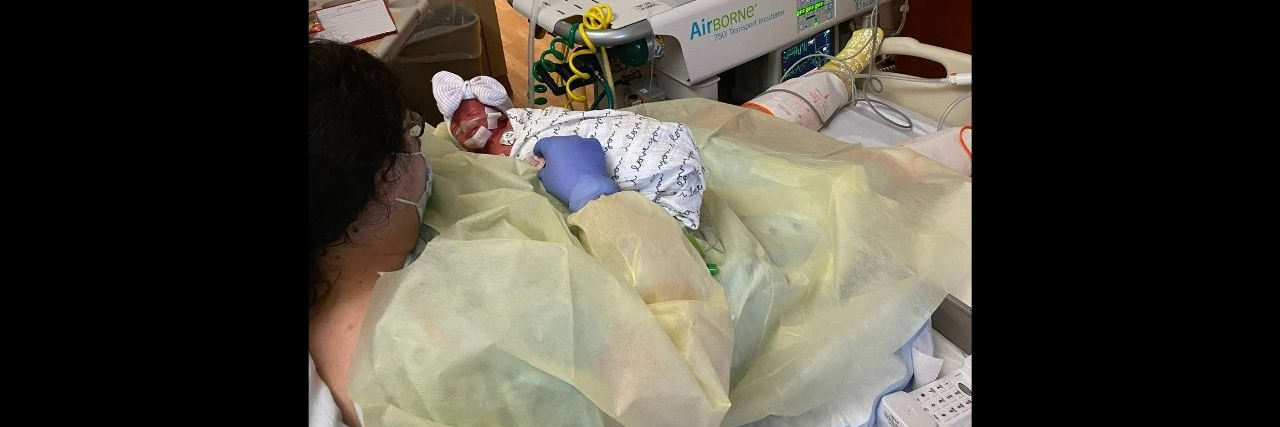
If you have ever experienced psychosis, you are probably aware that what you KNOW and what you BELIEVE are two very different things.
All throughout my pregnancy, from beginning to now (he was about about four weeks old at the time of writing) I have had trouble bonding, connecting, and otherwise believing in my son’s existence.
Which, truly, is worrisome and slightly terrifying.
Is this just some elaborate hallucination? That’s what my brain tells me.
From the first visit at the birthing center where I shared my concerns with the midwives that this pregnancy wasn’t “real” – it was one of those pregnancies where I went through the whole process physically, but with no baby at the end – to during labor when he finally emerged and I kept asking “is he real?”, this whole experience has yet to connect properly in my brain.
The trauma after birth didn’t help matters – between a huge blood clot, hemorrhaging, and postpartum preeclampsia – but recovery is a work in progress.
How I Cope with the Psychosis:
-I’ve surrounded myself with support, for one. There is rarely a time when no one is available to help
-Breastfeeding, cuddling my son, and skin to skin contact don’t make my son feel any more real, but they do seem to help keep my psychosis from getting worse.
-Honesty with my care team (midwives, psychiatrist, and probably a therapist soon) about what is happening so I can be properly cared for and medicated as needed
-Walking away (with my son left in good hands) when needed is invaluable. Although I have not in any way felt aggression or anger towards my son, sometimes a meltdown happens, and it’s easier to recover from a meltdown when you AREN’T holding a crying infant.
Next Steps:
As hard as it is to gather the motivation to breastfeed and otherwise care for an infant that my brain tells me doesn’t truly exist, I rely on my support system (primarily the people I live with) to help encourage and push me to do what needs to be done. When I simply cannot function, communication with my support people is key.
If you are going through something similar, please, surround yourself with as many supportive people that you can be fully open and honest with as you can. Their help can make or break your pregnancy and later your ability to function when caring for your newborn.
Have you gone through a pregnancy or birth while experiencing psychosis? Were you able to properly bond with your child later? Please let me know in the comments. I’m still holding out hope that this mental state isn’t forever.