Epidermolysis Bullosa
Epidermolysis Bullosa
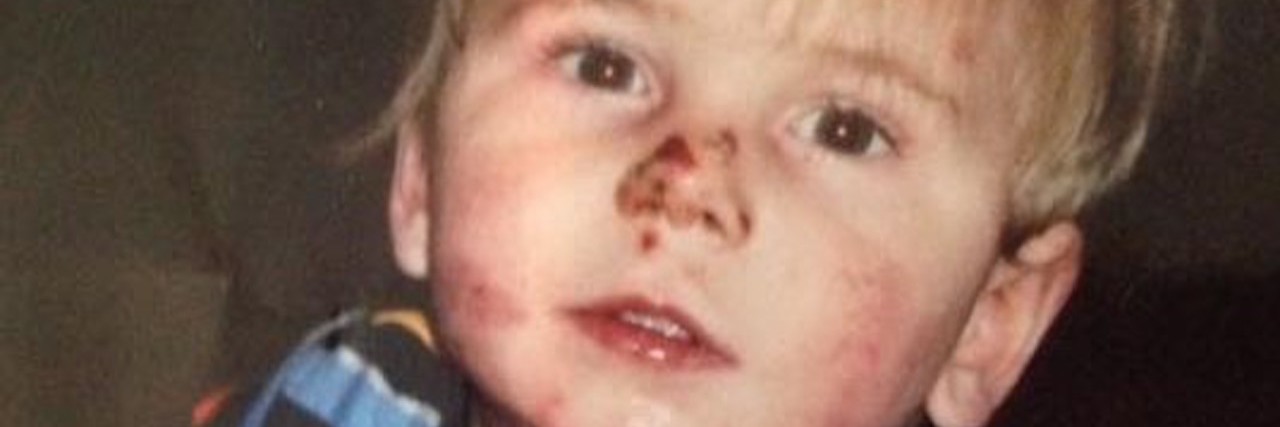
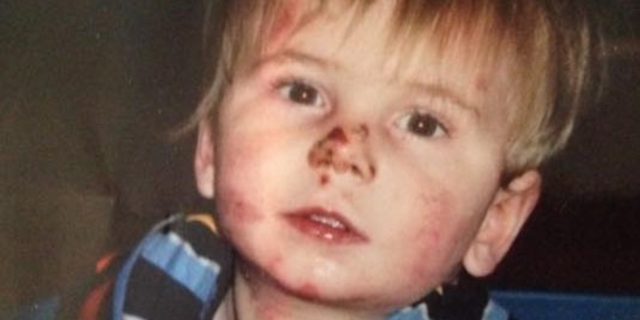
Epidermolysis Bullosa is a rare genetic skin disease that causes a person to have extremely fragile skin that blisters and tears easily from minor friction or trauma. It is often present at birth and sometimes people who have it even earn the nickname "butterfly children. Last but not least, treatment for people with this rare skin disease includes ongoing painful and time-consuming tasks like meticulous wound care, special dressings changes, and taking antibiotics for infection. Oh and other treatments for people who have this rare and painful skin condition includes pain management, nutritional support, preventing injury by wearing loose clothes and sometimes doing possible new gene therapies that offer hope.