26 Photos That Show How Autoimmune Disease Can Affect Your Skin
Autoimmune diseases come in a variety of forms, each affecting different organs and bodily systems and producing a unique array of symptoms. While some of these symptoms may be “invisible,” skin manifestations can often be one of the most visible and telltale signs of autoimmune disease.
“Autoimmune diseases are conditions where the immune system, which is primarily designed to protect the body from infections such as bacteria and viruses, by attacking and destroying them, becomes confused and and will attack the body itself,” Cynthia Aranow, M.D., professor at the Feinstein Institutes Lupus Center of Excellence, told The Mighty. “The skin is an organ that is commonly attacked and affected.”
The skin issues caused by autoimmune disease are as varied as the individuals with the condition. They come in all shapes, sizes, colors, and textures, and can appear anywhere from your head to your toes. Some may have autoimmune disorders that primarily affect the skin, such as psoriasis, dermatomyositis, scleroderma, or epidermolysis bullosa. Others may experience skin issues as a symptom of one of the 100+ identified autoimmune diseases, or as a side effect of medication.
Though skin manifestations are often quite visible, there isn’t enough awareness about these symptoms, and this can lead to hurtful judgments and misconceptions. Many people (medical professionals included) see rashes, sores or lesions and automatically assume you’re contagious. But even if you explain to someone that no, you’re not contagious, many still shy away in disgust. The lack of understanding can be so frustrating and hurtful.
We wanted to raise awareness of the ways autoimmune disease can manifest on the skin, so we asked our Mighty community to share a photo showing how their skin has been affected. By helping others better understand what these symptoms can look like and what it’s like to live with them, hopefully we can reduce the judgment and stigma surrounding skin issues, while also advocating for quicker diagnoses and better treatments.
Here’s what the community shared with us:
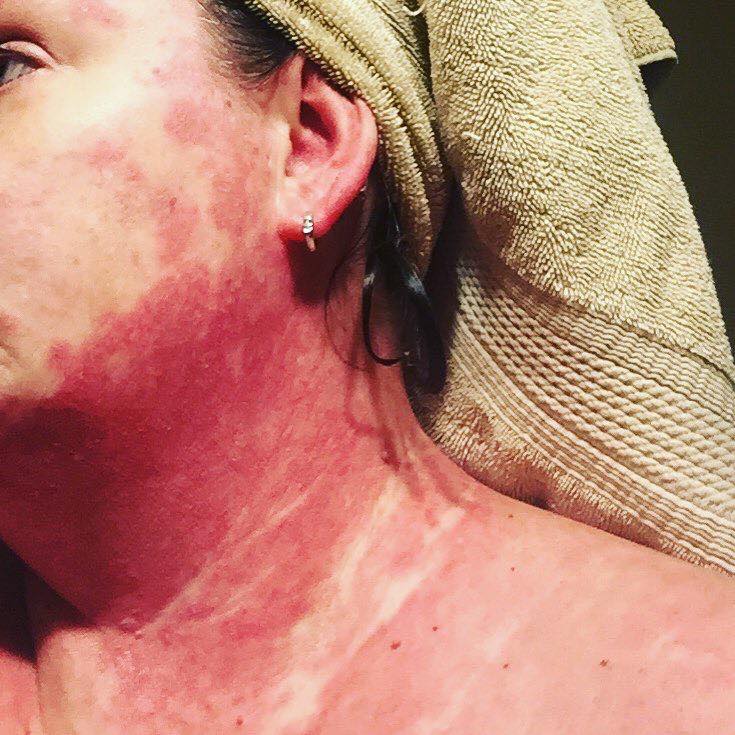
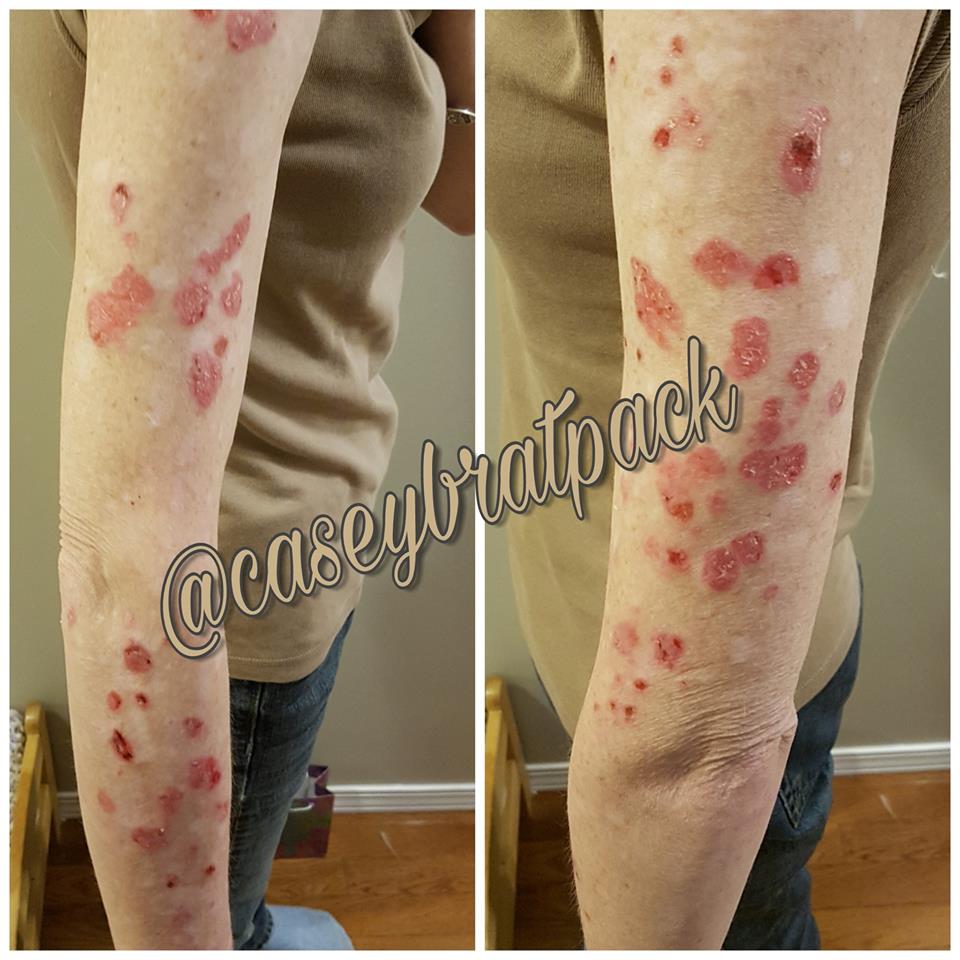
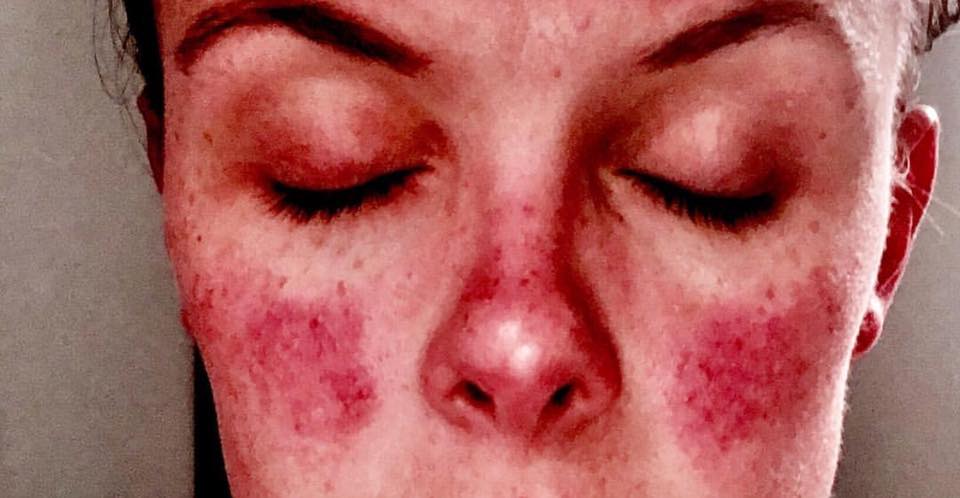
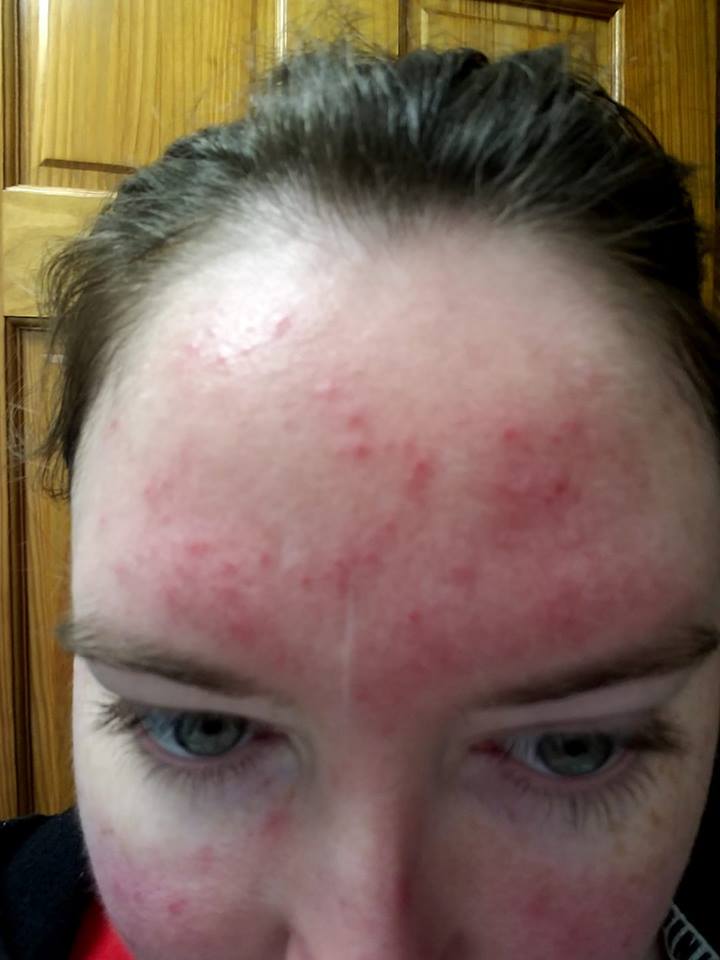
1. “My DLE [discoid lupus erythematosus] in full flare.” – Meghan E.C.
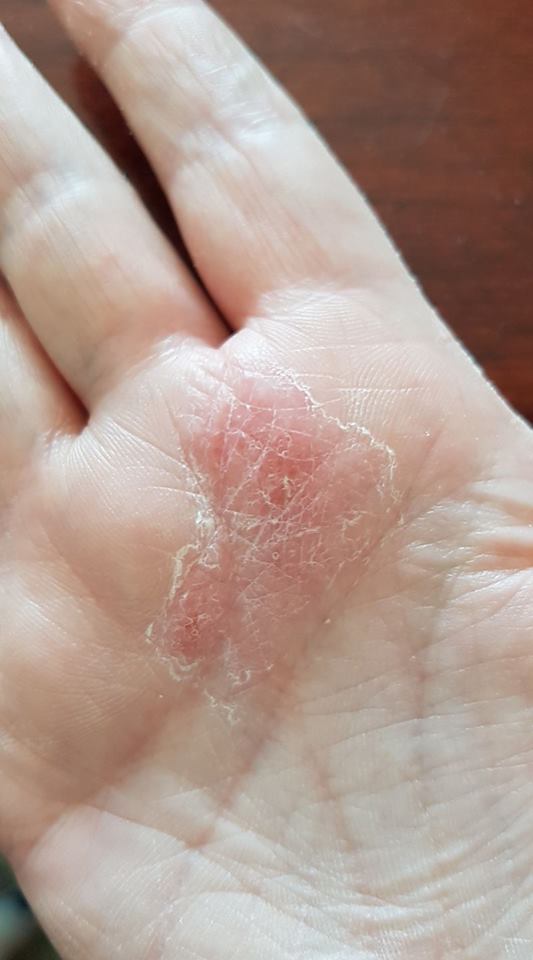
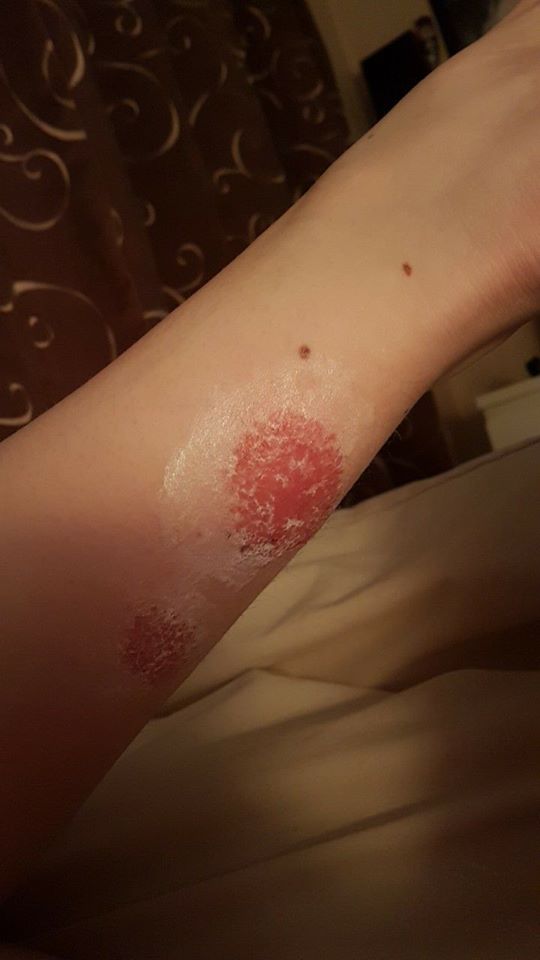
2. “Psoriasis brought on by stress.” – Lori C.
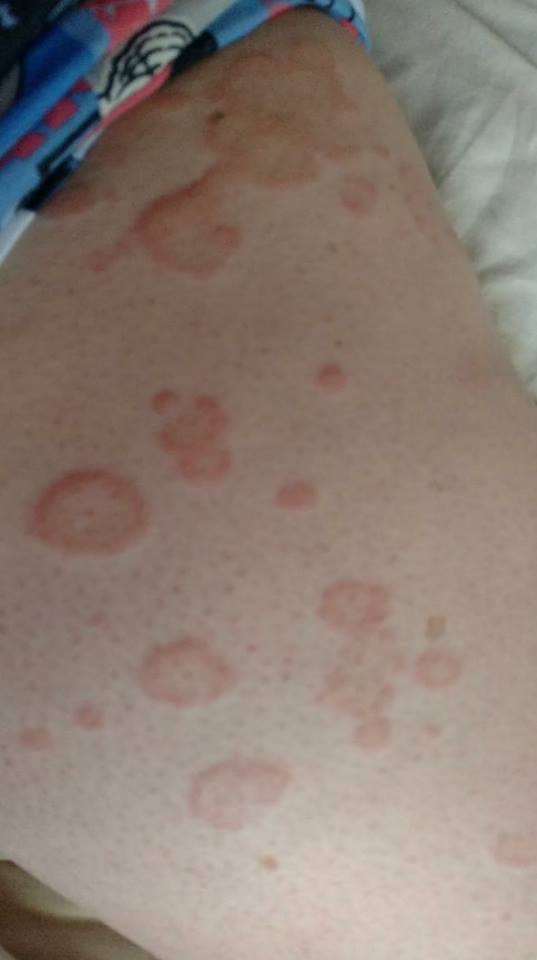
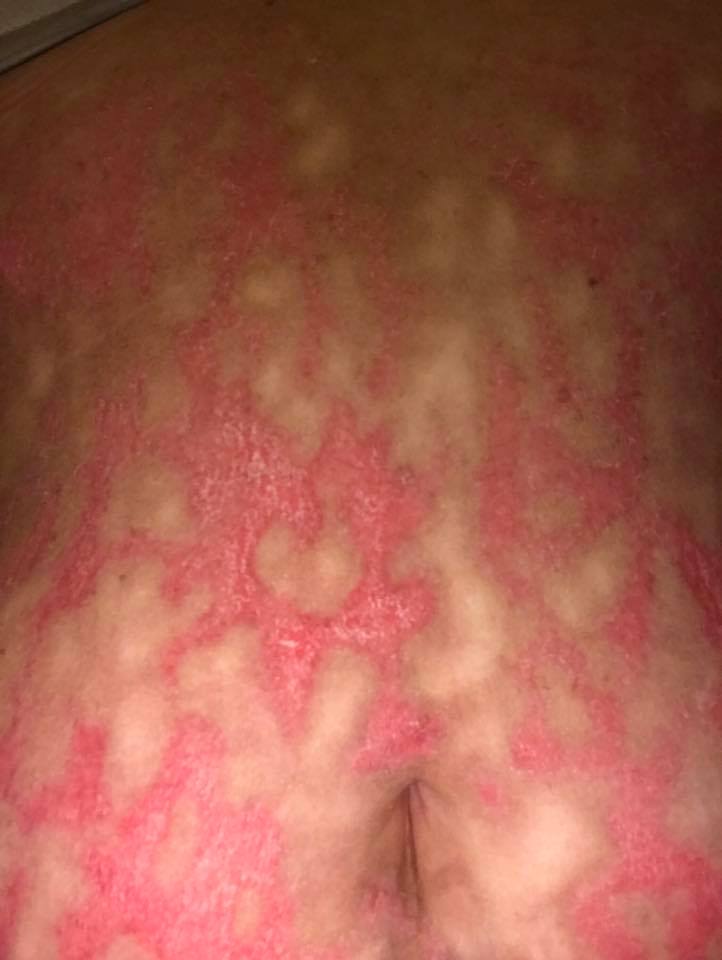
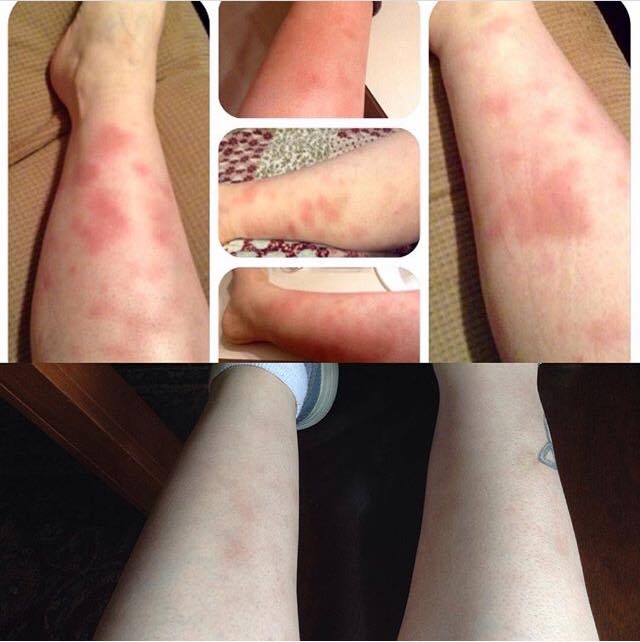
3. “I was finally diagnosed with undifferentiated connective tissue disease and autoimmune urticaria six months ago although this rash first appeared two years ago. This is my upper thigh although it is a generalized rash. These raised areas do not itch but they are horribly painful and burn (nerve pain), like I’m being stung by dozens of jellyfish constantly.” – Allison E.
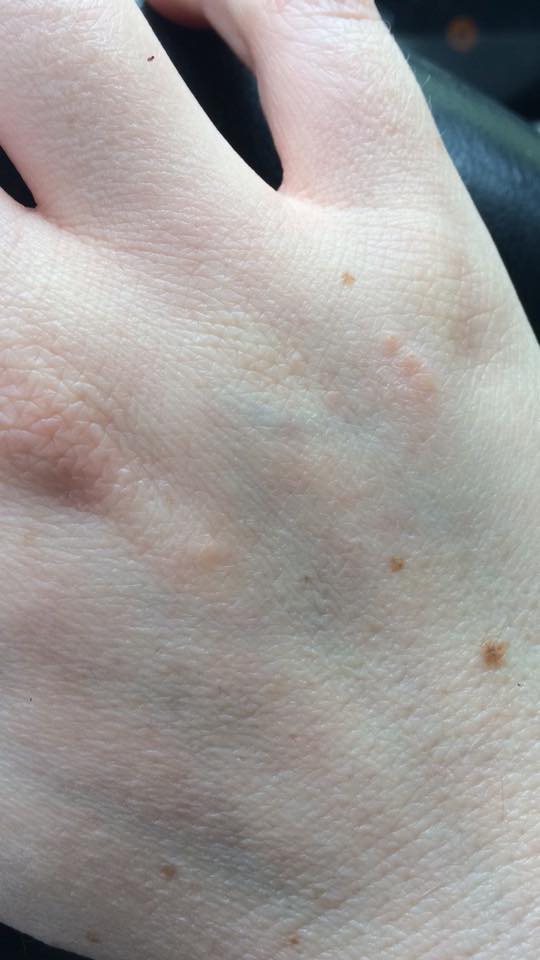
4. “You might not be able to see it due to my dark skin tone, but this picture was taken right after I got out of the hospital for the third time due to lupus-related incidents. Due to my ‘flare-ups’ going out of control, I started to get freckles on my nose. At first, I was really embarrassed by them. People at work would ask me about how I ‘suddenly got freckles.’ I couldn’t tell them without going into my whole lupus sob story, and it’s not really something I wanted to be known at work. It wasn’t until I met an old co-worker for lunch and she told me how ‘freckles fit my quirky personality.’ From that moment on, I decided not to hide my freckles any longer. I took this picture and posted them proudly. What’s weird is, I actually miss having them.” – Sidney D.
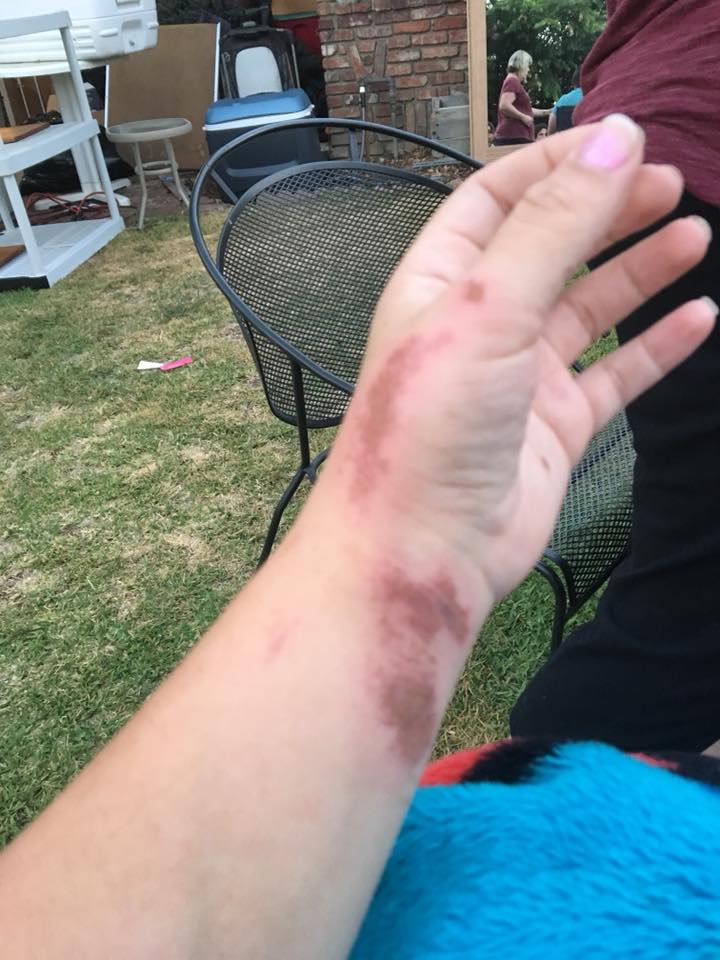
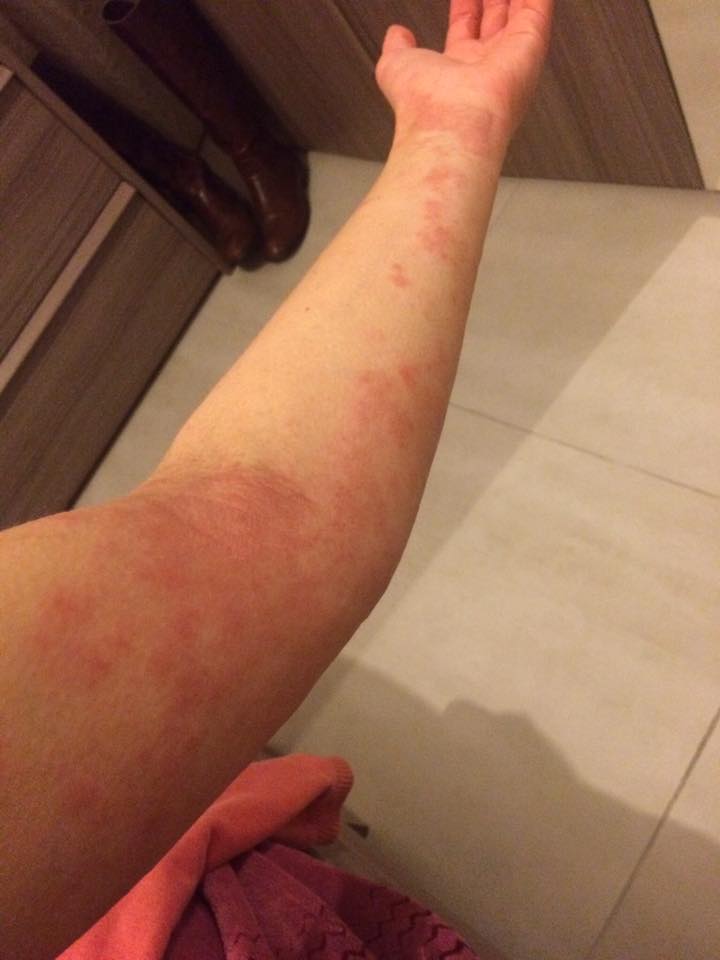
5. “Essentially an allergic reaction of two medications which made it essentially a chemical burn from the inside out! So so so painful! I had it on both hands, arm pits, back on my knees, even on my face! Rheumatoid disease problems!” – Jessie Z.O.
6. “I have several autoimmune conditions but they trigger Raynaud’s and it’s actually painful inside when this happens.” – Bianca P.M.
7. “Both arms, chest, upper back legs, behind ears, fingers… subacute cutaneous lupus (confirmation via biopsy). Never really ‘bothered’ me much in the past but now the sores drive me batty.” – Tricia M.C.
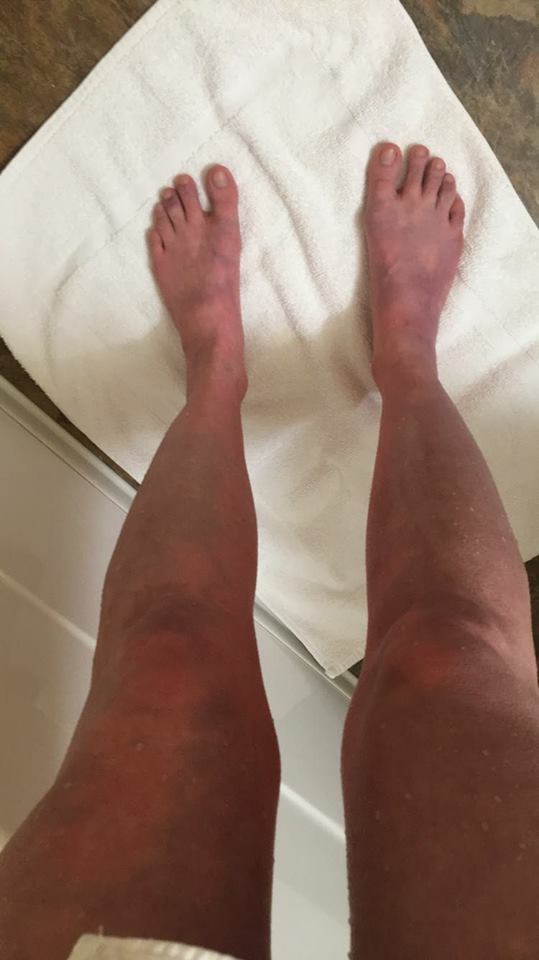
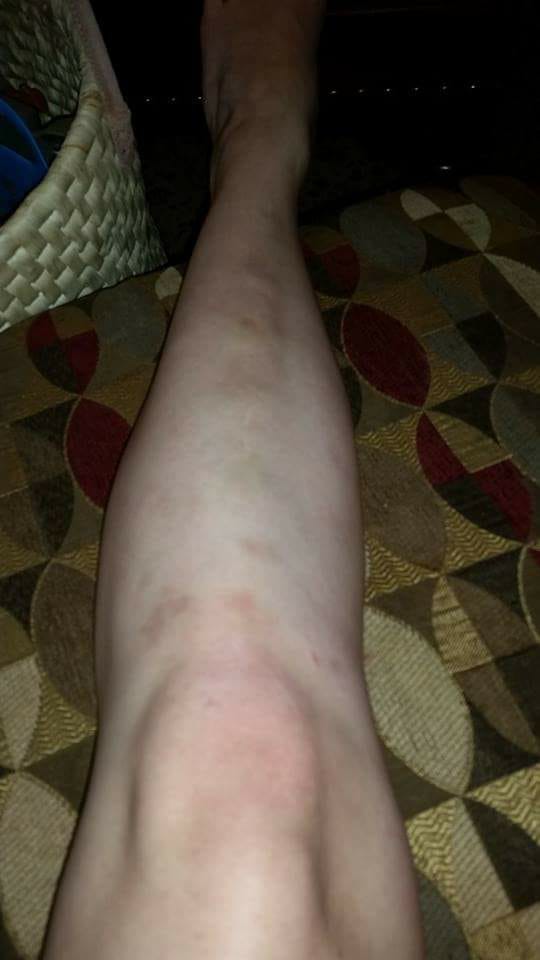
8. “Due to my postural orthostatic tachycardia syndrome (POTS), this is the color it turns when the blood pools in my legs. Bright red and dark purple.” – Melany M.
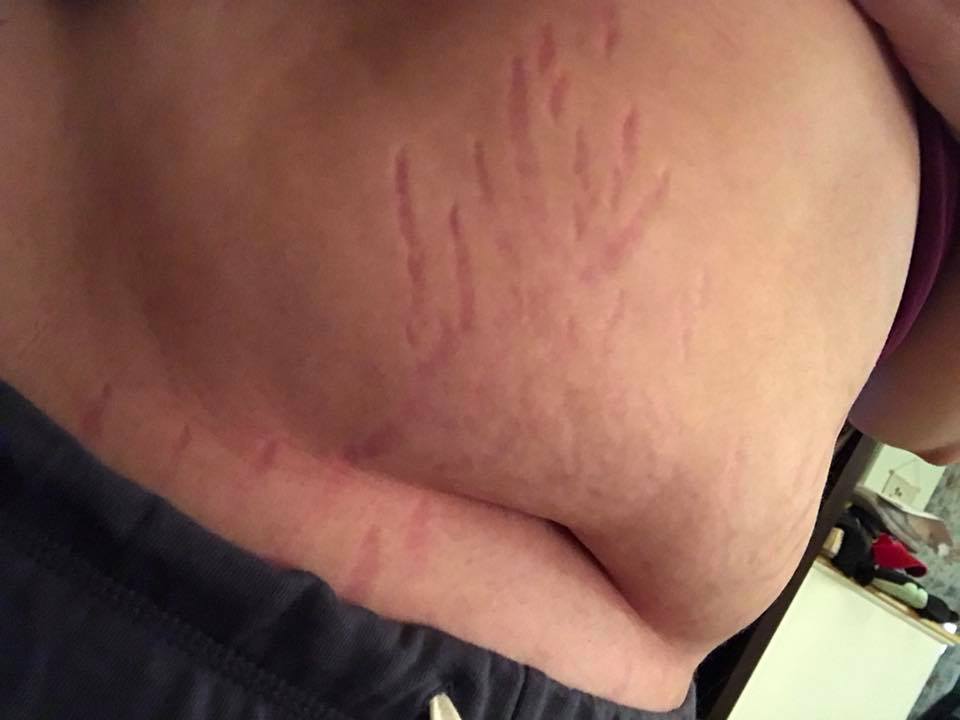
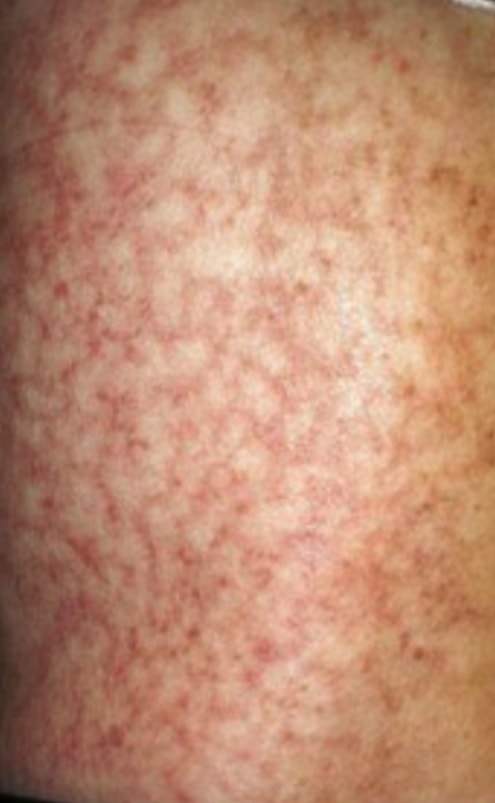
9. “Lyme, babesia or bartonella… I don’t remember which one causes what anymore. But I have gained weight and these horrible red streaks – I thought they were stretch marks but apparently this is a token symptom of one of my diseases.” – Kathryn B.
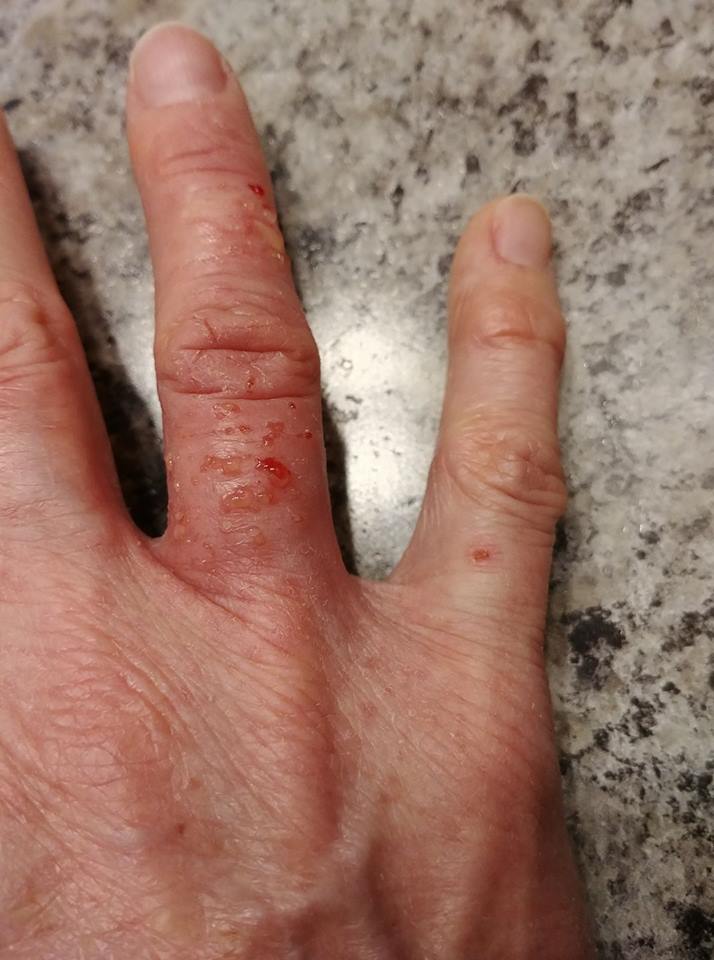
10. “Very painful, swollen, red, pussing, flared up cracking, fingers… been dealing for quite awhile. Doc prescribed prednisone, helped just a bit… came back. Anyone else dealing with this?” – Karen B.
11. “The photo here shows me when I was on prednisone steroids for my ulcerative colitis (left). I had a bloated face and terrible acne from the treatment. I’ve also seen how my autoimmune disease can affect me with white spots and rashes on the face, wrists and next to my stoma (what remains of my intestines that sticks out of my stomach).” – Saleem J.
12. “Today is a good day, so my skin isn’t too bad. I have Hashimoto’s. Dry skin makes my hands look much older than my 28 years and eating anything my thyroid doesn’t like causes an itchy red rash that sticks around for weeks.” – Megan P.
13. “Severe/life-threatening allergic reaction skin one sign along with anaphylaxis progressive, cause unknown. Autoimmune rapidly spreading across body.” – Dayna-Elyssia C.
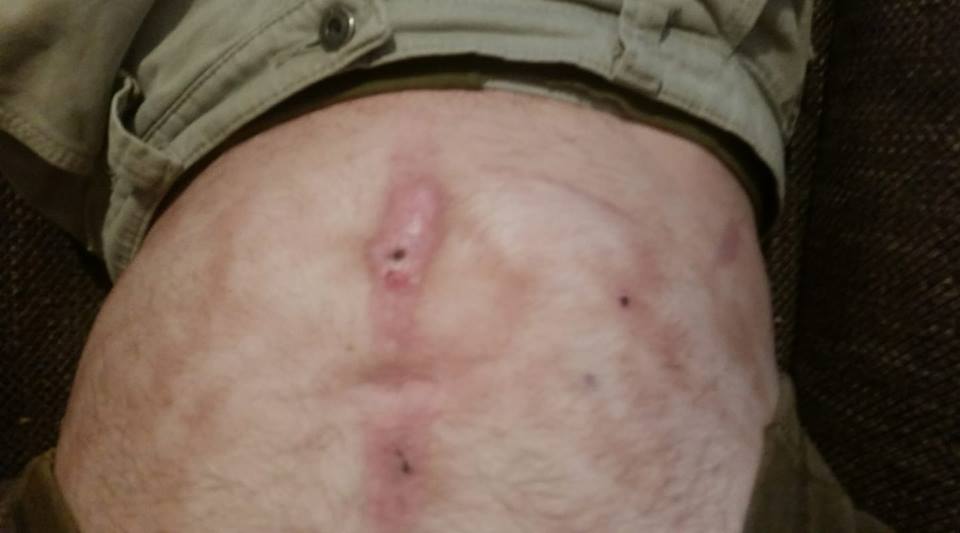
14. “I have lupus and antiphospholipid syndrome (APS). They have caused me to have livedoid vasculopathy all over my body. This is a picture of my stomach. It’s where I have it the worst. It’s due to the blood vessels collapsing and not bringing the blood supply my skin needs. It’s also happening to my internal organs and my brain. I don’t share this on Facebook and I keep my super noticeable areas covered because people look at it like it’s gross and treat me like I’m contagious. Even nurses and doctors look at it with disgust and touch me with ‘icky fingers.’ I constantly have to tell people who see it, ‘Don’t worry! It’s not contagious. It’s just my blood supply shutting down to parts of my body. If anyone should be worried, it’s me!’ It’s on my arms, legs, chest, and starting on my face. It’s getting harder to hide. It’s the only visible part of my invisible illnesses. I wish people understood that I’m not contagious and that their facial expressions sometimes hurts more than the skin pain.” – Jennifer M.
15. “When my lupus flares or I get stressed out I develop not only a malar rash but also raised painful rashes. My face feels hot, like it’s on fire, tight from swelling, and painful. It will spread to other areas of my body as well.” – Amy P.A.
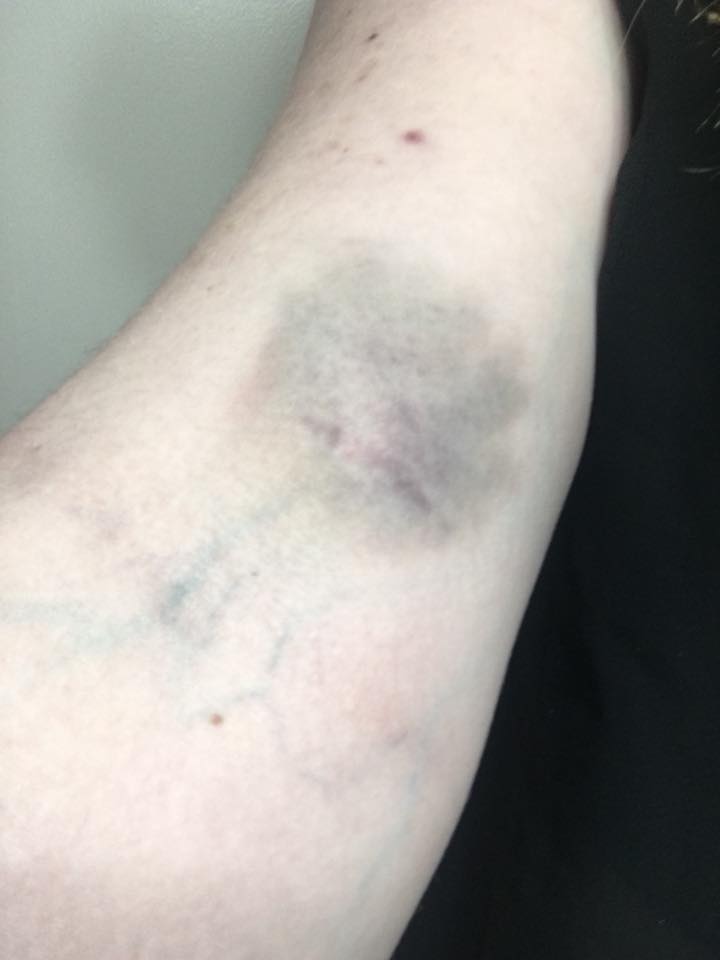
16. “Extreme bruising due to an undiagnosed autoimmune disease. This one was due to an IV, but I get ones like this all the time.” – Amber B.
17. “This is me. I have an undiagnosed autoimmune disease. I have hypo- and hyper-pigmentation as a result. My face is several different shades. There really isn’t anything to hide it, unless I want to wear really thick makeup.” – Kathy A.
18. “This is not a sunburn. This is a rash covering my entire arm. There were other places affected by it as well (ears, face, legs from the knee down, anything I had exposed to the sunlight). This happens every time I am in the sun. On this day, I was in it for over eight hours for a softball tournament. Sunblock doesn’t help. But like I said, it’s not a burn, but a horrible itchy rash.” – Stephanie D.
19. “Skin discoloration from overuse of a heat pad. And scabs from my belly being distended.” – Lance S.
20. “This is my malar rash when I’m flaring. It used to be one connected flush and now it’s turned to raised patches and a flush over my nose.” – Emily C.
21. “I had chronic erythema nodosum (EN) for two and a half years from Crohn’s disease. I didn’t present like a typical case at first so it took months to convince my doctors that I was sure it was EN. It took changing treatments, then doubling the dose and increasing frequency to finally clear up. What a nightmare! I’ve recently started seeing a couple very faint spots coming back on one leg, hopefully it doesn’t progress any further.” – Julia C.
22. “(Covered in Sudocrem.) Random patches appeared like this on my legs and my gastro said it’s a common occurrence with Crohn’s disease… Two months and countless prednisolone tablets on, they’re getting worse and more have popped up on my legs (mainly) and stomach. Off to the hospital tomorrow for more treatment options as they’re so sore and oozy.” – Amy G.
23. “Before I got diagnosed with rheumatoid arthritis (RA), my legs looked like this. My dermatologist said that it was called erythema nodosum and that it was common in autoimmune diseases. It was really itchy and raised. It eventually cleared up with prednisone but left bruising up and down my legs. Prior to being diagnosed with RA, I had been diagnosed with a different disorder, so being in pain wasn’t alarming. These marks were my eye opener and eventually why I was diagnosed.” – Juliana W.
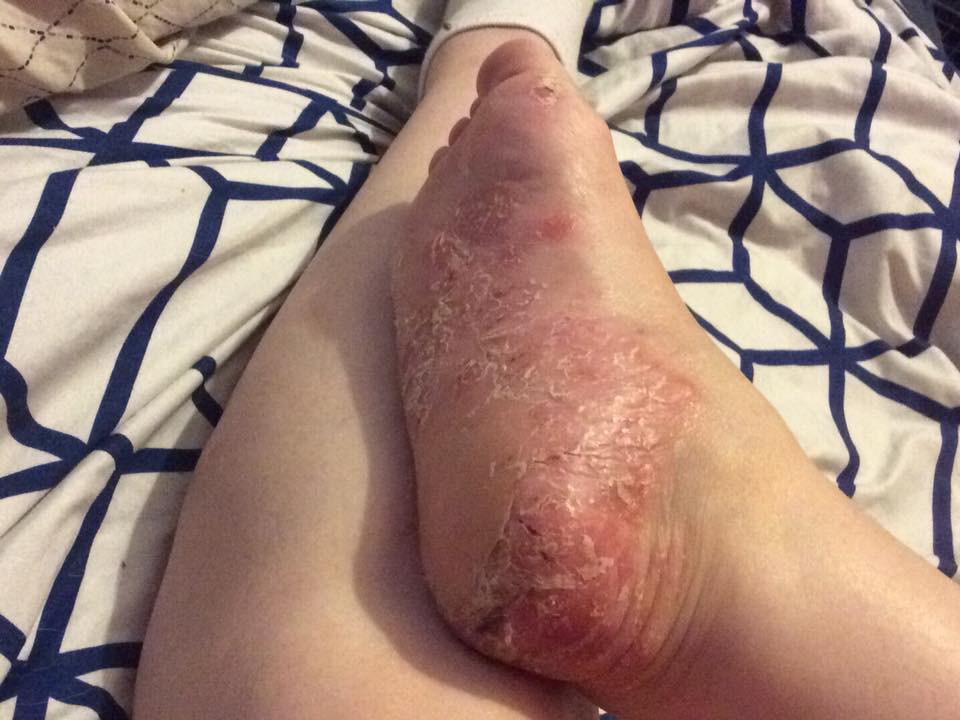
24. “Psoriasis on the soles of my feet. I have to wear socks all the time so I don’t leave blood everywhere. The heels especially crack and bleed. I stopped taking my RA immune suppressants for a surgery and all of a sudden this blooms on my feet. I had no idea a skin condition could be so painful.” – Karen J.
25. “The lovely roadmap on my back and legs…” – Shannon G.M.
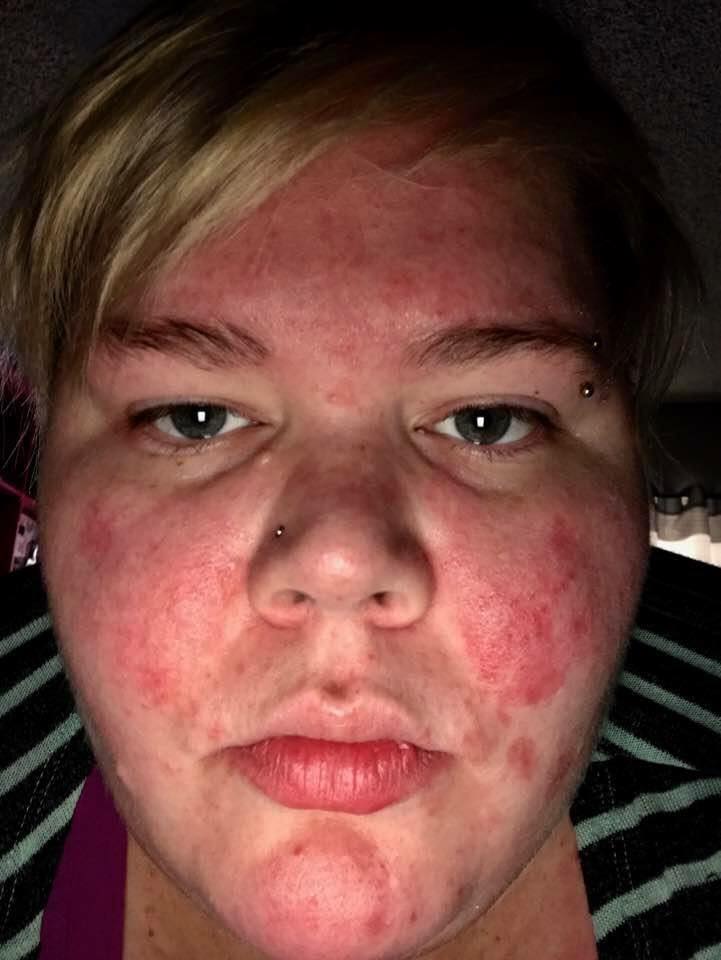
26. “Rosacea caused by a lupus flare-up. Thousands of little blisters, all over my face, at least one week out of every month. They burn and itch like crazy. The medication my dermatologist gave me helps clear it up faster, but does nothing to help the burning pain. It’s basically a week of hell every time it flares up.” – Patricia H.
If you’re struggling with skin issues because of your chronic illness, know you’re not alone. Talk with your doctor about the skin-related symptoms you’re experiencing to find out what treatments might be available to help.
“Treatment depends on both the extent of skin involvement as well as the underlying autoimmune disease,” Dr. Aranow shared. “In general, topical creams and ointments are the first line of therapy. Other therapies used in more severe conditions include pills or injections.”