I’m new here!
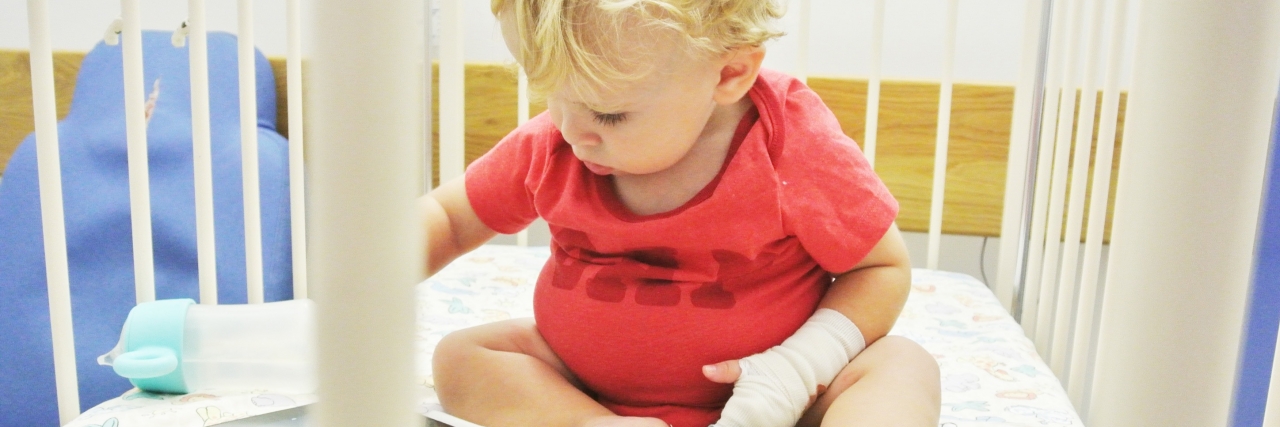
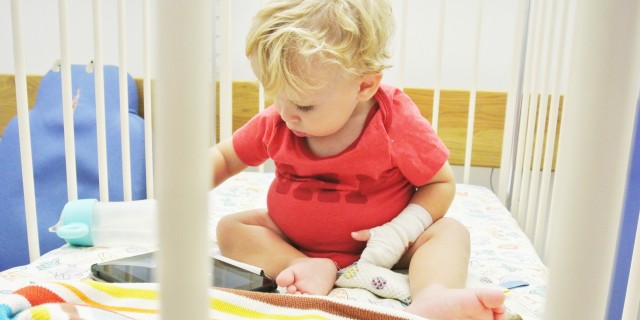
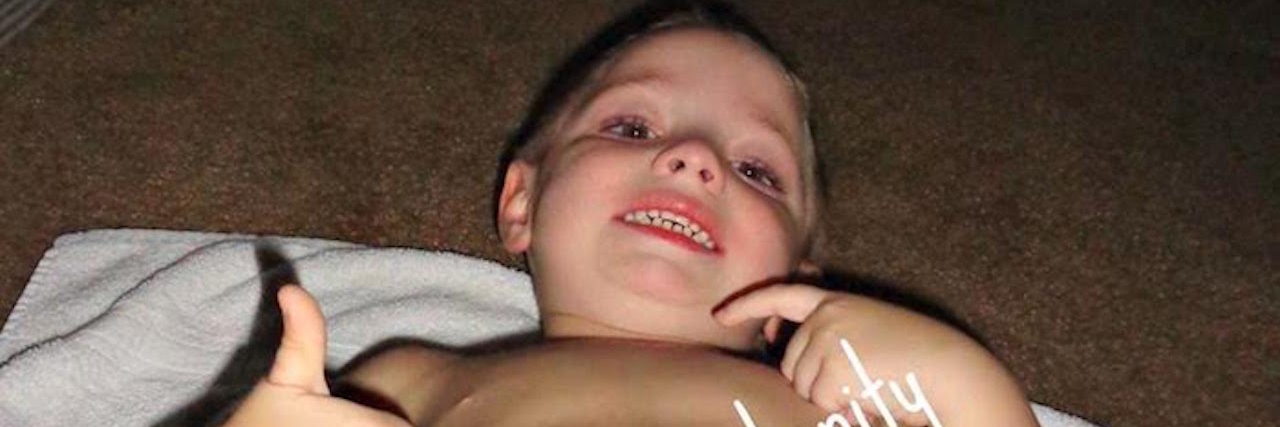
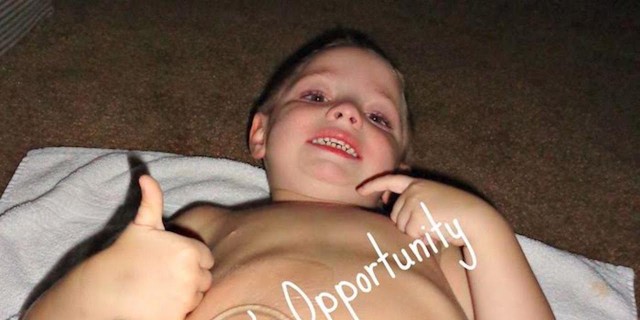
Hi, my name is jped. I'm here because I was born with Prune Belly Syndrome and have many other illnesses that have stemmed from it. I am here to be a voice, advocate, and supporter. I have been a lifelong medical patient.
#MightyTogether #ChronicKidneyDisease #complexpost-traumaticStressDisorder #Gastroparesis #Hyperparathyroidism #Anxiety #Depression