019, May 13). [Telephone interview].
- Marsh, L. (2013). Depression and Parkinson’s Disease: Current Knowledge. Current Neurology and Neuroscience Reports,13(12). doi:10.1007/s11910-013-0409-5
- McKeown, M. (2019, May 6). [Telephone interview].
- Moawad, H. (2018, October 08). Identifying Prodromal Parkinson Disease. Retrieved from https://www.neurologytimes.com/mds-congress/identifying-prodromal-parkinson-disease
- Pagano, G., Ferrara, N., Brooks, D. J., & Pavese, N. (2016). Age at onset and Parkinson disease phenotype. Neurology,86(15), 1400-1407. doi:10.1212/wnl.0000000000002461
- Postuma, R. B., Iranzo, A., Hu, M., Hogl, B., Boeve, B. F., Manni, R., . . . Pelletier, A. (2019). Risk and predictors of dementia and parkinsonism in idiopathic REM sleep behaviour disorder: A multicentre study. Brain,142(3), 744-759. doi:https://doi.org/10.1093/brain/awz030
- Robb, K. (2019). [E-mail interview].
- Savica, R., Grossardt, B. R., Bower, J. H., Ahlskog, J. E., Boeve, B. F., Graff-Radford, J., . . . Mielke, M. M. (2017). Survival and Causes of Death Among People With Clinically Diagnosed Synucleinopathies With Parkinsonism. JAMA Neurology,74(7), 839-846. doi:10.1001/jamaneurol.2017.0603
- Schrempf, W., Brandt, M., Storch, A., & Reichmann, H. (2014). Sleep disorders in Parkinson’s disease. Journal of Parkinson’s Disease,4(2), 211-221. doi:10.3233/JPD-130301
- Scorza, F., Carmo, A., Fiorini, A., Nejm, M., Scorza, C., Finsterer, J., & Ferraz, H. (2017). Sudden unexpected death in Parkinson’s disease (SUDPAR): A review of publications since the decade of the brain. Clinics,72(11), 649-651. doi:10.6061/clinics/2017(11)01
- Tagliati, M. (2019, April 25). [Telephone interview].
- Tanner, C., Albers, K., Goldman, S., Fross, R., Leimpeter, A., Klingman, J., & Eeden, S. V. (2012). Seborrheic Dermatitis and Risk of Future Parkinsons Disease (PD) (S42.001). Neurology,78(Meeting Abstracts 1). doi:10.1212/wnl.78.1_meetingabstracts.s42.001
- Wu, T., Zhang, J., Hallett, M., Feng, T., Hou, Y., & Chan, P. (2016). Neural correlates underlying micrographia in Parkinson’s disease. Brain,139(1), 144-160. doi:10.1093/brain/awv319
- Xu, J., Gong, D., Man, C., & Fan, Y. (2014). Parkinsons disease and risk of mortality: Meta-analysis and systematic review. Acta Neurologica Scandinavica,129(2), 71-79. doi:10.1111/ane.12201
- Yang, L. (2019, May 3). [Telephone interview].

