I’m new here!
Hi, my name is Charles. I'm here because I want to find out food treatment for hypertension
Hi, my name is Charles. I'm here because I want to find out food treatment for hypertension
I want to post something that’s light compared to the last one, and just to perhaps have some fun on this kinda internal joke I have. I say “I won the gene lottery” for the worst genes!
It’s not very sad to live with it for me, perhaps because I grew up in an environment so bad I had to learn to adapt fast, which makes me going blind not suffer so much though after 5 years actively dealing with constant spurts of vision loss, I finally feel some grief.
But really if I would list… disabilities? Well, ASD and blindness are together. Very likely to have won the ADHD gene too but I didn’t get to test yet because of money and because the overall test checks for ASD, ADHD and “being Gifted” and I’m already proven to have ASD and a “Gifted Brain” so I don’t want to pay a lot of money right now just to check if ADHD is here too. Now eyes? Congenital cataracts with retinal dystrophy followed by partial ophthalmoplegia, partial lagophthalmos, nocturnal lagophthalmos, light strabism and an amblyopic eye that never worked until some weeks ago and activated because my dominant eye got to the useless bar. Also was lucky to win the myopia and astigmatism genes but those are common in society. Then there’s the very specific genes from each of my parents… heart disease and hypertension weren’t on my bingo card until I actually got to a point where I apparently earned it from my dad. Then a very aggressive gastritis from my mum, and also coming from her… loose ligaments and double joint.
Aside from my effed mental health that is more mine than anyone else’s, I basically won the gene pool. I try laughing about it because if I’d cry for all of it I’d be even more miserable, but what most of that brings me isn’t the grief really, it’s a free ticket for being constantly annoyed and tired, always in fatigue and although my patience is almost endless, I do get frustrated and annoyed by having to go doctor after doctor trying to solve my issues, adjust medications, and overall, trying to find an ophthalmologist who actually will effing listen to me on testing for Retinitis Pigmentosa Sine Pigmento because I have all the symptoms, but nothing is visible on my retina, and that’s why this kind of RP I mentioned, is called “Sine Pigmento” (If you didn’t understand the term, it’s Latin for “without pigment”)
Hi, my name is LoreasaurusRex. I've been diagnosed with Long Covid, idiopathic tachycardia, idiopathic radiculopathy, hypertension, hypothyroid, PCOS… I’m anxious about starting a new prescription for gabapentin.
Hi, my name is sickofbeingsick. I've been diagnosed with severe GERD/acid reflux. Even prilosec isn’t helping. My throat & esophagus have been swollen for 7 days & I’m scared. I’m barely eating or drinking. Even plain water causes swelling & acid. I’ve had to sleep sitting straight upright for 7 nights.
#MightyTogether #Anxiety #Depression #ADHD #PTSD #OCD #Grief #Hypertension
Yesterday I met with my gynecologist to discuss different birth control methods. She wants me to stop taking estrogen due to hypertension and interactions with certain meds I’m on. We discussed the iud, implant, shot, and proestrogen only pill. I’m use to having periods only every 3 months and their lighter. Don’t want periods every month nor intermittent spotting. I got put on birth control for my pmdd and to help with bad cramping 20 years ago. I get yeast infections easily espically in the summer with excessive sweating. I don’t want weight gain. I’m already obese and having hard time losing. I already have depression and anxiety along with other health conditions including pots. Don’t want increased risk of breast cancer. It runs in my family. My pots is always worse when I’m on my period making me more dizzy and feeling like I’m going to faint more along with worse nausea. I have back pain but it’s worse when on my period along with bloating. I’m torn between the shot and implant. I have been doing research and both sound good except the weight gain with the shot. I have pain management procedures every couple of months besides other procedures, bloodwork, scans, etc. please help me decide between the shot and implant! #MajorDepressiveDisorder #GeneralizedAnxietyDisorder #PremenstrualDysphoricDisorder #POTS #ReflexSympatheticDystrophySyndrome
I experienced abnormal heart palpitations and fatigue during childhood football games. At 18, symptoms worsened (extreme fatigue climbing stairs, heavy head, and pounding heartbeat). Diagnosed with severely high blood pressure I was prescribed Telmisartan and a low-salt diet.
While medication initially helped, new symptoms emerged a year later: dizziness and near-fainting when standing quickly. Accidentally, I ate ~1kg of bitter lupin beans seasoned with sumac and salt over two days. Surprisingly, my blood pressure symptoms dramatically improved I stopped medication entirely.
After three months, mild symptoms returned. I repeated the lupin/sumac treatment, and symptoms disappeared again. For over 1.0.0.5 years, I’ve remained medication-free with only rare mild head pressure during stress. I share this hoping it helps others.
Hi, my name is Milodogboxer. I'm here because I'm depressed and am in a loveless 43 year relationship though he thinks all is peachy keen. He's built a wall, and to top it all off, in denial about his health... recently started metformin for type 2 diabetes, had a stent put in, high blood pressure, high cholesterol, 64 years old, drinks 5 plus days a week
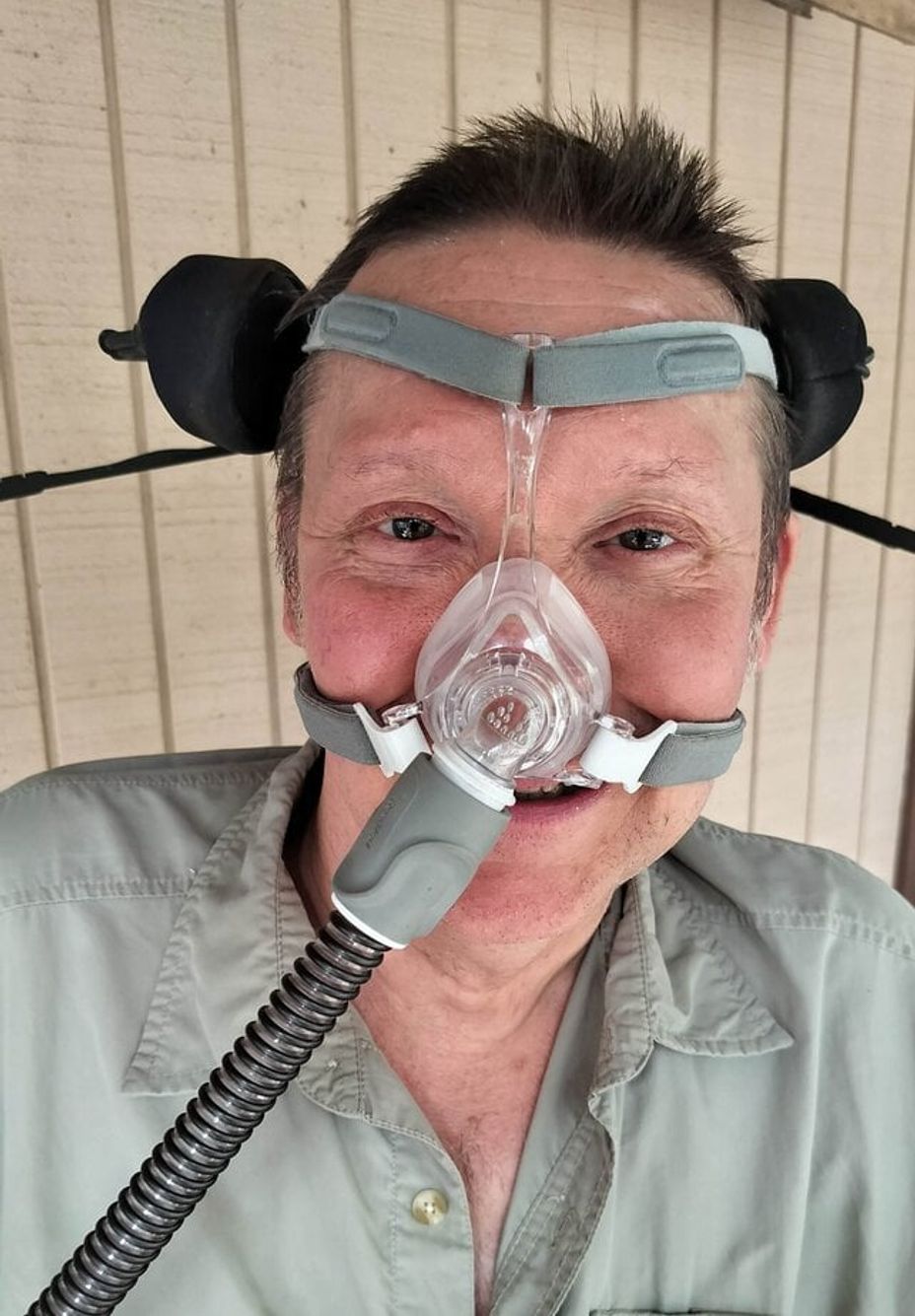
When my neuro prescribed CPAP, I thought, "ANOTHER THING!" But it was totally worthwhile: After my first full night with the CPAP, my daily 20-minute nap disappeared, and I haven’t taken one since.
Many of us don't realize we have treatable sleep apnea because we deal with so many other problems that we assume are the cause for our poor sleep, says Dr. Abdulghani Sankari, pulmonologist at Detroit's DMC DRH Sleep Disorders Center.
“They have pain issues, they have urinary issues, they have cardiovascular issues … They’re tired and not able to sleep well because of all these factors,” he says, “so they don’t recognize that there are other reasons … [why] they feel tired during the day.” CPAP/BiPAP often addresses manifested symptoms like daytime listlessness, waking up unrefreshed from sleep, and unexplained chronic pain. CPAP/BiPAP also helps improve aspects of sleep-affected cognition: memory, forgetfulness, attention span and intellectual abilities like troubleshooting problems effectively.
Letting these problems linger can even cause our condition to worsen. “The frequent interruption of breathing at night leads to what we call chronic intermittent hypoxia, so the body is exposed to low levels of oxygen, and that produces byproducts of inflammation and waste that [aggravate] symptoms on the central nervous system,” Sankari says. Unchecked sleep apnea is also a risk factor for high blood pressure, heart problems and type 2 diabetes. CPAP is an effective treatment for sleep apnea. Got questions? Pls contact me.
Better Nights, Better Days: CPAP, BiPAP and Disability
#fatigue #MultipleSclerosis #MightyTogether #ChronicIllness #autoimmune #newlydiagnosed #Disability #Caregiving

Hi, my name is PinkPachederm. I'm here because I have several autoimmune issues: Reynards, Sjogrens, Fibromyalgia, CAD, Arthritis, Migraines, Chronic Fatigue - as we know is a symptom of all the aforementioned diseases. Then for some extra fun I have Neuropathy in my hands & feet, carpal tunnel in both hands, something else in my thumbs - can't remember the name, and Glaucoma. High blood pressure, though not too bad, is kept under control, as is cholesterol. I am in constant pain somewhere in my body every day if not all over. I can tell when the weather will change by my barometric migraines which are as bad as regular migraines. The regimen of daily pills & healthy diet can sometimes get frustrating when a flare up occurs & the meds for it just put me to sleep. I detest having to cancel plans due to a flare up or migraine so severe I can not function.
So, I am here to see if there really are like pained people. Sometimes I think I am going crazy with all this pain & all these issues. Is there anyone else experiencing all of this???

Hi, I’m Tamanna — a new voice here, but one with a thousand stories stitched into her smile.
This week, I write not just for myself, but for every soul silently surviving — the nurses who cry in hospital stairwells, the mothers reheating tea they never finish, the strong women who smile while breaking inside. You see, I’ve been all of them. Still am.
There were days I held a dying father’s hand in one shift, then came home to rock my baby to sleep with shaky arms. I’ve stood under fluorescent hospital lights wondering if anyone saw me beyond the stethoscope and headscarf. But in every crack, I found poetry.
So here’s my truth — dramatic, flawed, funny even:
I’ve diagnosed heartbreak faster than hypertension.
I’ve Googled “how to cry quietly” in hospital washrooms.
I’ve laughed too hard at memes at 3 a.m. to feel less alone.
And once, I prescribed myself sleep. It didn’t work. Laughter did.
This week, I’m choosing healing. Not hustle. Not hollow praise. Just healing — for myself, my children, and everyone who reads this and whispers “me too.”
Because maybe our mess is the medicine.
So here’s my Mighty pep talk to you (and to me):
Rest, warrior. Breathe. Let the tea go cold. You are not late — you are blooming on divine timing.
Write that blog, post that story, say your truth out loud. Your voice is powerful, your pain is valid, and your softness is sacred.
I’m here now. New to this group, but not new to surviving. Let’s hold space for each other. And hey — if you cried, smiled, or felt a flicker of “me too,” hit that heart, drop a comment, or just exhale. That’s how we keep going.
With love and laughter,
Dr. Tamanna Islam Nishat
Writer | Doctor | Mental Health Advocate
#motherhoodunfiltered #burnoutsurvivor #faithinmedicine #womenwhowrite #healingwithwords #mightynewmember #VoiceOfTheWhiteCoat